Pelvic Organ Prolapse: Causes, Symptoms & Treatment
Share
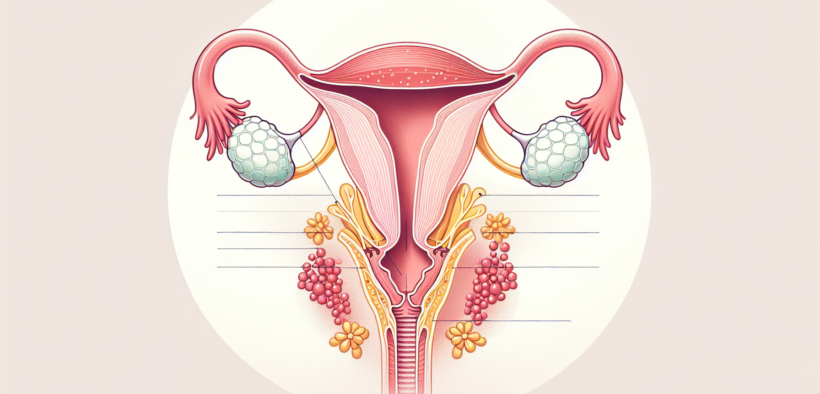
Pelvic organ prolapse is a condition that affects many Canadian women, particularly after childbirth or menopause, yet it remains widely underdiagnosed and rarely discussed. It occurs when the muscles and connective tissues supporting the pelvic organs become stretched or weakened, allowing the bladder, uterus, or rectum to shift downward and press into the vaginal canal. While it can feel alarming, this condition is rarely dangerous and is highly treatable.
Understanding Pelvic Organ Prolapse: Types, Stages & What Happens in Your Body
Pelvic floor weakness is the underlying driver behind most cases of prolapse, and understanding its causes is the first step toward effective management. Whether you are experiencing early symptoms or have already been diagnosed, this guide covers everything Canadian women need to know — from recognizing the signs to exploring surgical and non-surgical treatment options available across Canada’s healthcare system.
What Is Pelvic Organ Prolapse?
Your pelvic organs — the bladder, uterus, rectum, and small intestine — are held in place by a network of muscles, ligaments, and connective tissue. When that support system weakens, one or more organs can drop down and press into the vaginal canal.
There are several types of pelvic organ prolapse, depending on which organ is affected:
- Cystocele — the bladder drops into the vagina. This is the most common type.
- Urethrocele — the urethra (the tube that carries urine out of the body) shifts downward.
- Uterine prolapse — the uterus descends into or beyond the vagina.
- Vaginal vault prolapse — the top of the vagina collapses, often after a hysterectomy.
- Enterocele — part of the small intestine bulges into the vaginal wall.
- Rectocele — the rectum pushes against the back wall of the vagina.
In many cases, a woman may have more than one type at the same time. However, even when prolapse is present, it does not always cause noticeable symptoms.
What Causes Pelvic Organ Prolapse?
The most common cause of pelvic organ prolapse is pregnancy, labour, and vaginal delivery. During childbirth, the muscles, ligaments, and connective tissue of the pelvic floor can stretch, tear, or detach. This damage can reduce the pelvic floor’s ability to support the organs above it.
In addition, nerve damage during a long labour or an assisted delivery — for example, one that uses forceps — can affect muscle control in the pelvic region. When these nerves are injured, the pelvic floor may lose its dome shape and begin to sag downward.
The Role of Oestrogen and Menopause
Oestrogen is a hormone that helps keep pelvic tissues strong and elastic. After menopause, oestrogen levels drop significantly. As a result, the body produces less collagen — a protein that keeps connective tissue firm and flexible. This loss of collagen makes the pelvic floor more vulnerable to prolapse.
Therefore, many women first notice symptoms of pelvic organ prolapse during or after menopause, even if the original tissue damage happened years earlier during childbirth.
Other Contributing Factors
Several other factors can increase pressure on the pelvic floor and raise the risk of prolapse:
- Obesity — extra body weight places constant downward pressure on the pelvic organs.
- Chronic coughing — caused by smoking or lung conditions, repeated coughing strains the pelvic floor over time.
- Constipation — straining during bowel movements puts repeated pressure on pelvic tissues.
- Previous pelvic surgery — a hysterectomy (removal of the uterus), for example for endometriosis, can sometimes weaken the structures that support nearby organs.
- Spinal or muscle conditions — disorders such as multiple sclerosis or muscular dystrophy can affect the nerves and muscles that support the perineum.
Pelvic organ prolapse is rare in women who have never given birth. Furthermore, it tends to become more common with age as tissues naturally lose strength over time.
Recognising the Symptoms of Pelvic Organ Prolapse
Many women with pelvic organ prolapse have no symptoms at all. However, when symptoms do appear, they can range from mild discomfort to significant changes in daily life. Symptoms often feel worse when standing, jumping, or lifting, and they tend to improve when lying down.
Common symptoms of pelvic organ prolapse include:
- A feeling of heaviness or pressure in the pelvis
- A sensation that something is falling out of the vagina
- A pulling or aching feeling in the lower abdomen or lower back
- Pain or discomfort during sexual intercourse (dyspareunia)
- Urinary problems, such as leaking urine (urinary incontinence) or a sudden strong urge to urinate, especially at night
- Bowel difficulties, such as constipation or needing to support the back wall of the vagina to pass gas or stool
How Prolapse Affects Daily Life
For some women, pelvic organ prolapse interferes with exercise, work, or intimate relationships. The discomfort can affect self-confidence and mental wellbeing. It is important to know that you are not alone — this condition is very common — and that help is available through the Canadian healthcare system.
According to the Mayo Clinic’s overview of pelvic organ prolapse, roughly one-third of all women will be affected by some form of pelvic floor disorder during their lifetime.
Risk Factors for Pelvic Organ Prolapse
Some women are more likely to develop pelvic organ prolapse than others. Understanding your personal risk factors can help you take steps to protect your pelvic health.
Key risk factors include:
- Vaginal childbirth, especially multiple deliveries or delivering a large baby
- Menopause and the hormonal changes that come with it
- Excess body weight, which increases abdominal pressure
- Smoking or chronic lung disease that causes ongoing coughing
- Previous pelvic surgery, including hysterectomy
- Family history of prolapse, which suggests a genetic tendency toward weaker connective tissue
- Neurological conditions affecting muscle strength, such as multiple sclerosis
In addition, women of certain ethnic backgrounds may have a higher or lower risk. For example, research suggests that Hispanic women have a higher lifetime risk of prolapse surgery compared to other groups. Your family doctor can help assess your personal risk.
Treatment Options for Pelvic Organ Prolapse
The good news is that pelvic organ prolapse does not always need surgery. Many women manage their symptoms successfully with simple lifestyle changes and non-surgical treatments. The right approach depends on the type and severity of prolapse and how much it affects your quality of life.
Non-Surgical Treatments
Pelvic floor exercises (Kegel exercises) are often the first step. These exercises strengthen the muscles that support the pelvic organs. A pelvic floor physiotherapist — available through most provincial health systems — can teach you how to do them correctly.
Pessaries are small, removable devices inserted into the vagina to support the prolapsed organ. They come in different shapes and sizes, and a doctor or nurse can fit one for you. Pessaries are a safe, effective option for women who prefer to avoid surgery.
Lifestyle changes can also reduce symptoms significantly. These include maintaining a healthy weight, quitting smoking, treating chronic constipation with a high-fibre diet, and avoiding heavy lifting where possible.
Oestrogen therapy may help strengthen pelvic tissues in women who are postmenopausal. This is typically applied as a local vaginal cream or ring. Talk to your doctor about whether hormone therapy is appropriate for you. You can also find helpful guidance through Health Canada’s information on menopause and hormone therapy.
Surgical Options
When non-surgical treatments are not enough, surgery may be recommended. There are several surgical approaches depending on the organs involved and the woman’s overall health. In most cases, the goal of surgery is to restore the organs to their correct position and strengthen the pelvic support structures.
Surgery is typically arranged through a referral from your family doctor or gynaecologist, and it is covered under most provincial health plans in Canada. Recovery times vary, and your surgical team will guide you through what to expect.
For a broader look at pelvic floor health and treatment approaches, Healthline’s guide to pelvic organ prolapse offers reliable, easy-to-read information.
When to See a Doctor
If you notice any of the symptoms described above — especially a feeling of pressure, a bulge in the vaginal area, or urinary leakage — it is a good idea to speak with a healthcare provider. You do not need to wait until symptoms become severe.
Start by booking an appointment with your family doctor. If you do not have a family doctor, a walk-in clinic can assess your symptoms and refer you to a gynaecologist or urogynecologist if needed. Many provinces also have dedicated pelvic health programmes that offer assessments and physiotherapy without a specialist referral.
Remember, pelvic organ prolapse is a medical condition — not something you simply have to live with. Early attention often leads to simpler and more effective treatment. As always, please consult your doctor or a qualified healthcare professional before starting any treatment or making changes to your health routine.
Frequently Asked Questions About Pelvic Organ Prolapse
Can pelvic organ prolapse heal on its own?
In some cases, mild pelvic organ prolapse can improve over time, especially with pelvic floor exercises and lifestyle changes. However, moderate to severe prolapse typically requires treatment such as a pessary or surgery. It is best to speak with your family doctor to find out what is appropriate for your situation.
Is pelvic organ prolapse dangerous?
Pelvic organ prolapse is rarely life-threatening, but it can significantly affect your quality of life. Without treatment, some types of prolapse can worsen over time and lead to problems with bladder or bowel function. Early assessment by a healthcare provider is always recommended.
What does pelvic organ prolapse feel like?
Many women describe a feeling of pelvic pressure or heaviness, or a sensation that something is bulging or falling out of the vagina. Some also experience lower back ache, urinary leakage, or discomfort during sex. Symptoms of pelvic organ prolapse often feel worse after standing for long periods and better after lying down.
Can I exercise if I have pelvic organ prolapse?
Yes, but some exercises may worsen symptoms. High-impact activities like running or heavy lifting can increase pressure on the pelvic floor. A pelvic floor physiotherapist can help design a safe exercise plan that supports recovery while keeping you active.
Is pelvic organ prolapse covered by provincial health insurance in Canada?
Most diagnostic assessments and surgical treatments for pelvic organ prolapse are covered under provincial health plans across Canada. Pelvic floor physiotherapy may be partially covered depending on your province and extended health benefits. Ask your family doctor or walk-in clinic about referral options in your area.
Can pelvic organ prolapse affect sexual activity?
According to Mayo Clinic’s overview of pelvic organ prolapse, this information is supported by current medical research.
For more information, read our guide on managing health conditions through physical activity.
Yes, pelvic organ prolapse can sometimes cause pain or discomfort during intercourse, and it may affect sexual confidence. However, many women find that treating the prolapse — through exercises, a pessary, or surgery — significantly improves their sexual wellbeing. Talk openly with your doctor about any concerns you have.
Key Takeaways
- Pelvic organ prolapse occurs when weakened pelvic muscles and tissues allow one or more pelvic organs to shift out of place.
- The most common causes are childbirth, menopause, and ongoing abdominal pressure from factors like obesity or chronic coughing.
- Symptoms include a feeling of pelvic pressure, urinary leakage, and discomfort during sex — though some women have no symptoms at all.
- Non-surgical treatments such as Kegel exercises, pessaries, and lifestyle changes are effective for many women.
- Surgery is available when needed and is covered under most provincial health plans in Canada.
- If you think you may have pelvic organ prolapse, speak with your family doctor or visit a walk-in clinic — early care makes a real difference.
About the Author
Canada Health JournalCanada Health Journal is a trusted source of evidence-based health information for Canadians. Our content is reviewed by licensed medical professionals including physicians, registered dietitians, and specialists across Canada.
View all articles →