Burning Mouth Syndrome: Causes, Symptoms & Treatment Canada
Share
Burning mouth syndrome is a chronic condition that causes a persistent burning or scalding sensation in the mouth, tongue, gums, or throat, and it affects thousands of Canadians who often go years without a proper diagnosis. The discomfort can feel like you have just sipped a scorching hot drink, yet there are no visible signs of injury or irritation in the mouth.
What Causes Burning Mouth Syndrome in Canadian Patients?
Understanding the burning tongue causes behind this condition is the first step toward finding relief. Whether the problem stems from nerve damage, nutritional deficiencies, or hormonal changes, Canadian patients have effective treatment options available through their healthcare providers. In this article, we explain who is most at risk, how to recognize the symptoms, and what steps you can take to manage and treat this painful condition.
What Is Burning Mouth Syndrome?
| Treatment Option | How It Works | Potential Benefits | Considerations |
|---|---|---|---|
| Clonazepam (Topical or Oral) | Benzodiazepine that modulates GABA receptors to reduce nerve pain signals | Shown to reduce burning intensity; topical use minimizes systemic side effects | Risk of dependency with oral use; requires prescription from a Canadian physician |
| Tricyclic Antidepressants (e.g., Amitriptyline) | Alters neurotransmitter levels to interrupt chronic pain pathways | Effective for neuropathic pain; low doses often sufficient | Side effects include dry mouth and drowsiness; not recommended for older adults without careful monitoring |
| Cognitive Behavioural Therapy (CBT) | Addresses psychological factors and pain perception through structured therapy sessions | Long-term symptom relief; no medication side effects; available through provincial health programs | Requires multiple sessions; waitlists may apply in some Canadian provinces |
| Alpha-Lipoic Acid (Supplement) | Antioxidant that may protect nerve tissue and reduce neuropathic discomfort | Non-prescription option; some clinical evidence supports modest symptom improvement | Evidence is mixed; should be discussed with a healthcare provider before use |
| Capsaicin (Topical) | Desensitizes pain receptors (TRPV1) in oral mucosa over repeated application | Can reduce burning sensation with consistent use | May initially worsen symptoms; low-dose oral rinse form better tolerated than high-concentration versions |
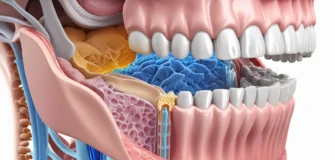
Burning mouth syndrome (also called glossodynia or stomatodynia) is a long-lasting condition. It causes a strong burning or scalding sensation in the mouth without any visible signs of irritation or injury.
The burning feeling can affect the tongue, cheeks, gums, the roof of the mouth, and even the throat. In addition to pain, some people also experience a bitter or metallic taste, a dry mouth feeling, or tingling and numbness in the tongue.
This condition can seriously affect quality of life. It may disrupt sleep, lower mood, and lead to anxiety or depression over time. However, with the right treatment plan, symptoms can be managed effectively.
Types of Burning Mouth Syndrome
Doctors generally recognize two types of burning mouth syndrome: primary and secondary.
Primary Burning Mouth Syndrome
Primary burning mouth syndrome has no clear, identifiable cause. Some researchers believe it may be linked to damage in the nerve fibres responsible for pain and taste in the tongue. This type is also called idiopathic burning mouth syndrome.
Secondary Burning Mouth Syndrome
Secondary burning mouth syndrome is caused by an underlying health condition or external factor. Once the root cause is treated, symptoms often improve. This is why finding the right diagnosis is so important.
Common Causes of Burning Mouth Syndrome
The exact cause of burning mouth syndrome can be difficult to pinpoint. However, researchers have linked it to a wide range of health conditions and lifestyle factors. According to the Mayo Clinic’s overview of burning mouth syndrome, several underlying issues may trigger or worsen the condition.
Common causes include:
- Dry mouth (xerostomia): Often caused by certain medications or health conditions that reduce saliva production.
- Nutritional deficiencies: Low levels of iron, zinc, folate (vitamin B9), thiamine (vitamin B1), riboflavin (vitamin B2), pyridoxine (vitamin B6), or cobalamin (vitamin B12) can all contribute.
- Acid reflux (GERD): Stomach acid that travels up the esophagus can reach the mouth and irritate the tissues.
- Hormonal changes: Burning mouth syndrome is strongly linked to menopause and related hormonal shifts.
- Anxiety and depression: Mental health conditions are frequently associated with this syndrome.
- Allergic reactions: Some people react to certain foods, food additives, flavourings, or oral care products.
- Certain medications: Blood pressure medications, especially ACE inhibitors, are a known trigger.
- Dental issues: Poorly fitted dentures or teeth that damage the inner lining of the mouth can contribute.
- Oral habits: Teeth grinding (bruxism), biting the tongue, or excessive use of mouthwash can all irritate the mouth.
- Excessive acidic drinks: Drinking large amounts of carbonated or acidic beverages can cause ongoing irritation.
Once burning mouth syndrome develops, it can persist for many years. As a result, early diagnosis and treatment are key to improving daily comfort.
Who Is at Risk?
Burning mouth syndrome is not a common condition, but it does affect a significant number of Canadians. It is far more common in women than in men. Most people first notice symptoms around the age of 50 to 60, often around the time of menopause.
Furthermore, certain factors may increase a person’s risk of developing this condition:
- A history of recurring upper respiratory infections
- Previous complex dental procedures
- Known food allergies
- Long-term use of certain medications
- Ongoing stress or emotional difficulties
It is important to note that symptoms can appear suddenly and without any obvious trigger. Therefore, even people without known risk factors can develop burning mouth syndrome.
Symptoms of Burning Mouth Syndrome
The most recognisable symptom of burning mouth syndrome is a burning, scalding, or hot sensation in the mouth. This feeling most often affects the tongue, but it can also spread to the gums, cheeks, palate, and throat.
Other symptoms include:
- Tingling or numbness in the mouth or on the tip of the tongue
- A persistent sensation of dry mouth
- Loss of taste or a change in taste, such as a bitter or metallic flavour
- Diffuse pain that gets worse throughout the day
A Distinctive Pattern of Pain
One of the most telling features of this condition is its daily pattern. Symptoms are often minimal or completely absent in the morning. However, the pain gradually builds through the day and reaches its peak by evening.
This pattern can disrupt sleep and make it harder to get through a normal day. In some cases, the discomfort leads to irritability, mood changes, anxiety, and depression. According to Healthline’s guide to burning mouth syndrome, this progressive daily pain pattern is one of the key signs that helps doctors identify the condition.
It is also worth noting that burning mouth syndrome does not cause visible changes inside the mouth. There are no sores, redness, or swelling that can be seen during a routine dental exam. This is one reason why the condition is often missed or misdiagnosed for years.
When to See a Doctor or Dentist in Canada
You should see a healthcare provider if you notice a persistent burning or painful feeling in your mouth, tongue, or gums. Do not wait to see if it goes away on its own. Early treatment leads to better outcomes.
In Canada, your first step should be visiting your family doctor or a walk-in clinic. Most provincial health plans cover an initial consultation. Your doctor or dentist will ask about your symptoms, medications, and health history.
If symptoms continue or no clear cause is found, you may be referred to a specialist. Depending on your situation, this could include a dermatologist, an ear nose and throat (ENT) specialist, or a mental health professional. This is because burning mouth syndrome is often connected to other health conditions that require a team approach.
For more information on finding a healthcare provider in your area, visit Health Canada’s official health resources page.
Always speak with your doctor before starting any new treatment or supplement. This article is for general information only and is not a substitute for professional medical advice.
How Is Burning Mouth Syndrome Treated?
Treatment for burning mouth syndrome is highly individual. What works for one person may not work for another. Your healthcare provider will build a treatment plan based on your specific symptoms, medical history, and any underlying conditions.
Treating the Underlying Cause
If a clear cause is found, treating it is the first priority. For example, if a nutritional deficiency is responsible, supplements may be recommended. If a medication is causing the problem, your doctor may adjust your prescription. If acid reflux is a trigger, managing GERD through diet and medication can bring relief.
Symptom Management
When no underlying cause can be identified, treatment focuses on relieving symptoms. Your doctor may consider options such as:
- Medications to manage nerve pain
- Low-dose antidepressants or anti-anxiety medications to help with both mood and pain
- Saliva substitutes or medications to treat dry mouth
- Cognitive behavioural therapy (CBT) to help manage the emotional impact of chronic pain
- Dietary changes to avoid triggers like acidic foods and drinks
In many cases, a combination of these approaches provides the best results. Patients who follow a treatment plan tailored to their needs often see a significant improvement in their symptoms and overall quality of life.
Frequently Asked Questions About Burning Mouth Syndrome
What does burning mouth syndrome feel like?
Burning mouth syndrome causes a hot, scalding, or tingling sensation inside the mouth, most often on the tongue. Some people also notice a bitter or metallic taste, or a persistent feeling of dry mouth. The sensation is similar to the feeling of burning your mouth with a hot drink.
What triggers burning mouth syndrome?
Burning mouth syndrome can be triggered by nutritional deficiencies, hormonal changes such as menopause, acid reflux, certain medications, dry mouth, or anxiety and depression. In some cases, no clear trigger is found and the condition is called primary or idiopathic burning mouth syndrome. Identifying a trigger is the first step toward effective treatment.
Can burning mouth syndrome go away on its own?
In some cases, symptoms of burning mouth syndrome do improve or resolve on their own over time. However, for many people, the condition becomes chronic and can last for years without treatment. Seeking medical advice early gives you the best chance of finding relief sooner.
Is burning mouth syndrome linked to anxiety or stress?
Yes, burning mouth syndrome is frequently associated with anxiety, stress, and depression. It is not fully clear whether mental health conditions cause the syndrome or whether living with chronic oral pain leads to emotional distress. Either way, addressing mental health is often an important part of managing this condition.
Who should I see in Canada if I think I have burning mouth syndrome?
Start by booking an appointment with your family doctor or visiting a walk-in clinic, as most provincial health plans cover this type of consultation. Your doctor may refer you to a dentist, dermatologist, ENT specialist, or mental health professional depending on your symptoms. A team approach is often the most effective way to manage burning mouth syndrome.
What vitamins are linked to burning mouth syndrome?
According to Mayo Clinic’s overview of burning mouth syndrome, this information is supported by current medical research.
For more information, read our guide on listeria infection symptoms and treatment in Canada.
Deficiencies in several B vitamins are commonly linked to burning mouth syndrome, including B1 (thiamine), B2 (riboflavin), B6 (pyridoxine), B9 (folate), and B12 (cobalamin). Low levels of iron and zinc may also play a role. A simple blood test from your family doctor can check for these deficiencies.
Key Takeaways
- Burning mouth syndrome causes a chronic burning or scalding feeling in the mouth, tongue, gums, or throat.
- The condition can be primary (no known cause) or secondary (linked to an underlying health issue).
- Common causes include nutritional deficiencies, menopause, acid reflux, dry mouth, certain medications, and anxiety.
- Symptoms often follow a daily pattern, starting mild in the morning and worsening throughout the day.
- Women between the ages of 50 and 60 are most commonly affected.
- Treatment is individualized and may include managing an underlying condition, medication, dietary changes, or cognitive behavioural therapy.
- If you notice persistent burning or pain in your mouth, speak with your family doctor, dentist, or visit a walk-in clinic. Early attention leads to better outcomes.
Frequently Asked Questions
What is burning mouth syndrome?
Burning mouth syndrome is a chronic condition causing a persistent burning, tingling, or scalding sensation in the mouth, often affecting the tongue, lips, gums, or palate. It occurs without an obvious visible cause. It primarily affects postmenopausal women but can develop in anyone, significantly impacting daily eating, drinking, and quality of life.
What are the symptoms of burning mouth syndrome?
Common symptoms include a burning or scalding sensation on the tongue, lips, gums, or inner cheeks, dry mouth, bitter or metallic taste, and numbness. Symptoms often worsen throughout the day, may appear suddenly or gradually, and can persist for months or years without proper diagnosis and treatment.
How is burning mouth syndrome treated in Canada?
Treatment for burning mouth syndrome focuses on managing symptoms since no universal cure exists. Options include cognitive behavioural therapy, clonazepam, alpha-lipoic acid supplements, antidepressants, and saliva substitutes for dry mouth. Canadian physicians typically tailor treatment to underlying causes, such as hormonal changes, nutritional deficiencies, or anxiety disorders.
Can burning mouth syndrome be prevented?
Prevention is not always possible, but certain strategies may reduce risk. Avoiding irritants like acidic foods, alcohol-based mouthwashes, and tobacco helps. Staying hydrated, managing stress, addressing nutritional deficiencies (especially B vitamins, iron, and zinc), and treating underlying conditions like diabetes or acid reflux may lower your chances of developing symptoms.
When should you see a doctor for burning mouth syndrome?
See a doctor or dentist if you experience persistent mouth burning lasting more than several days with no obvious cause, such as a known burn or irritation. Seek prompt attention if symptoms are accompanied by significant dry mouth, taste changes, or difficulty eating, as early diagnosis helps rule out serious underlying conditions.
About the Author
Dr. Linda Chen, RD, PhDDr. Linda Chen is a registered dietitian and PhD in Nutritional Sciences from the University of British Columbia. With expertise in clinical nutrition, sports dietetics, and gut health, she has worked with leading Canadian hospitals and sports organizations. Dr. Chen is a member of Dietitians of Canada and regularly contributes to national nutrition policy discussions.
View all articles →