Gum Disease: Causes, Symptoms & Treatment in Canada
Share
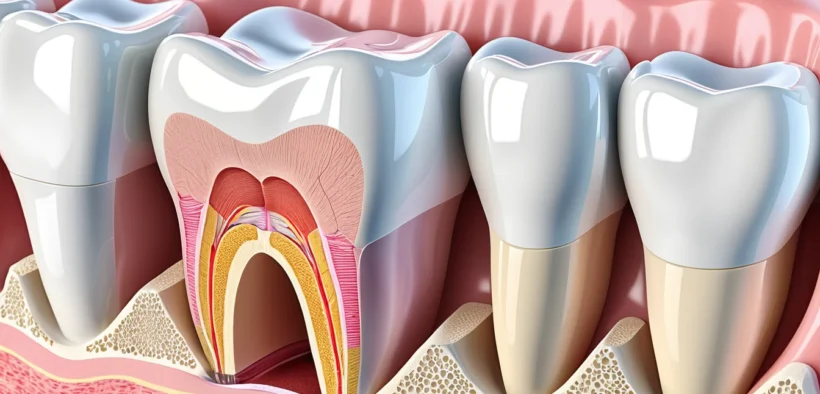
Gum disease is one of the most common oral health problems in Canada — yet it remains one of the most overlooked conditions affecting millions of Canadians every year. It starts quietly as mild inflammation along the gumline, but without timely intervention, it can silently destroy the soft tissue and bone that hold your teeth in place, eventually leading to tooth loss.
How Gum Disease Develops and Why Early Action Matters
The early stage, known as gingivitis, produces subtle gingivitis symptoms such as red, swollen, or bleeding gums that many people dismiss as normal. However, when left untreated, gingivitis progresses into periodontitis — a far more serious and potentially irreversible condition. According to Health Canada, oral disease remains a significant public health concern for Canadians of all ages, making awareness and early detection more important than ever.
What Is Gum Disease?
| Stage | Characteristics | Common Symptoms | Recommended Management |
|---|---|---|---|
| Gingivitis (Early Gum Disease) | Inflammation limited to the gum tissue; no bone or connective tissue damage; fully reversible | Red, swollen gums; bleeding when brushing or flossing; mild bad breath | Professional dental cleaning; improved daily brushing and flossing; antibacterial mouthrinse |
| Mild Periodontitis | Infection begins to affect bone and connective tissue; pocket depths of 3–4 mm form around teeth | Increased gum bleeding; slight gum recession; persistent bad breath; early tooth sensitivity | Scaling and root planing (deep cleaning); more frequent dental visits (every 3–4 months); improved oral hygiene routine |
| Moderate Periodontitis | Progressive bone and tissue loss; pocket depths of 4–6 mm; bacteria may enter the bloodstream | Noticeable gum recession; increased tooth sensitivity; loose or shifting teeth; pus between teeth and gums | Scaling and root planing; possible antibiotic therapy; referral to a periodontist; lifestyle modifications |
| Severe Periodontitis | Significant bone loss; pocket depths greater than 6 mm; high risk of tooth loss; systemic health implications | Severe gum recession; very loose teeth; difficulty chewing; intense pain; significant bone destruction visible on X-ray | Periodontal surgery (osseous surgery or flap surgery); bone grafting; possible tooth extraction; ongoing specialist care |
Gum disease, also called periodontitis or periodontal disease, is an infection that damages the soft tissue and bone supporting your teeth. It begins when bacteria build up along and under the gumline. Over time, this leads to serious and irreversible damage.
The early stage of gum disease is called gingivitis. At this stage, only the gums are affected, and the damage can still be reversed with proper care. However, when gingivitis is left untreated, it progresses into periodontitis — a much more serious condition. According to Health Canada, oral disease remains a significant public health concern for Canadians of all ages.
The science of diagnosing and treating gum disease is called periodontology. A dentist diagnoses the condition through a clinical examination of the gum tissue, along with dental X-rays. The sooner it is caught, the better the outcome.
Signs and Symptoms of Gum Disease
One of the biggest challenges with gum disease is that it often causes no pain in the early stages. Many people do not realise they have it until significant damage has already occurred. Knowing the warning signs can help you act quickly.
Common Signs to Watch For
- Red, swollen, or purple gums — healthy gums should be firm and pink
- Bleeding when you brush or floss — this is one of the earliest warning signs
- Bad breath (halitosis) — especially in the morning, but also throughout the day
- Receding gums — your teeth may look longer than before
- Tartar and plaque buildup — visible deposits on teeth near the gumline
- Loose or shifting teeth — a sign that bone support is being lost
- Deep pockets between teeth and gums — bacteria thrive in these spaces
It is worth noting that smokers may not experience gum bleeding as often. Smoking reduces blood flow to the gums, which can mask this common symptom. However, smoking is actually a major risk factor for severe gum disease.
When the gums pull away from the teeth, they leave deep pockets where bacteria multiply. These bacteria then attack the bone and connective tissue that anchor your teeth. As a result, teeth can become loose and may eventually fall out.
What Causes Gum Disease?
The main cause of gum disease is the buildup of plaque — a sticky film of bacteria that forms on teeth every day. When plaque is not removed through brushing and flossing, it hardens into tartar. Tartar can only be removed by a dental professional.
Risk Factors That Make It Worse
Several factors increase your risk of developing gum disease. Being aware of these can help you take better care of your oral health.
- Smoking or tobacco use — one of the strongest risk factors for severe gum disease
- Poor oral hygiene — infrequent brushing and skipping floss
- Genetics — some people are more prone to gum disease due to their family history
- Diabetes — high blood sugar levels can worsen gum infections
- Certain medications — some drugs reduce saliva flow, which protects the gums
- Stress — weakens the immune system’s ability to fight infection
- Hormonal changes — pregnancy and menopause can make gums more sensitive
Genetics does play a role in how your body responds to bacteria. However, good oral hygiene can significantly reduce your risk, even if gum disease runs in your family. Your behaviour matters more than your genes in most cases.
For more information on how lifestyle factors affect oral health, visit the Mayo Clinic’s periodontitis overview.
How Gum Disease Progresses
Gum disease does not happen overnight. It moves through stages, and each stage causes more damage than the last. Understanding this progression helps explain why early treatment is so important.
Stage 1: Gingivitis
Gingivitis is the earliest and mildest form of gum disease. The gums become red and swollen, and may bleed when you brush. At this stage, the bone and connective tissue are not yet affected. With proper brushing, flossing, and a professional cleaning, gingivitis can be fully reversed.
Stage 2: Early Periodontitis
If gingivitis is not treated, it advances to periodontitis. The gums begin to pull away from the teeth, forming pockets. Bacteria grow deep inside these pockets. The bone supporting the teeth starts to break down, and this damage is permanent.
Stage 3: Advanced Periodontitis
In advanced periodontitis, the bone and tissue loss becomes severe. Teeth may shift, loosen, or fall out entirely. At this stage, even aggressive treatment may not be able to save all the teeth. Furthermore, replacing lost teeth with implants or dentures becomes more complicated when the supporting bone has been destroyed.
Treatment Options for Gum Disease
The good news is that gum disease can be managed effectively, especially when caught early. Treatment cannot fully reverse the damage, but it can stop the disease from progressing. Your dentist will recommend a treatment plan based on how advanced your gum disease is.
Non-Surgical Treatment: Scaling and Root Planing
The most common non-surgical treatment is a deep cleaning called scaling and root planing. This procedure removes tartar and bacteria from below the gumline. The dentist uses ultrasonic instruments and fine hand tools to clean the root surfaces. This helps the gums reattach to the teeth and reduces pocket depth.
This type of treatment is sometimes called a “closed field” subgingival cleaning because the gums are not cut or moved aside. Most patients can manage with a local anaesthetic, and recovery is straightforward.
Surgical Treatment
In more advanced cases, surgery may be needed. A procedure called flap surgery involves gently folding back the gum tissue so the dentist can access and clean deeper areas of bone damage. In some cases, bone grafting or regenerative materials are used to help rebuild lost bone.
Surgical options are considered when non-surgical cleaning alone cannot control the infection. Your dentist or periodontist will explain all your options clearly before proceeding.
The Role of Home Care
No treatment works without your effort at home. Brushing twice daily, flossing every day, and using an antibacterial mouthwash all play a key role. Your dentist will show you the correct brushing technique and help you build a routine that works for you.
Quitting smoking is also critical. Smoking slows healing and increases the risk of gum disease returning. It is one of the most important steps you can take to protect your oral health. The Healthline guide to periodontitis offers further tips on managing gum disease at home.
Ongoing Maintenance Visits
After treatment, regular professional cleanings are essential. Depending on your situation, your dentist may recommend cleanings every one to six months. These appointments monitor the health of your gums and catch any signs of the disease returning early. Skipping these visits puts all your progress at risk.
Gum Disease and Your Overall Health
Gum disease does not just affect your mouth. Research has linked periodontitis to several serious health conditions. These include heart disease, diabetes complications, and respiratory infections. The bacteria from infected gums can enter the bloodstream and affect other parts of the body.
For Canadians managing chronic conditions like diabetes or heart disease, keeping gum disease under control is especially important. Speak with both your dentist and your family doctor about how your oral health connects to your overall wellbeing. Your provincial health plan may cover some dental assessments, especially if you have a qualifying condition — check with your provider for details.
When to See a Doctor or Dentist
You should book an appointment with your dentist if you notice any of the warning signs listed above. Do not wait for pain — gum disease is often painless until it is quite advanced. Early action makes a real difference.
If you do not have a regular dentist, your family doctor can refer you to one, or you can visit a walk-in dental clinic. Many communities across Canada have low-cost dental options through community health centres. Some provincial programmes also offer dental coverage for children, seniors, and low-income Canadians — ask at your local public health office.
If your gums are bleeding heavily, you have sudden tooth pain, or a tooth feels very loose, seek care promptly. A walk-in medical clinic can also assess signs of infection if you cannot reach a dentist right away.
Always speak with a qualified dental or medical professional for advice specific to your health situation. This article is for general information only.
Frequently Asked Questions About Gum Disease
Can gum disease be cured completely?
Gum disease cannot be fully cured once it has progressed beyond gingivitis, but it can be effectively controlled. With professional treatment and consistent home care, the progression of gum disease can be stopped. The key is early detection and ongoing maintenance with your dentist.
What does gum disease look like?
Gum disease often appears as red, swollen, or dark-coloured gums that bleed easily when brushing or flossing. You may also notice your gums pulling away from your teeth, making them look longer. In more advanced stages, teeth can become loose or gaps may appear between them.
Is gum disease linked to bad breath?
Yes, persistent bad breath (halitosis) is one of the most common signs of gum disease. The bacteria that cause gum disease release foul-smelling gases as they break down tissue and food particles. If brushing and mouthwash do not resolve bad breath, it is worth visiting a dentist to rule out gum disease.
How is gum disease treated in Canada?
In Canada, gum disease is treated by a dentist or periodontist, depending on severity. Mild to moderate cases are typically managed with a deep cleaning procedure called scaling and root planing. More advanced gum disease may require surgical treatment, and ongoing maintenance cleanings are essential after any treatment.
Can gum disease cause tooth loss?
Yes, untreated gum disease is one of the leading causes of tooth loss in adults. As the infection destroys the bone and connective tissue supporting the teeth, they become loose and may eventually fall out. Starting treatment early is the best way to prevent permanent tooth loss from gum disease.
Does gum disease run in families?
According to Health Canada’s oral health guidelines, this information is supported by current medical research.
For more information, read our guide on endocrine disorders that may worsen periodontal disease.
Genetics can influence how your body responds to the bacteria that cause gum disease, so it can run in families. However, good oral hygiene habits significantly reduce your risk, even if you have a family history. Regular dental visits and diligent home care are the most effective way to manage your genetic risk.
Key Takeaways
- Gum disease progresses from mild gingivitis to serious periodontitis if left untreated.
- Common signs include red or bleeding gums, bad breath, receding gums, and loose teeth.
- Smoking, poor oral hygiene, diabetes, and genetics all increase your risk.
- Treatment can stop gum disease from progressing, but it cannot reverse bone loss that has already occurred.
- Both professional treatment and daily home care are essential for long-term success.
- Regular dental cleanings — every one to six months — are critical after treatment.
- Gum disease is linked to other health conditions, including heart disease and diabetes.
- Canadians without a dentist can access care through walk-in dental clinics or community health centres.
- Always consult your dentist or family doctor for advice tailored to your personal health needs.
Frequently Asked Questions
What is gum disease?
Gum disease (periodontal disease) is a bacterial infection of the tissues surrounding and supporting your teeth. It begins as gingivitis — inflammation caused by plaque buildup — and can progress to periodontitis, where infection damages the gums, bone, and connective tissue, potentially leading to tooth loss if left untreated.
What are the early warning signs of gum disease?
Early signs of gum disease include red, swollen, or tender gums, bleeding when brushing or flossing, persistent bad breath, and gums that appear to be pulling away from teeth. Many Canadians ignore these symptoms since early-stage gum disease is often painless, making regular dental checkups essential for early detection.
How is gum disease treated in Canada?
Gum disease treatment depends on severity. Early stages are treated with professional dental cleaning and improved oral hygiene. Advanced cases require scaling and root planing (deep cleaning), antibiotics, or periodontal surgery. Most Canadian dental insurance plans provide partial coverage for these procedures — check your plan for specific benefits.
Can gum disease be reversed or prevented?
Early-stage gum disease (gingivitis) can be fully reversed with professional cleaning and consistent oral hygiene. Advanced periodontitis cannot be reversed but can be managed. Prevention includes brushing twice daily, flossing once daily, avoiding smoking, eating a balanced diet, and visiting your dentist for cleanings every six months.
When should you see a dentist for gum problems?
See a dentist promptly if you notice bleeding gums, persistent bad breath, gum recession, loose teeth, or pain while chewing. These symptoms suggest infection that worsens without professional treatment. Canadians without a regular dentist can contact their provincial dental association for referrals or visit a community dental clinic.
About the Author
Dr. Michael Ross, MD, FRCSCDr. Michael Ross is a fellowship-trained orthopedic surgeon at the University of Alberta Hospital, specializing in joint replacement and sports medicine. A Fellow of the Royal College of Surgeons of Canada (FRCSC), he has over 18 years of surgical experience and has authored multiple textbook chapters on musculoskeletal health. Dr. Ross is passionate about patient education and evidence-based medicine.
View all articles →