Hoffa’s Fat Pad Syndrome: Causes, Symptoms & Treatment
Share
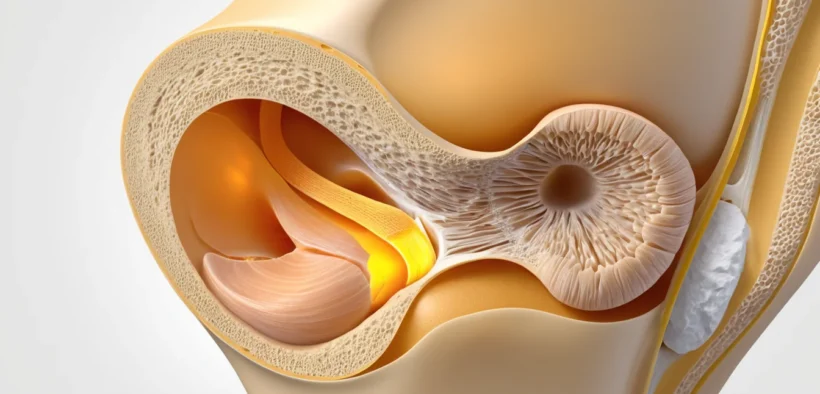
Hoffa’s fat pad syndrome is a common yet often overlooked cause of anterior knee pain that affects thousands of Canadians every year. This condition occurs when the infrapatellar fat pad, a small cushion of fatty tissue located just below the kneecap, becomes pinched, irritated, or inflamed during everyday movement or physical activity.
What Causes Hoffa’s Fat Pad Syndrome and Who Is at Risk?
Also known as infrapatellar fat pad impingement, this syndrome can cause sharp pain at the front of the knee that worsens with standing, walking, or straightening the leg. Many Canadians mistake it for other knee injuries, which can delay proper diagnosis and treatment. Understanding the causes, symptoms, and treatment options can help you take the right steps toward recovery and get back to the activities you enjoy.
What Is Hoffa’s Fat Pad Syndrome?
| Treatment Option | Benefits | Considerations |
|---|---|---|
| Rest & Activity Modification | Reduces inflammation and repeated impingement; no cost; first-line approach | Requires patient compliance; temporary activity restrictions may affect daily life |
| Physiotherapy | Strengthens quadriceps and surrounding muscles; improves patellar tracking; widely available across Canada | Requires multiple sessions over several weeks; effectiveness depends on severity of condition |
| Corticosteroid Injections | Provides significant short-term pain relief; reduces local inflammation quickly | Limited to 2–3 injections per year; may cause fat pad atrophy with repeated use; administered by physician |
| Taping & Bracing | Offloads the infrapatellar fat pad; provides immediate symptom relief; low-cost adjunct therapy | Requires proper technique; skin irritation possible; not a standalone long-term solution |
| Platelet-Rich Plasma (PRP) Therapy | Promotes tissue healing; growing evidence for chronic cases; minimally invasive | Limited OHIP/provincial coverage; variable availability across Canadian provinces; higher out-of-pocket cost |
| Surgical Resection (Hoffa’s Procedure) | Effective for refractory cases; removes impinging fat pad tissue; long-term resolution | Reserved for cases unresponsive to conservative care; carries standard surgical risks; recovery time of several weeks |
The Hoffa fat pad sits between the lower edge of the kneecap (patella) and the shin bone (tibia). It acts as a natural shock absorber, protecting the kneecap tendon and surrounding bone surfaces. Think of it as a small protective pillow inside your knee.
When this fat pad becomes pinched or inflamed, the condition is called Hoffa’s fat pad syndrome, sometimes also called fat pad impingement. It is considered one of the most sensitive structures in the entire knee joint. Even minor irritation can cause noticeable discomfort.
According to Mayo Clinic’s orthopaedic health resources, knee pain from soft tissue inflammation is a common reason people seek medical care, and accurate diagnosis is essential for effective treatment.
Common Causes of Hoffa’s Fat Pad Syndrome
This condition can develop in several ways. Sometimes it starts suddenly after a direct blow to the knee. Other times, it builds up gradually over weeks or months.
Common causes include:
- A direct impact or blow to the kneecap area
- Chronic osteoarthritis of the knee
- Tight quadriceps muscles at the front of the thigh
- Hyperextension of the knee — when the joint bends too far backward
- Repeated knee movements that stretch the joint beyond its normal range
Hoffa’s fat pad syndrome develops gradually when the knee is extended repeatedly past its normal straight position. Athletes who play sports with frequent jumping, landing, or pivoting are at higher risk. However, this condition can also affect people who stand for long periods at work.
Who Is Most at Risk?
Anyone can develop Hoffa’s fat pad syndrome, but certain people are more likely to experience it. Those with a kneecap that tilts backward and downward are more prone to pinching the fat pad. People who tend to hyperextend their knees during daily activities or sport are also at increased risk.
Young athletes, construction workers, retail employees, and healthcare workers who spend long hours on their feet may be especially vulnerable. If you have existing knee arthritis, you may also be more susceptible to this condition.
Signs and Symptoms of Hoffa’s Fat Pad Syndrome
The most common symptom is pain at the front and lower part of the knee, on either side of the kneecap tendon. This pain often worsens when you fully straighten your knee. It can feel sharp and immediate, especially during activity.
Other symptoms to watch for include:
- Swelling or puffiness around the kneecap tendon
- Pain that gets worse after standing for long periods
- Increased discomfort when jumping or landing
- Pain triggered by any position that causes the knee to hyperextend
Importantly, Hoffa’s fat pad syndrome does not typically cause the knee to lock, crack, or feel unstable. These symptoms point to a different knee problem. If you experience locking or giving way of the knee, speak with your family doctor promptly.
How Is It Different from Patellar Tendinitis?
Hoffa’s fat pad syndrome is sometimes confused with patellar tendinitis, also called jumper’s knee. However, there is a clear difference. With patellar tendinitis, pain is focused specifically on the tendon itself, usually at the lower tip of the kneecap.
With Hoffa’s fat pad syndrome, pain is felt on both sides of the kneecap tendon, in the area where the fat pad sits. This distinction matters greatly for choosing the right treatment. A healthcare professional can help you tell the difference with a physical assessment.
How Hoffa’s Fat Pad Syndrome Is Diagnosed
Diagnosis usually starts with a thorough physical examination of the knee. A physiotherapist or doctor will ask about your symptoms and how your knee feels during specific movements. They will also perform special hands-on tests designed to reproduce your pain and identify the fat pad as the source.
In many cases, a clinical examination alone is enough to confirm the diagnosis. However, imaging tests can provide additional information when needed.
Imaging and Further Tests
Your healthcare provider may recommend an MRI (magnetic resonance imaging) to get a detailed look at the soft tissues inside your knee. An ultrasound scan can also show swelling or changes in the fat pad tissue. These tools help rule out other conditions that may look similar.
Because the symptoms of Hoffa’s fat pad syndrome can overlap with other knee problems, it is important to get a precise diagnosis. This ensures you receive the most appropriate and effective treatment from the start. You can learn more about knee imaging options through Health Canada’s diagnostic imaging information.
Treatment Options for Hoffa’s Fat Pad Syndrome
The good news is that most people with Hoffa’s fat pad syndrome respond well to conservative, non-surgical treatment. The goal is to reduce inflammation, relieve pain, and prevent the problem from coming back.
Conservative (Non-Surgical) Treatment
Your doctor or physiotherapist will likely recommend starting with these approaches:
- Rest: Avoid activities that make your pain worse, such as running or jumping, until inflammation settles down.
- Ice therapy: Applying ice to the affected area helps reduce swelling and pain. Use a cloth-wrapped ice pack for 15–20 minutes at a time.
- Anti-inflammatory medication: Over-the-counter medications like ibuprofen can help manage pain and reduce swelling. Always follow the dosage instructions on the label.
- Corticosteroid injections: In some cases, a doctor may inject a corticosteroid directly into the knee to reduce severe inflammation.
- Physiotherapy: A registered physiotherapist can guide you through exercises to strengthen the muscles around your knee. Techniques like therapeutic ultrasound and transcutaneous electrical nerve stimulation (TENS) may also be used to manage pain.
- Patellar taping: Applying a special supportive tape above the kneecap can lift it slightly, creating more space for the fat pad and reducing pressure on the tissue.
Strengthening the quadriceps and surrounding muscle groups is an important part of long-term recovery. These muscles support and protect the knee joint, reducing stress on the fat pad during everyday movement.
Surgical Treatment
If conservative treatment does not produce the expected results after several months, surgery may be considered. The surgical procedure for Hoffa’s fat pad syndrome uses arthroscopic (keyhole) surgery.
During the procedure, a surgeon makes two small incisions below the kneecap. A tiny camera is inserted through one opening to view the inside of the joint. Surgical instruments are inserted through the other opening to remove part or all of the inflamed fat pad tissue.
Research shows that patients without other concurrent knee conditions tend to experience significant long-term improvement after arthroscopic resection. Recovery and noticeable improvement in symptoms can take anywhere from 3 to 12 months following surgery.
Possible Surgical Risks and Complications
As with any surgical procedure, there are some risks to be aware of. These include infection, bleeding, nerve injury (which may cause numbness or weakness), and continued pain or fat pad impingement after surgery. In rare cases, there is a risk of damage to the kneecap tendon.
Your surgeon will explain all risks clearly before any procedure. It is important to ask questions and make an informed decision together with your healthcare team.
Possible Complications If Left Untreated
Ignoring Hoffa’s fat pad syndrome can lead to ongoing problems. Chronic inflammation may develop if the fat pad is repeatedly irritated without proper treatment. Over time, this can become a persistent condition that is harder to manage.
For athletes, the condition can become serious enough to affect performance and competitive ability. Returning to activity too soon — before full recovery — can also delay healing and make symptoms worse. It is always better to address knee pain early rather than push through it.
The Healthline guide to knee pain causes and management provides useful general information on when and why knee conditions should be taken seriously.
Prevention of Hoffa’s Fat Pad Syndrome
Preventing this condition starts with being mindful of activities that stress the knee joint. Avoiding prolonged kneeling, deep squatting, or movements that cause the knee to hyperextend can lower your risk significantly. Wearing supportive footwear also helps maintain proper knee alignment.
Regular strengthening exercises for the quadriceps, hamstrings, and hip muscles protect the knee during everyday movement and sport. If you notice any early knee discomfort, rest and address it promptly rather than waiting for it to worsen.
When to See a Doctor
If you have persistent pain at the front of your knee that lasts more than a week or two, it is a good idea to seek medical advice. Start by booking an appointment with your family doctor, who can assess your knee and refer you to a physiotherapist or orthopaedic specialist if needed.
If you do not have a family doctor, a walk-in clinic is a good first option. Most provincial health plans in Canada cover initial assessments for musculoskeletal conditions like knee pain. Do not wait until the pain becomes unbearable — early treatment leads to better outcomes.
Seek care right away if your knee is severely swollen, if you cannot bear weight on your leg, or if the pain came on suddenly after an injury.
Frequently Asked Questions About Hoffa’s Fat Pad Syndrome
What does Hoffa’s fat pad syndrome feel like?
Hoffa’s fat pad syndrome typically causes pain at the front and lower part of the knee, on either side of the kneecap tendon. The pain often feels worse when you fully straighten your leg or stand for long periods. Some people also notice mild swelling around the kneecap area.
How long does Hoffa’s fat pad syndrome take to heal?
Recovery time for Hoffa’s fat pad syndrome depends on the severity and the type of treatment used. With conservative treatment, many people see improvement within 6 to 12 weeks. If surgery is required, improvements can take anywhere from 3 to 12 months.
Can Hoffa’s fat pad syndrome heal on its own?
Mild cases of Hoffa’s fat pad syndrome may improve with rest and activity modification. However, without proper treatment, the fat pad can remain chronically inflamed and the condition may become long-term. It is best to consult a healthcare professional for an accurate assessment and treatment plan.
Is Hoffa’s fat pad syndrome the same as jumper’s knee?
No, these are two different conditions. Jumper’s knee (patellar tendinitis) causes pain focused on the kneecap tendon itself. Hoffa’s fat pad syndrome causes pain on both sides of that tendon, where the fat pad tissue is located. A physiotherapist or doctor can distinguish between the two with a physical examination.
Do I need surgery for Hoffa’s fat pad syndrome?
Most people with Hoffa’s fat pad syndrome do not need surgery. Conservative treatments like physiotherapy, rest, ice, and patellar taping are effective for the majority of patients. Surgery is only considered when conservative treatment has not worked after several months of consistent effort.
Can I exercise with Hoffa’s fat pad syndrome?
According to Mayo Clinic’s overview of knee pain causes and treatment, this information is supported by current medical research.
For more information, read our guide on MRI vs CT scan differences for diagnosing knee conditions.
Some forms of exercise are safe and even helpful for Hoffa’s fat pad syndrome, particularly gentle strengthening exercises recommended by a physiotherapist. However, high-impact activities like running and jumping should be avoided during the acute phase. Always get guidance from a healthcare professional before continuing or starting an exercise routine.
Key Takeaways
- Hoffa’s fat pad syndrome involves inflammation of the fatty tissue located just below the kneecap.
- Common causes include direct knee impact, chronic arthritis, tight thigh muscles, and knee hyperextension.
- The main symptom is pain at the front and lower knee, on either side of the kneecap tendon, that worsens with straightening the leg.
- It is different from patellar tendinitis, though the two conditions can look similar.
- Most cases respond well to conservative treatment, including rest, physiotherapy, ice, and patellar taping.
- Surgery (arthroscopic resection) is available for cases that do not improve with non-surgical care.
- Early treatment leads to better outcomes — if knee pain persists, see your family doctor or visit a walk-in clinic.
- This article is for general informational purposes only. Always consult a qualified healthcare professional for diagnosis and treatment tailored to your individual needs.
Frequently Asked Questions
What is Hoffa’s fat pad syndrome?
Hoffa’s fat pad syndrome is a knee condition involving inflammation and impingement of the infrapatellar fat pad, a soft tissue structure located below the kneecap. It causes chronic anterior knee pain, typically worsened by prolonged standing or knee extension. It commonly affects athletes, active adults, and people who have experienced direct knee trauma.
What are the symptoms of Hoffa’s fat pad syndrome?
Common symptoms include sharp or aching pain below the kneecap, swelling around the lower knee, tenderness when pressing the area beside the patellar tendon, and pain that worsens with knee straightening, prolonged activity, or climbing stairs. Some people also notice a soft tissue bulge on either side of the patellar tendon.
How is Hoffa’s fat pad syndrome treated in Canada?
Treatment typically begins conservatively with physiotherapy, activity modification, taping techniques, and anti-inflammatory medications. Corticosteroid injections may be recommended for persistent cases. If conservative care fails after several months, arthroscopic surgery to partially remove or decompress the fat pad is available through orthopaedic specialists across Canada.
Can Hoffa’s fat pad syndrome be prevented?
Prevention focuses on maintaining strong quadriceps and hip muscles to reduce knee stress, avoiding prolonged kneeling or hyperextension, and wearing appropriate footwear. Gradual progression of exercise intensity, proper warm-up routines, and addressing biomechanical issues like flat feet or poor posture can significantly lower the risk of developing this condition.
When should you see a doctor for knee fat pad pain?
See a doctor or physiotherapist if knee pain below the kneecap persists beyond two weeks, worsens with daily activities, or is accompanied by significant swelling and reduced mobility. Early assessment helps rule out other conditions like patellar tendinopathy or meniscus injuries and ensures timely, appropriate treatment to prevent chronic impingement.
About the Author
Dr. Michael Ross, MD, FRCSCDr. Michael Ross is a fellowship-trained orthopedic surgeon at the University of Alberta Hospital, specializing in joint replacement and sports medicine. A Fellow of the Royal College of Surgeons of Canada (FRCSC), he has over 18 years of surgical experience and has authored multiple textbook chapters on musculoskeletal health. Dr. Ross is passionate about patient education and evidence-based medicine.
View all articles →