IT Band Syndrome: Causes, Symptoms & Treatment Canada
Share
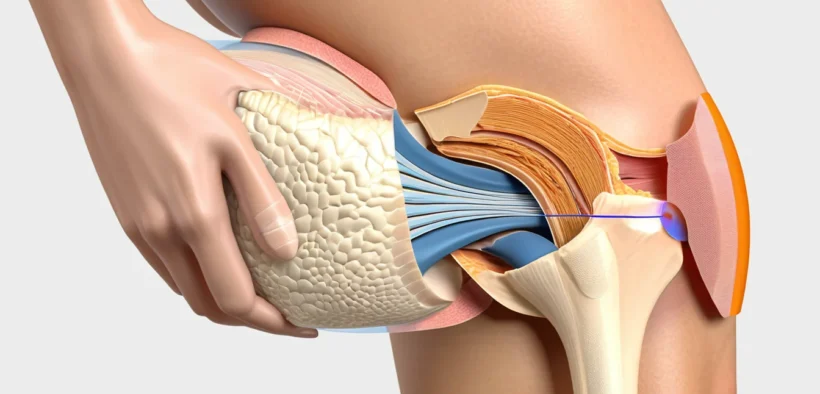
IT band syndrome is one of the most common causes of outer knee pain among active Canadians. It occurs when the iliotibial band — a thick strip of connective tissue running along the outside of your thigh — repeatedly rubs against the knee joint, leading to irritation and inflammation that can sideline you from the activities you enjoy most.
What Causes IT Band Syndrome in Active Canadians?
Whether you run trails in British Columbia, cycle through Ontario, or hike in the Rockies, understanding iliotibial band syndrome treatment options and what causes this condition can help you recover faster. In this guide, we break down the symptoms, diagnosis, proven stretches and exercises, and when it is time to see a Canadian healthcare provider.
What Is IT Band Syndrome?
| Treatment Option | Benefits | Considerations | Timeline for Relief |
|---|---|---|---|
| Rest & Activity Modification | Reduces inflammation; allows tissue healing; no cost | May require significant reduction in training volume; not a long-term solution alone | 1–2 weeks for acute symptoms |
| Physiotherapy | Addresses underlying biomechanical issues; strengthens hip abductors; supervised progression | Multiple sessions required; may involve out-of-pocket costs if not covered by provincial or private insurance | 4–8 weeks with consistent treatment |
| Foam Rolling & Stretching | Improves soft tissue mobility; low cost; can be done at home | Technique must be correct to avoid aggravation; not sufficient as a standalone treatment | Gradual improvement over 2–4 weeks |
| NSAIDs (e.g., Ibuprofen, Naproxen) | Reduces pain and inflammation quickly; available over the counter in Canada | Short-term use only; not suitable for individuals with kidney, gastrointestinal, or cardiovascular conditions | Days to 1–2 weeks for symptom relief |
| Corticosteroid Injection | Provides significant short-term pain relief; useful for severe or persistent cases | Administered by a physician; limited to 2–3 injections; does not address root cause | Days to 1 week post-injection |
| Surgery (ITB Release) | Effective for chronic, refractory IT band syndrome unresponsive to conservative care | Rare and last-resort option; recovery time of several months; referral to orthopaedic surgeon required | 3–6 months post-operative recovery |
The iliotibial (IT) band is a long, tough band of connective tissue. It runs from your hip down the outside of your thigh and attaches just below your knee. Its job is to help stabilize the knee during movement.
When this band becomes too tight or overworked, it can rub against a bony bump on the outside of your knee called the lateral femoral condyle. That repeated friction causes inflammation — and pain. This condition is known as IT band syndrome, and it is sometimes called iliotibial band syndrome or runner’s knee.
According to Mayo Clinic, overuse injuries like IT band syndrome are especially common in endurance athletes. However, you do not have to be an elite athlete to develop it. Everyday Canadians who suddenly increase their activity level are also at risk.
Common Causes of IT Band Syndrome
IT band syndrome is almost always caused by overuse rather than a single injury. The condition develops gradually over time. Several factors can increase your risk.
Repetitive Movement and Overuse
Running, cycling, and hiking involve the same knee motion repeated thousands of times. Over time, this repetition puts stress on the IT band. The band tightens and begins to rub against the knee joint with every stride or pedal stroke.
Runners who increase their mileage too quickly are especially vulnerable. The same goes for cyclists who adjust their seat height incorrectly. In addition, hiking on hilly terrain puts extra strain on the outer knee.
Biomechanical and Training Factors
Certain physical traits and training habits can raise your risk of developing IT band syndrome. These include:
- Weak hip and glute muscles
- Tight hip flexors or IT band
- Running on banked or uneven surfaces
- Worn-out footwear
- Training errors, such as increasing distance or intensity too quickly
- Running in only one direction on a track
A direct blow to the outside of the knee can also trigger the condition, though this is far less common. Most cases develop slowly from repeated stress on the joint.
Symptoms of IT Band Syndrome
The symptoms of IT band syndrome are usually easy to recognize, especially if you are active. The pain tends to follow a predictable pattern.
Pain on the Outside of the Knee
The most common symptom is a sharp or burning pain on the outer side of the knee. This pain usually appears during activity — not at rest. For many people, it starts after running or cycling for a set distance and then fades when they stop.
The pain may also radiate up the outer thigh. Some people feel a clicking or snapping sensation when they bend and straighten their knee. This happens as the IT band slides back and forth over the bony prominence at the side of the knee.
What Is Usually Absent
Unlike some other knee conditions, IT band syndrome does not typically cause joint swelling. Your knee’s range of motion usually stays normal. There is no locking or giving way of the joint.
These features help distinguish IT band syndrome from other conditions, such as a meniscus tear or arthritis. However, a proper diagnosis always requires a professional assessment. Your doctor will consider your symptoms and rule out other possible causes of outer knee pain.
How Is IT Band Syndrome Diagnosed?
Doctors diagnose IT band syndrome mainly by reviewing your symptoms and performing a physical examination. There is no single test that confirms the condition on its own.
Physical Examination
Your doctor will press on the outer side of your knee to check for tenderness. They may also perform a test called the Ober test, which assesses tightness in the IT band. In addition, they will ask about your activity level, training habits, and when the pain started.
Imaging tests like X-rays or MRI scans are not always necessary. However, your doctor may order them to rule out other causes of knee pain, such as a stress fracture or ligament injury. Health Canada encourages Canadians to work with their healthcare providers for accurate diagnosis and appropriate care.
Ruling Out Other Conditions
Several conditions can cause pain on the outside of the knee. These include lateral meniscus tears, lateral collateral ligament sprains, and patellofemoral syndrome. Your doctor will consider all of these possibilities before confirming a diagnosis of IT band syndrome.
Getting the right diagnosis matters because the treatment approach varies significantly between conditions. Do not try to self-diagnose based on symptoms alone.
Treatment Options for IT Band Syndrome
The good news is that most cases of IT band syndrome respond well to non-surgical treatment. With the right approach, most people recover fully and return to their normal activities.
Rest and Activity Modification
The first step in treatment is reducing or temporarily stopping the activity that caused the problem. This does not mean you have to stop all exercise. Low-impact activities like swimming or using a stationary bike with a high seat setting are often well tolerated.
As pain improves, you can gradually return to your usual activity. However, try not to increase intensity or distance too quickly. A gradual return helps prevent the problem from coming back.
Stretching and Strengthening Exercises
Targeted exercises are a cornerstone of IT band syndrome recovery. Stretching the IT band, hip flexors, and glutes can reduce tension along the outer thigh. Strengthening the hip abductor muscles helps correct the underlying muscle imbalances that often contribute to the condition.
A physiotherapist can design a programme tailored to your specific needs. Many provincial health plans in Canada cover physiotherapy visits, at least in part. Check with your provincial health authority to understand your coverage.
Pain Relief Measures
Applying ice to the outside of your knee for 15 to 20 minutes after activity can help manage pain and inflammation. Over-the-counter anti-inflammatory medications like ibuprofen may also provide short-term relief. Always follow the recommended dosage and speak with a pharmacist if you have any concerns.
Foam rolling the outer thigh can help release tightness in the IT band. This is a popular recovery technique among runners and cyclists. According to Healthline, foam rolling may improve tissue flexibility and reduce muscle soreness when used regularly.
When Surgery Is Considered
Surgery for IT band syndrome is rare. Most people recover fully without it. However, if symptoms persist despite several months of conservative treatment, a surgeon may recommend a procedure to release tension in the IT band.
This procedure involves making a small cut in the IT band so that it no longer rubs tightly against the knee. Recovery after surgery typically involves physiotherapy and a gradual return to activity. Surgery is always a last resort and is not necessary for the vast majority of people with this condition.
When to See a Doctor
You should see a doctor if your knee pain is persistent, worsening, or interfering with your daily life. Do not try to push through significant pain, as this can make the injury worse and delay your recovery.
Your family doctor is a great first point of contact. They can assess your knee, refer you to a physiotherapist, and determine whether further investigation is needed. If you do not have a family doctor, a walk-in clinic can provide an initial assessment and help you get the care you need.
Seek care promptly if you notice significant swelling, severe pain, or an inability to bear weight on your leg. These symptoms may point to a more serious injury that needs immediate attention.
Frequently Asked Questions
How long does IT band syndrome take to heal?
Recovery from IT band syndrome varies depending on how severe the condition is and how consistently you follow your treatment plan. Mild cases may improve within a few weeks with rest and stretching. More stubborn cases can take several months to resolve fully.
Can I still run with IT band syndrome?
Running through significant pain is not recommended, as it can worsen IT band syndrome and slow your recovery. However, some people are able to continue light jogging if symptoms are mild and they reduce their distance and pace. It is best to speak with your doctor or physiotherapist before continuing to run.
What exercises help IT band syndrome?
Exercises that strengthen the hip abductors and glutes are especially helpful for IT band syndrome. Side-lying leg raises, clamshells, and single-leg squats are commonly recommended. Stretching the IT band and hip flexors regularly can also reduce tension and prevent recurrence.
Is IT band syndrome the same as runner’s knee?
The term “runner’s knee” can refer to several different conditions, which makes it a little confusing. IT band syndrome is one condition that falls under this umbrella term, but patellofemoral pain syndrome is another. Your doctor can help determine exactly which condition is causing your knee pain.
Does IT band syndrome go away on its own?
In many cases, IT band syndrome does improve with rest and reduced activity. However, simply resting without addressing the underlying causes — such as muscle weakness or training errors — often leads to the problem returning. A structured rehabilitation programme gives you the best chance of a full and lasting recovery.
Is heat or ice better for IT band syndrome?
According to Mayo Clinic’s overview of iliotibial band syndrome, this information is supported by current medical research.
For more information, read our guide on MRI vs CT scan for diagnosing outer knee pain.
Ice is generally recommended for managing acute pain and inflammation from IT band syndrome, especially right after activity. Apply ice wrapped in a cloth to the outer knee for 15 to 20 minutes at a time. Heat may be helpful before activity to warm up the tissue, but speak with your healthcare provider about what works best for your situation.
Key Takeaways
- IT band syndrome is caused by repeated friction between the iliotibial band and the outer knee joint.
- It is most common in runners, cyclists, and hikers, but anyone who increases activity too quickly can develop it.
- Symptoms include burning or sharp pain on the outside of the knee during activity, sometimes with a clicking sensation.
- Diagnosis is based on symptoms and a physical exam; imaging is not always required.
- Most cases respond well to rest, stretching, strengthening exercises, and physiotherapy.
- Surgery is rarely needed and is only considered after other treatments have failed.
- If knee pain is persistent or severe, visit your family doctor or a walk-in clinic for proper assessment.
- As always, speak with your healthcare provider before starting any new treatment or exercise programme.
Frequently Asked Questions
What is IT band syndrome?
IT band syndrome is an overuse injury caused by inflammation of the iliotibial band, a thick strip of connective tissue running along the outer thigh from the hip to the knee. It occurs when the band repeatedly rubs against the lateral femoral epicondyle, causing pain and swelling on the outside of the knee.
What are the symptoms of IT band syndrome?
Common symptoms include a sharp, burning pain on the outer knee or hip, swelling along the iliotibial band, and discomfort that worsens during running, cycling, or stair climbing. Pain typically begins after a consistent distance or duration of activity and may subside with rest, then return once exercise resumes.
How is IT band syndrome treated?
IT band syndrome treatment includes rest, ice application, anti-inflammatory medications like ibuprofen, and physiotherapy. Targeted stretching, foam rolling, and strengthening exercises for the hips and glutes are highly effective. In persistent cases, corticosteroid injections or, rarely, surgery may be recommended by a Canadian sports medicine physician.
How can I prevent IT band syndrome from coming back?
Prevention involves gradually increasing training intensity, strengthening hip abductors and glutes, wearing properly fitted footwear, and incorporating regular stretching and foam rolling into your routine. Avoiding sudden mileage increases, running on cambered surfaces, and addressing biomechanical imbalances with a physiotherapist significantly reduces recurrence risk.
When should I see a doctor for IT band syndrome?
See a doctor if outer knee or hip pain persists beyond two weeks despite rest and home treatment, if swelling or significant bruising develops, or if pain begins interfering with daily activities. A Canadian physiotherapist or sports medicine doctor can confirm the diagnosis and create an individualized recovery plan.
About the Author
Dr. Sarah Mitchell, MDDr. Sarah Mitchell is a board-certified family physician with over 15 years of clinical experience. She completed her MD at the University of Toronto and her residency at Toronto General Hospital. Dr. Mitchell specializes in preventive medicine and chronic disease management. She is a member of the College of Family Physicians of Canada (CFPC) and has published over 30 peer-reviewed articles on preventive health care.
View all articles →
