Neck Pain Causes: Treatment & Recovery Guide Canada
Share
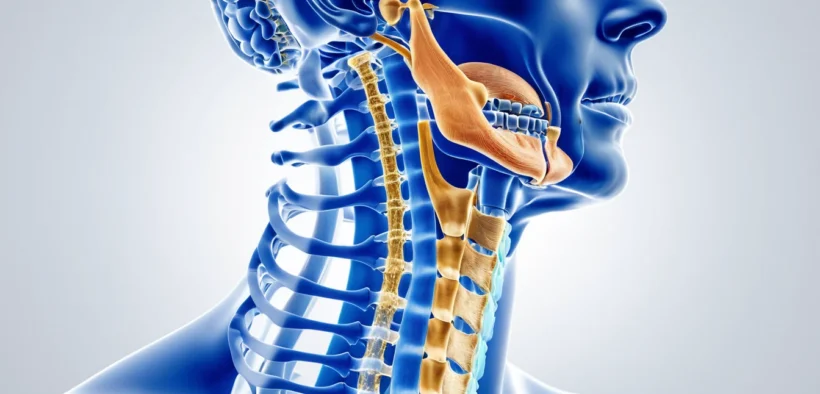
Neck pain causes range from simple muscle strain to serious nerve compression, and understanding them is the first step toward recovery. In Canada, neck pain is one of the most common health complaints — studies show that up to 80% of people will experience it at least once in their lifetime. A Canadian study found that 54% of the general population had neck pain in the past six months alone, and for 5% of those individuals, the pain was disabling.
Understanding the Most Common Neck Pain Causes
If you are currently dealing with cervical spine pain, you are far from alone. Whether your discomfort started after a long day at a desk, a sports injury, or seemingly out of nowhere, this article explains why neck pain happens, what symptoms to watch for, and the most effective neck pain treatment options available to Canadians. From exercises and physical therapy to injections and surgery, you will find the guidance you need to take control of your recovery.
How Is the Neck Structured?
| Type of Neck Pain | Common Characteristics | Typical Duration | Recommended Management |
|---|---|---|---|
| Muscle Strain & Tension | Stiffness, aching, tightness; often worsened by prolonged desk work or poor posture | Acute: days to 2 weeks | Rest, heat or ice therapy, gentle stretching, over-the-counter NSAIDs (e.g., ibuprofen) |
| Cervical Osteoarthritis | Gradual onset of pain and stiffness, grinding sensation, reduced range of motion; more common in adults over 50 | Chronic: months to years | Physiotherapy, low-impact exercise, pain management, possible corticosteroid injections |
| Herniated Cervical Disc | Sharp or burning pain that may radiate into the arm, numbness or tingling in fingers, muscle weakness | Subacute to chronic: weeks to months | Physiotherapy, traction, epidural steroid injections, surgery if conservative care fails |
| Whiplash Injury | Neck pain and stiffness following sudden impact (e.g., motor vehicle accident), headache, dizziness, fatigue | Acute to subacute: days to 12 weeks | Active mobilization, physiotherapy, pain relief medications; avoid prolonged immobilization |
| Cervical Radiculopathy | Nerve root compression causing radiating pain, weakness, or numbness down one arm; may include reflex changes | Variable: weeks to months | Physiotherapy, nerve-specific exercises, medications (gabapentin, NSAIDs), possible surgical referral |
| Meningitis-Related Neck Pain | Severe neck stiffness, high fever, sensitivity to light, headache; inability to touch chin to chest | Acute: requires emergency care | Immediate emergency medical attention — call 911 or visit the nearest emergency department |
Your neck, also called the cervical spine, is made up of seven small bones called vertebrae. It is the most mobile part of your entire spine. It lets you tilt, turn, and nod your head in many directions.
The cervical spine also helps you balance and plays a key role in your vision. Several structures in the neck can cause pain, including the vertebral bones, ligaments, intervertebral discs, joints, joint capsules, and the surrounding muscles. Understanding these structures helps explain why neck pain can feel so different from person to person.
Common Causes of Neck Pain
Neck pain has many causes, ranging from muscle strain to nerve compression. However, the most common causes fall into three main groups: overuse injuries, nerve root compression, and joint-related pain. Infections and tumours can also cause neck pain, but these are far less common.
Overuse and Strain
This is the most common type of neck pain, accounting for about 85% of all cases. It often develops after a car accident — especially a rear-end collision that causes a whiplash motion. It can also build up gradually from repetitive physical strain, poor posture, psychological stress, or working in the cold.
People who sit at a desk without armrests, or who use a keyboard placed too high, are especially at risk. So are workers who use their arms and shoulders heavily throughout the day. This type of neck pain typically limits how far you can move your head and makes everyday activities uncomfortable.
In addition to stiffness, overuse neck pain can disrupt your sleep. It may also come with dizziness, headaches, or nausea. Sometimes the pain spreads to the shoulders, shoulder blades, or the back of the head — even without any nerve involvement. For more information on how posture and workplace habits affect your neck, visit Health Canada’s wellness resources.
Radicular Neck Pain (Pinched Nerve)
Radicular pain happens when a nerve root in the cervical spine gets irritated or compressed. The most common cause is a herniated disc — when the soft cushion between two vertebrae bulges out and presses on a nearby nerve. Cervical spondylosis, a type of age-related joint wear, is the second most common cause.
With a herniated disc, you may feel intense neck pain that suddenly shoots down one arm. With cervical spondylosis, the pain tends to develop more slowly over time. The exact location of the pain depends on which nerve is affected. For example, a compressed nerve at C5–C6 can cause pain in the shoulder, deltoid muscle, and outer arm. A nerve at C7–C8 may cause pain in the forearm and fingers.
Beyond pain, you may also notice some muscle weakness in the arm or hand. This is usually mild, but it is important to monitor. Mayo Clinic offers a helpful overview of cervical spondylosis and its effects on the nerves.
Joint-Related Neck Pain
The small joints between your vertebrae — called facet joints — can also be a source of chronic neck pain. These joints absorb a lot of repeated stress over a lifetime. They are especially vulnerable after car accidents or from ongoing microtraumas.
The joints most often affected are at the C4–C5 and C5–C6 levels, where mechanical forces are greatest. A key feature of this type of pain is that you can often point to exactly where it hurts along the back of your neck. If this sounds familiar, speak with your family doctor or visit a walk-in clinic for an assessment.
Neck Pain Symptoms to Watch For
Neck pain can feel different depending on its cause. However, some symptoms are common across most types. Knowing what to watch for helps you describe your condition clearly to a healthcare provider.
- Stiffness or limited range of motion — difficulty turning or tilting your head
- Headaches — often starting at the base of the skull
- Dizziness or nausea — especially with overuse-type neck pain
- Pain that radiates to the shoulder or arm — may suggest nerve involvement
- Muscle weakness in the arm or hand — a sign that nerve compression may be more serious
- Tingling or numbness in the fingers — another possible sign of nerve root irritation
If you experience sudden, severe neck pain after a fall or accident, seek medical attention right away. Similarly, neck pain combined with fever, unexplained weight loss, or difficulty swallowing needs prompt evaluation.
Neck Pain Treatment Options
Regardless of the cause, the first goal of treatment is to reduce your pain. There are several effective options available, and your treatment plan may combine more than one approach.
Medications and Physical Therapies
Pain relievers and anti-inflammatory medications are often the first step. In some cases, muscle relaxants may also help, especially if muscle spasm is a major issue. These medications are usually available through your family doctor or after a visit to a walk-in clinic.
Physical therapies can work well alongside medication. These include therapeutic massage, heat and cold therapy, and physiotherapy techniques such as TENS (transcutaneous electrical nerve stimulation) and ultrasound therapy. Note that ultrasound therapy is generally not recommended for radicular neck pain, as it may worsen nerve irritation in some cases.
Wearing a soft cervical collar can provide short-term relief. However, most experts recommend using one for no more than 72 hours, as prolonged use can weaken neck muscles over time. For radicular pain specifically, avoiding activities that make your symptoms worse is an important part of early recovery.
Corticosteroid Injections
For joint-related neck pain caused by arthritis or facet joint degeneration, corticosteroid injections may help reduce inflammation and relieve symptoms. These are typically performed by a specialist and can provide meaningful relief when other treatments have not been enough. Your family doctor can provide a referral if this option is appropriate for you.
Surgery
Surgery is rarely needed for neck pain. However, if nerve compression is causing progressive muscle weakness that is getting worse, surgery may become necessary. This is considered when non-surgical treatments have failed and motor function is at risk. Your specialist will guide you through this decision if it applies to your situation.
Exercises for Neck Pain Recovery
Once your acute pain is under control, exercise is one of the most effective long-term treatments for neck pain. A Finnish study involving 180 patients showed that targeted neck exercises significantly outperformed standard pain management approaches. The study compared endurance-focused exercises with strength-focused exercises — both were more effective than relying on pain relief measures alone.
A physiotherapy programme for neck pain typically focuses on strengthening the muscles that support the cervical spine. It also works on improving balance, body awareness (proprioception), and correcting poor posture habits. These goals work together to reduce the risk of future flare-ups.
Some helpful exercises include gentle neck stretches, chin tucks, shoulder blade squeezes, and deep cervical flexor activation. However, always start an exercise programme under the guidance of a registered physiotherapist, especially if you have radicular symptoms or a recent injury. Healthline provides a practical guide to safe neck pain exercises you can discuss with your provider.
When to See a Doctor About Neck Pain
Most neck pain improves on its own within a few days to weeks. However, some situations call for professional care sooner rather than later. You should see your family doctor or visit a walk-in clinic if your neck pain:
- Lasts more than one to two weeks without improvement
- Is severe or getting progressively worse
- Radiates down your arm or causes tingling and numbness in your fingers
- Is accompanied by muscle weakness in your arm or hand
- Follows a car accident, fall, or sports injury
- Comes with fever, chills, unexplained weight loss, or difficulty swallowing
In Canada, your first point of contact for neck pain is usually your family doctor. They can assess your symptoms, order imaging if needed, and refer you to a physiotherapist, chiropractor, or specialist. If you do not have a family doctor, most provincial health plans cover walk-in clinic visits for this type of concern. Do not ignore worsening symptoms — early treatment leads to better outcomes.
Frequently Asked Questions About Neck Pain
What is the most common cause of neck pain?
The most common cause of neck pain is muscle and soft tissue strain from overuse, poor posture, or sudden movements like whiplash. This type of neck pain accounts for about 85% of all cases. It often improves with rest, heat or cold therapy, and gentle movement.
How long does neck pain usually last?
Most cases of neck pain from muscle strain or minor injury improve within a few days to two weeks. However, neck pain related to nerve compression or joint degeneration may last longer and require professional treatment. If your neck pain persists beyond two weeks, it is a good idea to see your family doctor.
Can neck pain cause headaches and dizziness?
Yes, neck pain can often come with headaches, dizziness, and even nausea — especially with overuse-type or whiplash-related injuries. This happens because the cervical spine plays a role in balance and has close connections to the structures at the base of the skull. These symptoms usually improve as the neck pain itself is treated.
Is exercise good or bad for neck pain?
Exercise is generally very beneficial for neck pain, especially once the acute phase has passed. Targeted strengthening and stretching exercises help stabilise the cervical spine, improve posture, and reduce the risk of future episodes. Always start a neck pain exercise programme with guidance from a registered physiotherapist.
When does neck pain require surgery?
Surgery for neck pain is rarely needed and is usually only considered when nerve compression is causing progressive muscle weakness that does not improve with other treatments. Most people with neck pain — even radicular neck pain from a herniated disc — recover well without surgery. Your specialist will discuss whether surgery is appropriate based on your specific situation.
Does provincial health insurance in Canada cover neck pain treatment?
According to Mayo Clinic’s overview of neck pain symptoms and causes, this information is supported by current medical research.
For more information, read our guide on ear and head discomfort during air travel.
Visits to your family doctor or a walk-in clinic for neck pain are covered under most provincial health plans across Canada. However, coverage for physiotherapy, chiropractic care, and massage therapy varies by province and whether you have extended health benefits. Check with your provincial health authority or extended benefits provider to understand what is covered for you.
Key Takeaways
- Neck pain is very common — up to 80% of Canadians will experience it in their lifetime.
- The three main types are overuse/strain pain, radicular pain from nerve compression, and joint-related pain.
- Most neck pain improves with rest, anti-inflammatory medication, physiotherapy, and exercise.
- Targeted neck exercises are proven to reduce pain and prevent future episodes.
- Progressive muscle weakness or numbness in the arm or hand needs prompt medical evaluation.
- See your family doctor or a walk-in clinic if your neck pain lasts more than two weeks or is getting worse.
- Always consult a qualified healthcare provider before starting a new treatment or exercise programme for neck pain.
Frequently Asked Questions
What are the most common neck pain causes?
The most common neck pain causes include muscle strain from poor posture, prolonged screen time, sleeping in an awkward position, whiplash injuries, and cervical disc problems. Arthritis and nerve compression are also frequent culprits. Most cases involve the soft tissues surrounding the cervical spine rather than serious structural damage.
What are the symptoms of neck pain I should watch for?
Neck pain symptoms include stiffness, limited range of motion, sharp or aching pain, headaches originating at the base of the skull, and shoulder or upper back discomfort. Numbness, tingling, or weakness radiating into the arms may indicate nerve involvement and warrants prompt medical evaluation.
How is neck pain treated in Canada?
Neck pain treatment in Canada typically includes physiotherapy, chiropractic care, massage therapy, and over-the-counter pain relievers like ibuprofen or acetaminophen. Heat or ice application, gentle stretching, and posture correction are also effective. Most provincial health plans partially cover physiotherapy; severe cases may require specialist referral or imaging.
How can I prevent neck pain causes from recurring?
Preventing recurring neck pain causes involves maintaining good posture during desk work, adjusting monitor height to eye level, taking regular movement breaks, using a supportive pillow, and strengthening neck and upper back muscles. Ergonomic workspace setups are especially important for Canadians working from home long-term.
When should I see a doctor for neck pain?
See a doctor immediately if neck pain follows trauma, is accompanied by numbness or weakness in the arms or hands, causes severe headache, fever, or difficulty swallowing. Pain lasting longer than two weeks without improvement also warrants medical assessment to rule out serious underlying conditions like disc herniation or infection.
About the Author
Dr. Sarah Mitchell, MDDr. Sarah Mitchell is a board-certified family physician with over 15 years of clinical experience. She completed her MD at the University of Toronto and her residency at Toronto General Hospital. Dr. Mitchell specializes in preventive medicine and chronic disease management. She is a member of the College of Family Physicians of Canada (CFPC) and has published over 30 peer-reviewed articles on preventive health care.
View all articles →