Mastitis Treatment: Causes, Symptoms & Help in Canada
Share
Mastitis treatment is essential for the many Canadian mothers who develop this painful breast infection during the early months of breastfeeding. Mastitis causes pain, swelling, redness, and warmth in the breast and can leave you feeling exhausted and feverish. While it most commonly affects nursing women, it can occur at any stage of life. Recognizing the warning signs early ensures you get effective care before complications arise.
Effective Mastitis Treatment Options in Canada
Understanding mastitis symptoms is the first step toward a faster recovery. In Canada, healthcare providers typically recommend a combination of antibiotics, continued breastfeeding, and home comfort measures to resolve the infection. Because untreated mastitis can progress to a breast abscess, it is important to consult a doctor as soon as you notice breast changes. This guide covers everything Canadian women need to know about causes, risk factors, and the most effective treatment options available.
What Is Mastitis?
| Treatment Option | How It Works | Benefits | Important Considerations |
|---|---|---|---|
| Antibiotics (e.g., Cloxacillin, Cephalexin) | Eliminates bacterial infection, most commonly caused by Staphylococcus aureus | Resolves infection within 10–14 days; safe during breastfeeding | Requires a prescription from a Canadian physician or nurse practitioner; complete the full course to prevent resistance |
| Continued Breastfeeding or Pumping | Keeps milk flowing to prevent blockages and reduce bacterial buildup in the breast | Speeds recovery; maintains milk supply; safe for the baby | Recommended by the Society of Obstetricians and Gynaecologists of Canada (SOGC); stopping abruptly may worsen symptoms |
| Pain Relief (Ibuprofen or Acetaminophen) | Reduces inflammation, fever, and breast pain | Over-the-counter availability across Canada; both are compatible with breastfeeding | Ibuprofen is preferred for its anti-inflammatory properties; consult a pharmacist if taking other medications |
| Warm Compresses and Rest | Improves milk flow, relieves localized pain, and supports immune recovery | Non-pharmacological; can be used alongside other treatments immediately | Apply for 10–15 minutes before feeding; adequate rest is essential and may require support from healthcare providers or family |
| Surgical Drainage (for Abscess) | Drains a pus-filled abscess that has not responded to antibiotic mastitis treatment | Resolves severe infections that antibiotics alone cannot treat | Performed by a physician or surgeon in a hospital or clinic setting; breastfeeding may continue after drainage in most cases |
Mastitis is an infection of the breast tissue. It can cause a firm, tender lump and make you feel exhausted and unwell. In some cases, it can also lead to a fever.
Most cases of mastitis appear in the first three months after birth. However, it can also occur in women who are not breastfeeding, including those going through menopause. In rare cases, a type of breast cancer called inflammatory breast cancer can mimic mastitis, so it is important to get any breast changes checked by a healthcare provider.
How Does Mastitis Develop?
Bacteria normally found in a baby’s mouth can enter the breast through tiny skin breaks. These breaks are often invisible to the naked eye. Once inside, the bacteria travel into the deeper breast tissue and multiply, causing infection.
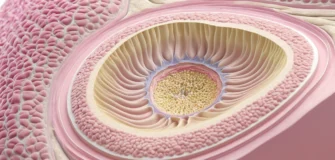
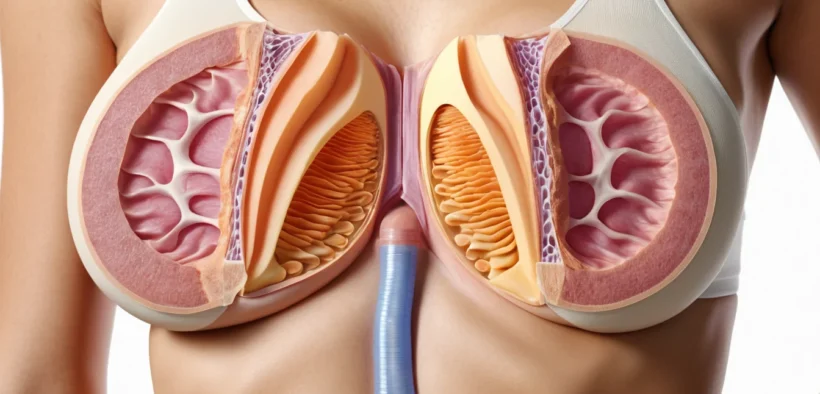
The breast is a complex gland made up of milk-producing lobules, milk ducts, fatty tissue, and connective tissue. When bacteria invade this tissue, the immune system responds with inflammation. This causes the classic signs of redness, swelling, heat, and pain.
What Happens If Mastitis Is Left Untreated?
If not treated properly, mastitis can develop into a breast abscess. An abscess is a pocket of pus that forms deep in the breast tissue. This is a more serious condition and often requires surgical drainage. Therefore, early treatment is essential to prevent complications.
Types of Mastitis
There are two main types of mastitis based on their relationship to breastfeeding and pregnancy.
- Puerperal mastitis: This type occurs during breastfeeding or shortly after childbirth. It is the most common form.
- Non-puerperal mastitis: This type occurs outside of breastfeeding. It can affect women at menopause or those with certain chronic health conditions. In rare cases, it can even affect men with a condition called gynaecomastia (enlarged breast tissue).
It is important to note that not all mastitis is caused by infection. Some cases are non-infectious, meaning no bacteria are involved. However, infection is still the leading cause in most patients.
Risk Factors for Mastitis
Certain factors make a person more likely to develop mastitis. Knowing these risk factors can help you take steps to lower your risk.
- Previous mastitis: If you have had it before, you are more likely to get it again. Mastitis has a recurring nature.
- Skin injuries on the breast: Even small, invisible cracks or sores around the nipple can let bacteria in.
- Incomplete emptying of the breast: When the breast is not fully drained during feeding, milk builds up. This is called breast engorgement and creates conditions where bacteria can grow.
- Tight-fitting bra: A bra that is too tight can restrict milk flow inside the breast.
- Feeding in only one position: Keeping the baby in the same position every time can prevent full drainage of the breast.
- Chronic health conditions: Diabetes or a weakened immune system, including HIV infection, can increase your risk.
In addition, hormonal changes during menopause can block the milk ducts. This can lead to chronic duct inflammation and increase the risk of non-puerperal mastitis.
Symptoms of Mastitis
Mastitis symptoms can come on quickly and feel quite severe. Many women describe feeling like they have the flu before they even notice breast changes.
Common symptoms include:
- A painful, swollen area on one breast
- Redness and warmth in the affected area
- A firm lump or thickening in the breast tissue
- Fever and chills
- Fatigue and general feeling of being unwell
- Burning sensation, especially during breastfeeding
According to Mayo Clinic’s guide on mastitis, symptoms often develop suddenly and can affect your ability to care for your baby. Furthermore, the World Health Organization’s breastfeeding guidelines recommend continuing to breastfeed during mastitis when possible, as stopping suddenly can worsen engorgement.
Mastitis vs. Breast Engorgement
Breast engorgement can feel similar to mastitis. Engorgement happens when the breasts overfill with milk, usually in the first days after birth. It causes tightness, heaviness, and mild warmth. However, engorgement typically affects both breasts and does not cause a high fever. Mastitis usually affects only one breast and often comes with a fever above 38.5°C. If your symptoms include fever or do not improve after 12 to 24 hours of home care, see a doctor.
Treatment for Mastitis
Most cases of mastitis respond well to treatment when caught early. Your doctor will assess your symptoms and recommend the best approach for you.
Antibiotics
If your mastitis is caused by a bacterial infection, your doctor will likely prescribe antibiotics. It is important to finish the full course, even if you start feeling better. Stopping early can allow the infection to return or become harder to treat.
Continuing to Breastfeed
Many healthcare providers in Canada advise mothers to continue breastfeeding or pumping during mastitis treatment. Emptying the breast regularly helps clear the infection. Stopping breastfeeding suddenly can worsen engorgement and may make the infection worse.
Home Care and Comfort Measures
In addition to antibiotics, several home care steps can help relieve symptoms:
- Apply a warm compress to the affected breast before feeding to encourage milk flow.
- Rest as much as possible and stay well hydrated.
- Wear a properly fitted, supportive bra — not too tight.
- Take over-the-counter pain relievers like ibuprofen or acetaminophen to ease pain and reduce fever. Always follow the dosage instructions on the package.
- Try different breastfeeding positions to help drain all parts of the breast evenly.
For more guidance on safe medications while breastfeeding, you can refer to Health Canada’s drug safety resources.
Treating a Breast Abscess
If mastitis develops into an abscess, antibiotics alone may not be enough. A doctor will usually need to drain the abscess. This can be done with a needle under ultrasound guidance or through a small surgical cut. Recovery is generally straightforward with proper care.
When to See a Doctor
Do not wait to get help if you think you have mastitis. Early treatment helps prevent serious complications like a breast abscess.
See your family doctor or visit a walk-in clinic as soon as possible if you notice:
- A red, swollen, or painful area on your breast
- A fever above 38.5°C
- Symptoms that are not improving after 12 to 24 hours
- A hard lump that is not going away
- Discharge from the nipple that is not breast milk
- Symptoms that return after a previous mastitis infection
If you are covered under your provincial health plan, a visit to your family doctor is covered. If you cannot get a same-day appointment, a walk-in clinic can prescribe antibiotics and provide a referral if needed. In severe cases, you may need to visit your nearest emergency department.
It is always a good idea to speak with your doctor or a registered nurse before starting any new treatment. This article is for informational purposes only and does not replace professional medical advice.
Can I keep breastfeeding if I have mastitis?
Yes, in most cases you can and should continue breastfeeding if you have mastitis. Emptying the breast regularly helps the infection clear faster. Your doctor can confirm whether it is safe to continue based on your specific situation.
How long does mastitis last?
With proper treatment, mastitis usually improves within 10 to 14 days. Most women feel better within a few days of starting antibiotics. However, finishing the full course of antibiotics is important to prevent the infection from coming back.
What does mastitis feel like?
Mastitis typically feels like a painful, hot, and swollen area on one breast. Many women also feel feverish, tired, and achy, similar to having the flu. The breast may have a firm lump or a red, wedge-shaped patch on the skin.
Can mastitis go away on its own without antibiotics?
Mild cases of mastitis may improve with rest, frequent breastfeeding, and warm compresses. However, most cases caused by a bacterial infection require antibiotics to clear fully. Without treatment, mastitis can worsen and develop into a breast abscess, which is harder to treat.
Can you get mastitis if you are not breastfeeding?
Yes, mastitis can occur in women who are not breastfeeding, including those going through menopause or with certain chronic health conditions. Non-puerperal mastitis is less common but still requires medical attention. In rare cases, symptoms that look like mastitis may be a sign of inflammatory breast cancer, so always get checked by a doctor.
Is mastitis covered under provincial health plans in Canada?
According to Mayo Clinic’s comprehensive guide to mastitis, this information is supported by current medical research.
For more information, read our guide on learn how bacterial infections like kidney infections are treated in Canada.
Yes, a visit to your family doctor or a walk-in clinic for mastitis is covered under most provincial and territorial health plans in Canada. Your doctor can assess your symptoms, prescribe antibiotics if needed, and refer you to a specialist if your condition is more complex. Always check with your provincial health authority for details on covered services.
Key Takeaways
- Mastitis is a breast infection most common in the first three months after birth, but it can affect anyone at any age.
- It is usually caused by bacteria entering the breast through small skin cracks, leading to pain, swelling, redness, and fever.
- Risk factors include breast engorgement, tight bras, only one feeding position, and weakened immunity.
- Treatment typically involves antibiotics, continued breastfeeding, rest, and warm compresses.
- Untreated mastitis can develop into a breast abscess requiring surgical drainage.
- See your family doctor or walk-in clinic promptly if you notice breast pain with fever or a hard lump that does not go away.
- Always follow your doctor’s advice and complete your full antibiotic course to prevent recurrence.
Frequently Asked Questions
What is mastitis?
Mastitis is a breast tissue infection causing inflammation, pain, swelling, and warmth. It most commonly affects breastfeeding women (lactation mastitis) but can occur in anyone. In Canada, it affects approximately 10–20% of nursing mothers, typically within the first three months postpartum. Bacterial infection, usually Staphylococcus aureus, is the most common cause.
What are the symptoms of mastitis?
Common mastitis symptoms include breast tenderness, swelling, warmth, and redness, often in a wedge-shaped area. Many women also experience flu-like symptoms such as fever above 38.5°C, chills, fatigue, and body aches. In breastfeeding women, pain typically worsens during or after nursing and may affect milk flow.
What is the recommended mastitis treatment in Canada?
Mastitis treatment in Canada typically involves a 10–14 day course of antibiotics, most commonly cloxacillin or cephalexin, prescribed by a physician. Continued breastfeeding or pumping is strongly encouraged to clear the infection. Supportive care includes rest, warm compresses, hydration, and ibuprofen or acetaminophen for pain and fever relief.
Can mastitis go away without antibiotics?
Mild mastitis may resolve without antibiotics if caught early. Frequent breastfeeding, rest, warm compresses, and anti-inflammatory medications can help. However, if symptoms persist beyond 12–24 hours, worsen, or include high fever, Canadian health guidelines recommend seeing a doctor promptly to prevent progression to a painful breast abscess.
When should you see a doctor for mastitis treatment in Canada?
See a doctor immediately if you experience fever above 38.5°C, severe breast pain, red streaking on the skin, or symptoms not improving within 24 hours of home care. In Canada, walk-in clinics, family physicians, or telehealth services like Maple or provincial health lines are accessible options for prompt evaluation and antibiotic prescription.
About the Author
Dr. Sarah Mitchell, MDDr. Sarah Mitchell is a board-certified family physician with over 15 years of clinical experience. She completed her MD at the University of Toronto and her residency at Toronto General Hospital. Dr. Mitchell specializes in preventive medicine and chronic disease management. She is a member of the College of Family Physicians of Canada (CFPC) and has published over 30 peer-reviewed articles on preventive health care.
View all articles →