Breast Mastitis: Causes, Symptoms & Treatment Canada
Share
Breast mastitis is one of the most common inflammatory conditions affecting the breast, causing significant pain, swelling, and discomfort for thousands of Canadians each year. Whether you are a new mother or experiencing symptoms unrelated to breastfeeding, understanding this condition can help you seek timely care and avoid serious complications.
What Is Breast Mastitis and What Causes It?
This comprehensive guide covers everything you need to know about mastitis symptoms breastfeeding mothers frequently encounter, including the different types of breast inflammation, breast abscesses, and when to visit your family doctor or a walk-in clinic in Canada. Recognizing the early warning signs is the first step toward effective treatment and a faster recovery.
Understanding the Breast: A Quick Overview
| Treatment Option | Benefits | Considerations | Typical Duration |
|---|---|---|---|
| Antibiotics (e.g., Cloxacillin, Cephalexin) | Clears bacterial infection effectively; first-line treatment recommended by Health Canada | May affect breast milk; complete full course even if symptoms improve; inform prescriber of penicillin allergy | 10–14 days |
| Continued Breastfeeding or Pumping | Helps drain affected breast, reducing milk stasis and easing pain; safe for infant | May be uncomfortable initially; improper latch can worsen symptoms; lactation consultant support recommended | Throughout recovery |
| Pain Relief (Ibuprofen or Acetaminophen) | Reduces fever, swelling, and discomfort; ibuprofen also acts as anti-inflammatory | Follow dosing guidelines; ibuprofen generally preferred for inflammation; consult pharmacist if breastfeeding | As needed, typically 3–7 days |
| Warm Compresses and Breast Massage | Promotes milk flow, eases blocked ducts, and provides natural pain relief | Should complement—not replace—antibiotic therapy; avoid aggressive massage on severely inflamed tissue | Multiple times daily during recovery |
| Surgical Drainage (for Abscess) | Necessary when a breast abscess develops; removes accumulated pus and prevents spreading infection | Required in approximately 3–11% of breast mastitis cases; performed under local or general anaesthesia at a hospital | Single procedure; follow-up care 1–2 weeks |
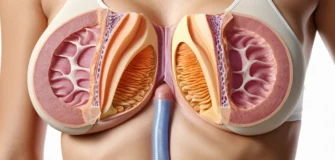
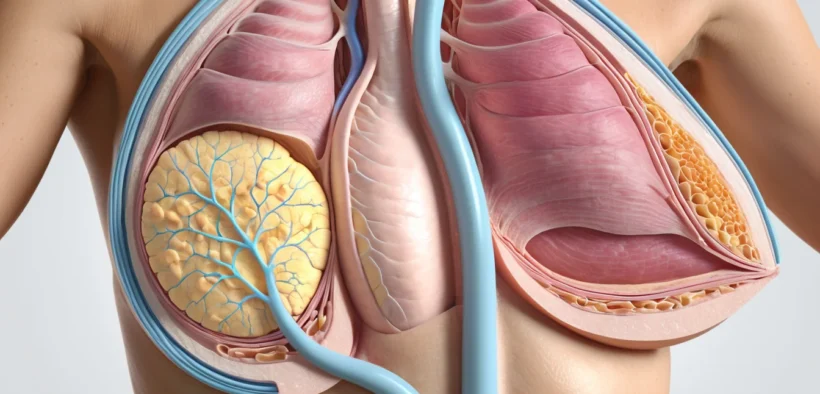
The breast is a glandular organ found in both men and women. In women, it plays an active role in milk production. In men, it exists only in a basic, undeveloped form.
The breast sits on the front wall of the chest and contains glandular tissue, fat, and skin. The glandular tissue is organized into 15 to 20 lobes. Each lobe has its own milk duct that opens at the nipple.
Doctors often divide the breast into five zones, or quadrants, to help locate problems more precisely. Four quadrants surround the nipple, and a fifth central zone sits directly around the areola. This system helps your doctor describe where a lump, infection, or other issue is found.
What Is Breast Mastitis?
Breast mastitis is an inflammation of the breast tissue. It may or may not involve a true abscess, or pocket of pus. It most often affects women who are breastfeeding, but it can occur at any time.
Mastitis makes the breast feel hot, red, swollen, and very tender. Some women also develop a fever and feel generally unwell. In some cases, pus may drain from the nipple when the breast is pressed.
According to the Mayo Clinic’s overview of mastitis, the condition is most common during the first few weeks of breastfeeding. However, it can develop at other times too.
Epidemic Mastitis
Epidemic mastitis involves strains of bacteria — often penicillin-resistant Staphylococcus aureus — that spread through the act of breastfeeding. This type can spread quickly in hospital settings or maternity wards. When combined with other infections, it can become very serious.
The breast becomes extremely painful and red. Pus may appear at the nipple. Treatment includes antibiotics, warm compresses, and regular emptying of the breast.
Non-Epidemic Puerperal Mastitis
This type affects the connective tissue between the breast lobes. It most often develops when cracked nipples allow bacteria to enter the breast. Milk that is not fully drained from the breast also creates an environment where bacteria can grow.
Treatment involves antibiotics and making sure the breast is emptied regularly. Your doctor may recommend continuing to breastfeed or to pump milk to prevent further buildup.
Breast Abscess: When Infection Becomes Localized
A breast abscess is a collection of pus inside the breast tissue. It often develops when mastitis is not treated quickly enough. Abscesses can form in several locations within the breast.
The most common location is just below the areola, known as a subareolar abscess. Other locations include just under the skin, between the breast lobes, or behind the breast tissue itself. One classic sign is a yellow stain left on a cloth or pad when the nipple is gently pressed — this is a helpful early warning sign.
Common symptoms of a breast abscess include:
- Breast pain and tenderness
- Redness and warmth over the skin
- Swelling in one area of the breast
- Fever or general feeling of illness
- Swollen lymph nodes under the arm
For more detailed information on breast infections, Healthline’s guide to breast abscesses offers a helpful overview of symptoms and treatment options.
Chronic Breast Abscess
A chronic abscess develops when an acute mastitis infection does not fully heal. Over time, the area becomes hard and nodular. It may feel like a firm, painful lump under the skin.
Pressing the nipple may produce a purulent, or pus-like, discharge. A needle aspiration — where a doctor uses a small needle to draw out fluid — can confirm the diagnosis. Treatment usually involves repeated incisions to drain the pus, along with thorough cleaning of the area and a course of antibiotics. Severe or recurring cases may require surgical removal of the affected breast tissue.
Galactocele: A Milk-Filled Cyst
A galactocele is a benign cyst that forms in the breast and contains milk. It usually develops after a woman stops breastfeeding. The milk becomes trapped in a blocked duct and forms a smooth, movable lump.
Galactoceles are generally not painful and are not cancerous. However, they can become infected if bacteria enter the cyst. Your doctor can confirm the diagnosis with an ultrasound and, if needed, drain the cyst with a small needle.
Specific vs. Non-Specific Inflammatory Conditions
Inflammatory breast conditions can be either specific or non-specific. Non-specific inflammation is caused by common bacteria, such as Staphylococcus aureus or Streptococcus. These are the most common causes of breast mastitis and abscesses.
Specific inflammatory conditions are less common. They may be linked to underlying conditions such as tuberculosis or other systemic diseases. These require a more targeted treatment approach and further investigation by your doctor.
In addition, some inflammatory breast conditions can mimic the appearance of breast cancer. Therefore, any new lump, redness, or skin change in the breast should always be assessed by a healthcare provider promptly. Health Canada’s breast health resources provide further guidance on breast disease awareness for Canadians.
Breast Lymph Nodes and Why They Matter
The breast drains fluid through a network of lymph vessels. These vessels lead to lymph nodes, which are small glands that filter bacteria and other harmful substances. When the breast becomes infected, nearby lymph nodes often swell in response.
The main groups of lymph nodes related to the breast are found in the armpit (axillary nodes) and along the inside of the chest (internal mammary nodes). Swollen or tender nodes under the arm are often a sign that the body is fighting an infection in the breast. Your doctor will check these nodes during a physical examination.
When to See a Doctor
You should contact your family doctor or visit a walk-in clinic as soon as possible if you notice any of the following:
- A red, hot, or swollen area of the breast that does not improve within 24 hours
- A lump or hardened area that is painful to touch
- Pus or unusual discharge from the nipple
- Fever above 38.5°C alongside breast pain
- Swollen or tender lymph nodes under your arm
Most provincial health plans in Canada cover visits to your family doctor or a walk-in clinic for breast concerns. Do not wait to seek care. Early treatment of breast mastitis and abscesses prevents complications and leads to faster recovery. If you are breastfeeding and develop symptoms, your doctor can advise you on whether it is safe to continue nursing during treatment.
Remember, this article is for general information only. It is not a substitute for professional medical advice. Always consult your doctor or a qualified healthcare provider for diagnosis and treatment.
Frequently Asked Questions About Breast Mastitis
What are the first signs of breast mastitis?
The first signs of breast mastitis usually include breast pain, redness, and warmth in one area of the breast. You may also notice swelling and feel a general sense of illness, similar to having the flu. Some women develop a fever alongside these symptoms.
Can breast mastitis go away on its own without antibiotics?
Mild cases of breast mastitis may sometimes improve with rest, frequent breastfeeding or pumping, and warm compresses. However, most cases require antibiotic treatment to fully clear the infection. It is important to see your doctor early to avoid the infection developing into a more serious abscess.
Can you still breastfeed if you have mastitis?
In most cases, it is safe and even recommended to continue breastfeeding when you have breast mastitis. Emptying the breast regularly helps clear the infection and prevents milk from building up. Your doctor or a lactation consultant can give you personalized advice based on your situation.
What is the difference between mastitis and a breast abscess?
Breast mastitis is a general inflammation of the breast tissue and does not always involve a pocket of pus. A breast abscess, however, is a localized collection of pus that forms inside the breast, often as a complication of untreated mastitis. An abscess usually requires drainage in addition to antibiotic treatment.
Is breast mastitis a sign of cancer?
Breast mastitis is an infection and is not the same as breast cancer. However, a rare type of cancer called inflammatory breast cancer can look very similar to mastitis, with redness, swelling, and warmth. If your symptoms do not improve with antibiotic treatment within a week or two, see your doctor right away for further investigation.
Who is most at risk of developing breast mastitis?
According to Mayo Clinic’s overview of mastitis causes and symptoms, this information is supported by current medical research.
For more information, read our guide on learn about other common bacterial infections like kidney infections.
Breastfeeding women, especially in the first few weeks after delivery, are most at risk of developing breast mastitis. Cracked or sore nipples, infrequent feeding, and incomplete draining of the breast all increase the risk. However, mastitis can also occur in women who are not breastfeeding and, rarely, in men.
Key Takeaways
- Breast mastitis is an inflammation of the breast tissue, most common in breastfeeding women.
- Symptoms include breast pain, redness, warmth, swelling, and sometimes fever.
- A breast abscess is a localized pocket of pus that can develop when mastitis is left untreated.
- A galactocele is a benign milk-filled cyst that usually develops after stopping breastfeeding.
- Swollen lymph nodes under the arm often accompany a breast infection.
- Treatment typically includes antibiotics, warm compresses, and regular emptying of the breast.
- Always visit your family doctor or a walk-in clinic early if you notice signs of breast inflammation.
- Your provincial health plan covers assessment of breast concerns — do not delay seeking care.
Frequently Asked Questions
What is breast mastitis?
Breast mastitis is an inflammation of breast tissue, often caused by a bacterial infection. It most commonly affects breastfeeding women (lactation mastitis) but can occur in anyone. It develops when bacteria enter the breast through cracked nipples or blocked milk ducts, causing painful swelling, redness, and warmth in the affected area.
What are the symptoms of breast mastitis?
Common symptoms of breast mastitis include breast pain, swelling, warmth, and redness. Many women also experience flu-like symptoms such as fever above 38.5°C, chills, fatigue, and body aches. The affected breast may feel hard or have a tender lump. Symptoms typically appear suddenly and worsen without treatment.
How is breast mastitis treated in Canada?
Breast mastitis is typically treated with a 10–14 day course of antibiotics prescribed by a doctor. Continuing to breastfeed or regularly expressing milk helps clear the infection. Ibuprofen or acetaminophen can relieve pain and fever. Most cases resolve fully with treatment, but a breast abscess may require drainage if infection worsens.
How can I prevent mastitis while breastfeeding?
Prevent mastitis by ensuring your baby latches correctly to avoid cracked nipples. Feed frequently or express milk regularly to prevent blocked ducts. Keep nipples clean and dry, alternate feeding positions, and avoid tight-fitting bras. Staying well-hydrated and rested also supports immune function and reduces your risk of developing an infection.
When should I see a doctor for breast mastitis?
See a doctor promptly if you experience breast pain with redness, swelling, or a fever over 38.5°C lasting more than 24 hours. Seek immediate care if symptoms worsen despite antibiotics, you notice pus discharge, or a painful lump develops — this may indicate a breast abscess requiring urgent medical treatment.
About the Author
Dr. Linda Chen, RD, PhDDr. Linda Chen is a registered dietitian and PhD in Nutritional Sciences from the University of British Columbia. With expertise in clinical nutrition, sports dietetics, and gut health, she has worked with leading Canadian hospitals and sports organizations. Dr. Chen is a member of Dietitians of Canada and regularly contributes to national nutrition policy discussions.
View all articles →