Gingivitis Causes, Treatment & Prevention in Canada
Share
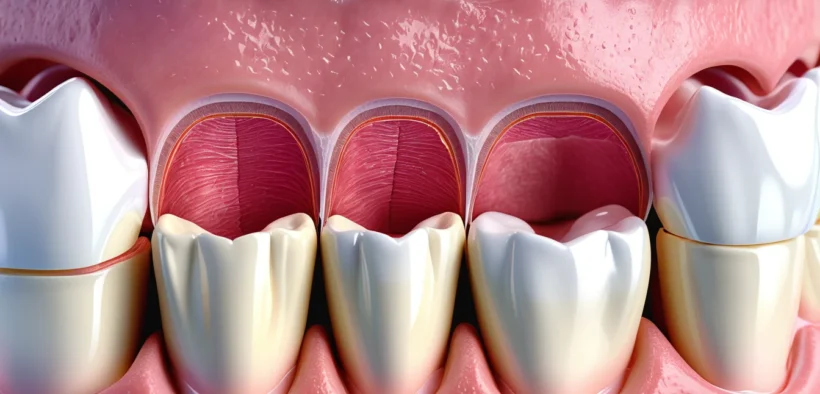
Gingivitis causes, treatment, and prevention are essential topics for every Canadian to understand — because this common form of gum disease affects millions of people across the country each year. Gingivitis develops when bacteria-laden plaque accumulates along the gumline, triggering inflammation that makes gums red, swollen, and prone to bleeding. The good news is that when caught early, gingivitis is entirely reversible.
Understanding Gingivitis Causes, Treatment & How to Reverse It
Recognizing early gum disease signs is the first step toward protecting your smile and your overall health. Many Canadians overlook bleeding gums or mild soreness, assuming the symptoms are normal. But left untreated, gingivitis can progress into periodontitis — a far more serious condition that can lead to tooth loss and has been linked to heart disease, diabetes complications, and other systemic health issues. With the right daily habits and professional dental care, you can stop gingivitis in its tracks and keep your gums healthy for life.
What Is Gingivitis?
| Treatment Option | How It Works | Benefits | Considerations |
|---|---|---|---|
| Professional Dental Cleaning (Scaling) | Dentist or dental hygienist removes plaque and tartar buildup from teeth and along the gumline | Directly eliminates the primary cause of gingivitis; provides immediate relief of inflammation | Recommended at least twice yearly; covered partially by most Canadian dental insurance plans and the Canadian Dental Care Plan (CDCP) |
| Improved Daily Brushing | Twice-daily brushing with a soft-bristled toothbrush disrupts plaque before it hardens into tartar | Low cost, highly effective for early-stage gingivitis; reduces bacteria at the gumline | Technique matters; brushing too hard can worsen gum irritation; electric toothbrushes may improve results |
| Daily Flossing | Removes interdental plaque and food debris that brushing cannot reach between teeth | Significantly reduces gingival bleeding and inflammation when done consistently | Floss picks or water flossers are acceptable alternatives for those with dexterity challenges |
| Antiseptic Mouthwash (e.g., Chlorhexidine) | Kills bacteria in the mouth and along the gumline to reduce plaque and infection | Clinically proven to reduce gingivitis symptoms; useful as an adjunct to mechanical cleaning | Chlorhexidine requires a prescription in Canada; long-term use may cause tooth staining and altered taste |
| Lifestyle Modifications | Quitting smoking, improving nutrition, and managing conditions like diabetes reduce systemic risk factors | Addresses underlying contributors to gingivitis; improves overall oral and systemic health | Smoking cessation support is available through provincial health programs across Canada |
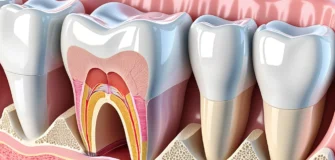
Gingivitis is an early form of gum disease. It causes changes to the colour, texture, and shape of the gum tissue around your teeth. Your gums may look redder than usual, feel puffy, or bleed when you brush.
These early signs are easy to miss because they are often painless. However, that does not mean the problem is harmless. Catching gingivitis early gives you the best chance of reversing it completely.
According to Health Canada, oral health is closely linked to your overall health. Problems in your mouth can affect the rest of your body, making it important to take gum inflammation seriously.
What Causes Gingivitis?
The main cause of gingivitis is bacterial plaque. Plaque is a soft, sticky film that builds up on your teeth every day. It forms when bacteria in your mouth mix with food particles and saliva.
When plaque sits along the gumline, the bacteria inside it release toxins. These toxins irritate the gums and trigger an inflammatory response. Your body is trying to fight back — but that inflammation is what causes the redness and swelling you see.
How Plaque Becomes Tartar
If plaque is not removed daily, it hardens over time. It absorbs calcium and phosphate from your saliva and turns into a rough, hardened substance called tartar (also called calculus). Tartar cannot be removed by brushing alone. You need a dental professional to clean it off.
This is why regular dental cleanings are so important. Once tartar forms, it creates a rough surface where even more plaque can stick — making the problem worse over time.
Risk Factors That Make Gingivitis More Likely
Some people are more likely to develop gingivitis than others. Understanding your risk can help you take action sooner.
- Poor oral hygiene — not brushing or flossing regularly
- Smoking or tobacco use — reduces blood flow to gum tissue
- Diabetes — affects the body’s ability to fight infection
- Dry mouth — less saliva means more bacterial buildup
- Certain medications — some drugs cause gum overgrowth or dry mouth
- Hormonal changes — pregnancy, puberty, and menopause can affect gum sensitivity
- Crowded teeth — harder to clean properly, allowing plaque to build up
If any of these apply to you, talk to your dentist. They can help you create a plan that fits your specific needs.
Recognising the Signs of Gingivitis
One of the tricky things about gingivitis is that it often does not hurt — at least not at first. Many Canadians do not realise they have it until a dentist points it out. Knowing what to look for helps you act quickly.
Common signs of gingivitis include:
- Gums that bleed when you brush or floss
- Red or dark reddish-purple gums (healthy gums should be pink and firm)
- Swollen or puffy gums
- Gums that feel tender when touched
- Persistent bad breath that does not go away
- Gums that appear to be pulling away from your teeth
Bleeding gums are never normal. If you notice blood when you brush, do not ignore it. It is one of the earliest and most reliable signs that your gums need attention.
How to Treat Gingivitis
The main goal of gingivitis treatment is to remove plaque and tartar from around the gumline. In many cases, this can be done at your regular dental cleaning appointment. Your dentist or dental hygienist will use special tools to scale away tartar above and below the gumline.
After a professional cleaning, the real work happens at home. Your gums need consistent daily care to heal and stay healthy. In most early-stage cases, gingivitis can be fully reversed with good oral hygiene habits.
Professional Dental Treatments
For more advanced cases, your dentist may recommend a deeper cleaning procedure called scaling and root planing. This smooths the root surfaces of your teeth so bacteria have less surface to cling to. Your dentist will advise you on what level of treatment is right for you.
The Mayo Clinic’s overview of gingivitis treatment confirms that professional cleaning is the most effective first step. From there, maintaining a strong home routine is essential to prevent it from coming back.
Crowns, Bridges, and Dental Work
Sometimes dental work itself can make gingivitis harder to manage. Ill-fitting crowns, bridges that cannot be cleaned underneath, or overcrowded teeth can all trap plaque. Your dentist can assess whether any existing dental work needs to be adjusted to support better gum health.
How to Prevent Gingivitis at Home
Prevention is always easier than treatment. The best defence against gingivitis is a consistent daily oral hygiene routine. Most dentists agree that brushing and flossing properly every single day can make a dramatic difference.
Brushing
Brush your teeth at least twice a day — once in the morning and once before bed. Use a soft-bristled toothbrush and fluoride toothpaste. Hold your brush at a 45-degree angle to your gums and use gentle circular motions. Brush for at least two full minutes.
Replace your toothbrush every three to four months, or sooner if the bristles look frayed. A worn toothbrush does not clean effectively.
Flossing
Flossing removes plaque and food from between your teeth — places your toothbrush simply cannot reach. Floss at least once a day, ideally before bedtime. If regular floss is difficult to use, try floss picks, a water flosser, or an interdental brush.
Mouthwash
An antibacterial mouthwash can help reduce bacteria in your mouth and freshen your breath. Look for a mouthwash that is approved by the Canadian Dental Association (CDA). Mouthwash works best as a complement to brushing and flossing — not a replacement for them.
Diet and Lifestyle
What you eat affects your gum health. Sugary and starchy foods feed the bacteria that cause plaque. Eating a balanced diet rich in vegetables, whole grains, and fibre helps support a healthy mouth. Drinking plenty of water — especially fluoridated tap water — also protects your teeth.
If you smoke, quitting is one of the best things you can do for your gum health. Smoking weakens your immune system’s ability to fight gum infections. Furthermore, smokers often have more severe gum disease and heal more slowly after treatment.
What Happens If Gingivitis Is Left Untreated?
Untreated gingivitis does not stay mild forever. Over time, it can progress into a more serious condition called periodontitis. This is a deep infection of the gums and the bone that supports your teeth.
As a result of periodontitis, the bone and connective tissue that hold your teeth in place can be permanently destroyed. This leads to loose teeth and, eventually, tooth loss. Unlike gingivitis, the damage caused by periodontitis cannot always be fully reversed.
Research published by the World Health Organization on oral health shows that severe gum disease affects nearly 19% of adults worldwide. It is also linked to other health conditions, including heart disease and diabetes. Taking care of your gums is about more than just your smile.
When to See a Doctor or Dentist
If your gums bleed regularly, look red or swollen, or you have persistent bad breath, it is time to see a dental professional. Do not wait for pain — gingivitis is often painless until it becomes more serious.
Most provincial health plans in Canada provide some coverage for dental cleanings and checkups, particularly for children. Adults should check their provincial benefits or private insurance plan to understand what is covered. If you do not have a family dentist, a walk-in dental clinic can be a good starting point for an assessment.
Your family doctor can also be a helpful resource. They can refer you to a dentist, discuss any medications that might be affecting your gum health, and help you manage underlying conditions like diabetes that increase your risk.
Always consult your dentist or family doctor before starting any new oral health treatment, especially if you have underlying health conditions or are taking medication.
Frequently Asked Questions About Gingivitis
Can gingivitis go away on its own?
Gingivitis does not typically go away without treatment. However, it can be fully reversed with consistent brushing, flossing, and a professional dental cleaning. The sooner you address it, the easier it is to treat.
How long does it take to treat gingivitis?
Most people see improvement in their gum health within two to four weeks of starting a consistent oral hygiene routine. After a professional cleaning, gingivitis symptoms like bleeding and swelling usually begin to reduce within one to two weeks. Your dentist can track your progress at follow-up visits.
Is gingivitis contagious?
The bacteria that contribute to gingivitis can be spread through saliva, for example through kissing or sharing utensils. However, developing gingivitis also depends on individual oral hygiene habits and personal risk factors. Maintaining good oral hygiene is the best way to protect yourself.
What is the difference between gingivitis and periodontitis?
Gingivitis is the early, milder stage of gum disease that affects only the gum tissue. Periodontitis is a more advanced stage where the infection spreads to the bone and tissue supporting your teeth. Unlike gingivitis, periodontitis can cause permanent damage and tooth loss if left untreated.
Can children get gingivitis?
Yes, children can develop gingivitis, especially during puberty when hormonal changes affect gum sensitivity. Teaching children good brushing and flossing habits early is one of the most effective ways to prevent gum disease for life. Many provincial health programmes in Canada offer dental coverage for children to support regular checkups.
Does mouthwash cure gingivitis?
According to Health Canada’s guidelines on oral health, this information is supported by current medical research.
For more information, read our guide on endocrine disorders that may increase your risk of gum disease.
Mouthwash alone cannot cure gingivitis. It can help reduce bacteria and control bad breath, but it does not replace brushing, flossing, or professional dental cleanings. Use an antibacterial mouthwash as part of a complete oral hygiene routine for the best results.
Key Takeaways
- Gingivitis is an early, reversible form of gum disease caused by bacterial plaque.
- Common signs include bleeding gums, redness, swelling, and bad breath.
- The condition is fully preventable and treatable with good daily oral hygiene.
- Brush twice a day, floss daily, and visit your dentist for regular cleanings.
- If left untreated, gingivitis can progress to periodontitis and lead to tooth loss.
- Risk factors include smoking, diabetes, dry mouth, hormonal changes, and crowded teeth.
- If you notice bleeding or swollen gums, see your dentist or visit a walk-in dental clinic — do not wait for pain.
- Always speak with your dentist or family doctor for personalised advice about your oral health.
Frequently Asked Questions
What are the main gingivitis causes and treatment options in Canada?
Gingivitis is primarily caused by plaque buildup along the gumline, leading to bacterial infection and inflammation. Other causes include smoking, hormonal changes, diabetes, and certain medications. Treatment involves professional dental cleaning, improved brushing and flossing habits, and antimicrobial mouthwash. Most cases resolve fully with consistent oral hygiene.
What are the early symptoms of gingivitis?
Early gingivitis symptoms include red, swollen, or puffy gums that bleed easily when brushing or flossing. Gums may appear darker than their normal pink colour. Bad breath and gum tenderness are also common warning signs. Unlike advanced gum disease, gingivitis is painless, making it easy to overlook without regular dental checkups.
What is the most effective gingivitis causes treatment recommended by dentists?
The most effective gingivitis treatment begins with a professional dental cleaning called scaling, which removes hardened plaque and tartar. Dentists also recommend brushing twice daily with fluoride toothpaste, flossing daily, and using an antibacterial mouthwash. Following this routine consistently can reverse gingivitis within two to four weeks.
How can I prevent gingivitis at home?
Preventing gingivitis at home involves brushing teeth twice daily for two minutes, flossing once daily, and rinsing with an antibacterial mouthwash. Avoiding tobacco, eating a balanced diet low in sugar, and staying hydrated also reduce risk. Regular professional cleanings every six months are essential for long-term gum health.
When should I see a dentist for gingivitis in Canada?
See a dentist if your gums bleed regularly when brushing, appear persistently red or swollen, or if you notice persistent bad breath. Early intervention prevents gingivitis from progressing to periodontitis, a serious condition causing tooth and bone loss. Most provincial dental associations recommend checkups every six months for preventive care.
About the Author
Dr. Linda Chen, RD, PhDDr. Linda Chen is a registered dietitian and PhD in Nutritional Sciences from the University of British Columbia. With expertise in clinical nutrition, sports dietetics, and gut health, she has worked with leading Canadian hospitals and sports organizations. Dr. Chen is a member of Dietitians of Canada and regularly contributes to national nutrition policy discussions.
View all articles →