Double Uterus: Symptoms, Causes & Treatment in Canada
Share
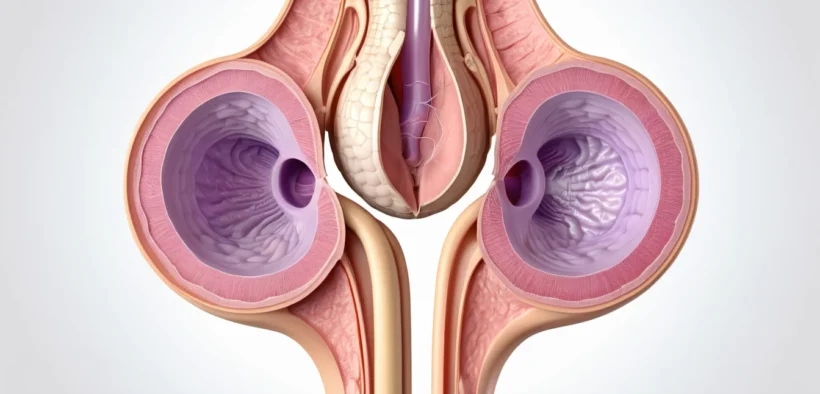
A double uterus is a rare congenital condition where a woman is born with two separate uterine cavities instead of one. Many Canadian women live with this condition their entire lives without ever knowing, as it often produces no noticeable symptoms. However, for some women, a double uterus can significantly affect pregnancy outcomes and overall reproductive health.
Understanding Double Uterus: Causes and Risk Factors
Also known as uterus didelphys, this uterine abnormality develops during fetal growth when the two small tubes that normally fuse to form the uterus fail to merge completely. While many women experience no complications, others may face challenges such as recurrent miscarriage or preterm birth. Understanding the symptoms and causes of this condition can help Canadian women know when to speak with their family doctor or specialist for proper diagnosis and care.
What Is a Double Uterus?
| Anomaly Type | Key Characteristics | Associated Symptoms | Management Approach |
|---|---|---|---|
| Uterine Didelphys (True Double Uterus) | Two completely separate uterine cavities, two cervixes, and often a divided vagina | Painful periods, abnormal bleeding, recurrent pregnancy loss | Regular monitoring; surgical correction considered if recurrent miscarriage occurs |
| Bicornuate Uterus | Single cervix with a heart-shaped uterus divided into two horns at the top | Pelvic pain, preterm labour, abnormal fetal positioning | Metroplasty (Strassman procedure) in select cases; close obstetric monitoring |
| Septate Uterus | Single uterus divided internally by a fibrous or muscular septum; most common Müllerian anomaly | Recurrent miscarriage, preterm birth, menstrual irregularities | Hysteroscopic septum resection; associated with best surgical outcomes |
| Arcuate Uterus | Mild indentation at the top of the uterine cavity; considered a normal variant by many specialists | Usually asymptomatic; rarely linked to late pregnancy loss | Typically no treatment required; monitoring during pregnancy recommended |
| Unicornuate Uterus | Only one fully developed uterine horn; may have a small rudimentary horn on one side | Endometriosis, ectopic pregnancy risk, preterm labour | Removal of rudimentary horn if causing pain or obstruction; high-risk obstetric care |
During fetal development, the uterus forms from two small tubes. Normally, these tubes merge to create a single, hollow organ. In some cases, the tubes do not fully join together. Instead, each tube develops on its own, forming a double uterus — a condition also called uterus didelphys.
Each cavity in a double uterus often has its own cervix. Some women also have a divided or double vagina. This condition is more common among women who have experienced recurrent miscarriage or premature birth. However, many women with a double uterus never experience any complications at all.
You can learn more about uterine development from the Mayo Clinic’s overview of double uterus.
Double Uterus Symptoms to Watch For
Many women with a double uterus have no symptoms whatsoever. The condition is often discovered by accident during a routine pelvic exam or prenatal ultrasound. In fact, some women only find out after experiencing repeated pregnancy losses.
However, some women do notice signs. It is important to pay attention to changes in your menstrual cycle or pelvic region. Possible symptoms of a double uterus include:
- Unusual pain before or during your menstrual period
- Abnormal bleeding during your menstrual cycle
- Repeated miscarriages
- Premature labour
If you notice any of these symptoms, do not ignore them. Speak with your family doctor or visit a walk-in clinic for an initial assessment.
What Causes a Double Uterus?
Researchers have not yet identified a single clear cause for a double uterus. The condition develops before birth, during early fetal development. It appears to happen when the two small tubes that normally form the uterus fail to fuse together properly.
Interestingly, a double uterus is often found alongside kidney abnormalities. This suggests that one underlying factor may affect the development of both organs at the same time. Genetic factors may also play a role, though more research is still needed.
For more background on how uterine abnormalities develop, visit Healthline’s guide to uterus didelphys.
Possible Complications of a Double Uterus
Many women with a double uterus lead completely normal lives. They have healthy sex lives, become pregnant, and give birth without any issues. However, for some women, complications can arise.
Pregnancy and Fertility Concerns
A double uterus can sometimes contribute to fertility challenges. In addition, the condition may increase the risk of miscarriage, particularly recurrent miscarriage. Women with a double uterus may also experience premature labour or unusual positioning of the baby during pregnancy.
It is important to note that many women with a double uterus do carry pregnancies to full term. With the right medical support, a healthy pregnancy is entirely possible. Your obstetrician can help you build a care plan that reduces your risks.
Other Uterine Abnormalities
A double uterus is one of several types of uterine abnormalities. Other structural differences in the uterus can also affect fertility and pregnancy. Therefore, getting an accurate diagnosis is an important first step in understanding your reproductive health.
How Is a Double Uterus Diagnosed?
A double uterus is often discovered during a routine pelvic exam. Your doctor may notice a double cervix or feel an unusual uterine shape. If a uterine abnormality is suspected, your doctor will likely recommend one or more imaging tests.
Ultrasound
An ultrasound uses high-frequency sound waves to create images of the inside of your body. A device called a transducer is used to capture these images. The transducer can be placed on the skin of your abdomen or inserted into the vagina (called a transvaginal ultrasound). Both methods provide clear, useful images of the uterus.
For an abdominal ultrasound, you may be asked to drink a certain amount of water beforehand. This helps the uterus show up more clearly on the screen.
MRI (Magnetic Resonance Imaging)
An MRI uses a magnetic field and radio waves to create detailed cross-sectional images of the inside of your body. It does not use radiation. Usually, no special preparation is needed before an MRI.
However, the MRI machine is quite loud and the space inside is narrow. If you feel uncomfortable in enclosed spaces or with loud noises, let your doctor know ahead of time. A mild sedative can be prescribed to help you feel more at ease during the scan.
When to See a Doctor About a Double Uterus
If you are experiencing unusual pelvic pain, abnormal bleeding, or repeated miscarriages, it is time to speak with a healthcare provider. You can start by booking an appointment with your family doctor. If you do not have a family doctor, a walk-in clinic can provide an initial assessment and refer you to the right specialist.
Early diagnosis matters, especially if you are planning a pregnancy or have already experienced pregnancy loss. Your doctor may refer you to an obstetrician or a gynaecologist for further testing and care. Together, you can create a plan that gives you the best chance at a healthy pregnancy.
If you have already been diagnosed with a double uterus and are planning to have a child, make sure your obstetric team knows. Open communication with your care team — whether through your provincial health plan or a specialist referral — is essential for the best outcome.
As always, this article is for general information only. Please consult your doctor or a qualified healthcare provider for advice specific to your situation.
Preparing for Your Appointment
When you visit your doctor about a possible double uterus, a little preparation goes a long way. Being ready helps your appointment run smoothly and ensures you get the most useful information.
What to Bring and Do Before Your Visit
- Write down all your symptoms, including when they started and how long they last
- Make a list of all medications, vitamins, and supplements you currently take
- Note any past pregnancies and how they progressed
- Ask the clinic ahead of time if any preparation is needed before tests
- Bring a trusted family member or friend for support — they may remember details you forget
Questions to Ask Your Doctor
Do not hesitate to ask your doctor questions during your appointment. You might want to ask:
- What is the most likely cause of my symptoms?
- Do I need surgery, and why or why not?
- What treatment options are available through my provincial health plan?
- Should I see a specialist such as a gynaecologist or reproductive endocrinologist?
- What reliable resources do you recommend for more information?
Your doctor will also likely ask you questions. Be ready to describe your menstrual cycle, any past pregnancies, and your plans for future pregnancies. Honest and detailed answers help your doctor give you the best possible care.
For more information on reproductive health in Canada, visit Health Canada’s official health information page.
Can you get pregnant with a double uterus?
Yes, many women with a double uterus do become pregnant and carry their babies to full term. However, the condition can increase the risk of miscarriage, premature birth, or unusual fetal positioning. Working closely with an obstetrician gives you the best chance of a healthy pregnancy.
What are the symptoms of a double uterus?
Many women with a double uterus have no symptoms at all and never know they have the condition. Some women may experience unusual pelvic pain, abnormal menstrual bleeding, or repeated miscarriages. If you notice any of these signs, speak with your family doctor or visit a walk-in clinic.
Is a double uterus hereditary?
The exact cause of a double uterus is not fully understood, and researchers have not confirmed a clear hereditary link. The condition develops before birth when the two tubes that form the uterus fail to merge properly. Genetic factors may play a role, but more research is needed to confirm this.
Does a double uterus require surgery?
Surgery is not always necessary for a double uterus. Treatment is only recommended when the condition causes symptoms such as severe pelvic pain or recurrent miscarriages. Your gynaecologist or obstetrician can help you decide whether surgery or another form of treatment is right for you.
How is a double uterus diagnosed in Canada?
A double uterus is often found during a routine pelvic exam when a doctor notices an unusual uterine shape or a double cervix. Your doctor may then order an ultrasound or MRI to confirm the diagnosis. These tests are generally covered under provincial health plans when medically necessary.
Can a double uterus cause miscarriage?
According to Mayo Clinic’s overview of double uterus, this information is supported by current medical research.
For more information, read our guide on urinary incontinence and other pelvic health concerns in Canada.
Yes, a double uterus can increase the risk of miscarriage, particularly recurrent miscarriage. The condition may also lead to premature birth or complications during pregnancy. However, many women with a double uterus do have successful pregnancies with appropriate medical care and monitoring.
Key Takeaways
- A double uterus (uterus didelphys) is a rare condition where the uterus has two separate cavities instead of one
- Many women with a double uterus have no symptoms and never receive a diagnosis
- Possible symptoms include unusual pelvic pain, abnormal menstrual bleeding, and recurrent miscarriage
- The exact cause is unknown, but the condition often occurs alongside kidney abnormalities
- Diagnosis is usually made through a pelvic exam, ultrasound, or MRI
- Treatment is only needed when the condition causes symptoms or complications
- Many women with a double uterus have healthy pregnancies with the right medical support
- If you are concerned, speak with your family doctor, visit a walk-in clinic, or ask for a referral to a gynaecologist through your provincial health plan
Frequently Asked Questions
What is a double uterus?
A double uterus is a rare congenital condition where a female is born with two separate uterine cavities instead of one. It develops when the Müllerian ducts fail to fuse properly during fetal development. Each uterus may have its own cervix and connect to a divided or normal vagina.
What are the symptoms of a double uterus?
Many people with a double uterus experience no symptoms at all. When symptoms occur, they may include abnormal or heavy menstrual bleeding, painful periods, repeated miscarriages, premature labour, and pelvic pain. Some women only discover the condition during a routine pelvic exam or pregnancy ultrasound.
Can a double uterus affect pregnancy in Canada?
Yes, a double uterus can increase pregnancy risks, including preterm birth, miscarriage, breech positioning, and low birth weight. However, many Canadians with this condition carry pregnancies successfully. Close monitoring by an obstetrician and access to high-risk pregnancy care significantly improves outcomes for those affected.
How is a double uterus treated?
A double uterus often requires no treatment if it causes no symptoms or pregnancy complications. When intervention is needed, surgery such as a metroplasty may be recommended to improve fertility outcomes. Treatment decisions are individualized and typically made in consultation with a gynecologist or reproductive specialist based on symptoms and reproductive goals.
When should you see a doctor about a double uterus?
See a doctor if you experience recurrent miscarriages, unusually heavy or painful periods, difficulty conceiving, or pelvic pain. In Canada, a family doctor or gynecologist can refer you for imaging tests such as an ultrasound or MRI to diagnose uterine abnormalities and discuss appropriate next steps for your situation.
About the Author
Dr. Linda Chen, RD, PhDDr. Linda Chen is a registered dietitian and PhD in Nutritional Sciences from the University of British Columbia. With expertise in clinical nutrition, sports dietetics, and gut health, she has worked with leading Canadian hospitals and sports organizations. Dr. Chen is a member of Dietitians of Canada and regularly contributes to national nutrition policy discussions.
View all articles →