Patellofemoral Pain Syndrome: Causes & Treatment Canada
Share
Patellofemoral pain syndrome is one of the most common causes of knee pain affecting Canadians of all ages. This condition develops around the kneecap and can turn simple daily activities like climbing stairs, sitting for long periods, or going for a walk into painful experiences. It is especially prevalent among teenagers, runners, and physically active adults across Canada.
What Causes Patellofemoral Pain Syndrome in Canadians?
Often referred to as runner’s knee in Canada, patellofemoral pain syndrome occurs when the cartilage beneath the kneecap becomes irritated, softened, or worn down due to overuse, misalignment, or muscle imbalances. The good news is that most people recover fully with the right combination of rest, physiotherapy, and lifestyle changes. In this comprehensive guide, you will learn exactly what causes anterior knee pain symptoms, how to recognize the warning signs early, and which evidence-based treatment options are available to help you get back to an active, pain-free life.
What Is Patellofemoral Pain Syndrome?
| Treatment Option | Primary Benefits | Key Considerations | Typical Timeline |
|---|---|---|---|
| Physiotherapy & Exercise Rehabilitation | Strengthens quadriceps, hip abductors, and glutes to correct patellar tracking; reduces long-term recurrence | Requires consistent commitment; best supervised by a registered physiotherapist (PT) in Canada | 6–12 weeks for noticeable improvement |
| NSAID Medications (e.g., Ibuprofen, Naproxen) | Reduces acute inflammation and pain, improving mobility during early recovery | Not recommended for long-term use; consult a physician; may interact with other medications | Short-term use, typically 1–2 weeks |
| Patellar Taping & Bracing | Provides immediate pain relief by repositioning the kneecap; allows continued low-impact activity | Should be fitted by a trained clinician; not a standalone solution; skin irritation possible with tape | Ongoing use during activity as needed |
| Activity Modification & Rest | Reduces mechanical load on the patellofemoral joint; prevents symptom aggravation | Complete rest is discouraged; low-impact alternatives like swimming or cycling are recommended | 2–6 weeks alongside active rehabilitation |
| Orthotics & Footwear Correction | Corrects biomechanical issues such as overpronation that contribute to abnormal patellar tracking | Custom orthotics available through podiatrists; coverage may vary by provincial health plan or extended benefits | Ongoing; reassessed every 1–2 years |
| Surgical Intervention (Rare) | Addresses structural abnormalities unresponsive to conservative care; options include lateral release or tibial tubercle realignment | Reserved for severe, refractory cases; risks include infection and prolonged recovery; refer to an orthopaedic surgeon | Recovery typically 3–6 months post-surgery |
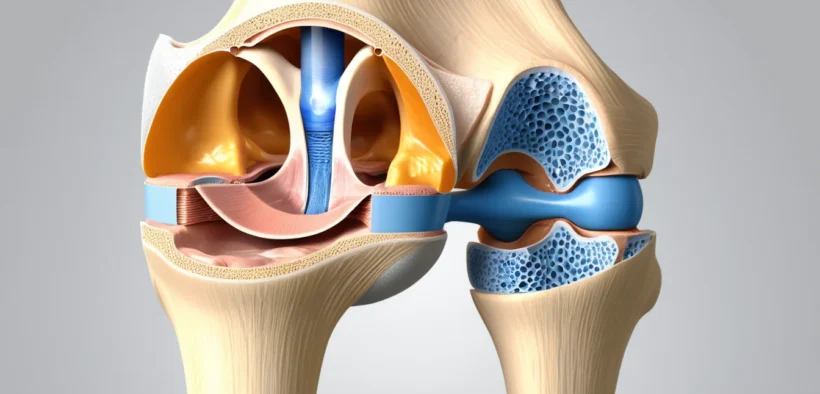
The knee is made up of bones, cartilage, and soft tissue that all work together. The patella, or kneecap, sits at the front of the knee and glides along a groove in the thighbone when you move. Patellofemoral pain syndrome happens when the cartilage under the kneecap becomes irritated, softened, or worn down.
This condition is sometimes called “runner’s knee.” However, you do not have to be a runner to develop it. It can affect anyone who puts repeated stress on the knee joint. According to the Mayo Clinic, patellofemoral pain syndrome is one of the most frequently diagnosed knee conditions worldwide.
Common Causes of Patellofemoral Pain Syndrome
Several factors can lead to patellofemoral pain syndrome. Understanding the cause helps your doctor choose the best treatment for you.
Overuse and Physical Activity
Repeated knee movements, such as running, jumping, or cycling, can put too much stress on the kneecap. Over time, this wears down the cartilage underneath it. Athletes and people who suddenly increase their activity level are at higher risk.
Kneecap Misalignment
Sometimes the kneecap does not track properly along its groove in the thighbone. This misalignment causes uneven pressure on the cartilage. Weak thigh muscles or tight tendons can make this worse.
Excess Body Weight
Carrying extra weight puts added pressure on the knee joint with every step you take. This increases the wear and tear on the cartilage over time. Maintaining a healthy body weight can help protect your knees in the long run.
Previous Knee Injury
A past knee injury, such as a sprain or a direct blow to the kneecap, can damage the cartilage. This damage may lead to patellofemoral pain later in life. In addition, poor recovery from a past injury can leave the knee more vulnerable to future problems.
Recognizing the Symptoms
The symptoms of patellofemoral pain syndrome can range from mild to severe. They often get worse with activity and improve with rest. Knowing what to look for can help you seek care sooner.
Pain at the Front of the Knee
The most common symptom is a dull, aching pain at the front of the knee, around or behind the kneecap. The pain often gets worse when you bend your knees. Activities like squatting, kneeling, climbing stairs, or sitting for long periods can trigger it.
Knee Giving Way
Some people notice that their knee suddenly gives out or buckles unexpectedly. This happens when the muscles around the knee are too weak to support the joint. It can be a startling and dangerous symptom, especially on stairs or uneven ground.
Clicking or Grinding Sensations
You may hear or feel a clicking, popping, or grinding sensation when you move your knee. This is caused by the rough cartilage surface moving against the bone. Furthermore, some people feel a general sense of instability in the knee during walking or physical activity.
How Is Patellofemoral Pain Syndrome Diagnosed?
If you are experiencing knee pain, your family doctor or walk-in clinic can start the diagnostic process. A proper diagnosis is important before starting any treatment. Do not try to self-diagnose based on symptoms alone.
Physical Examination
Your doctor will ask about your symptoms, your activity level, and your medical history. They will then examine your knee, checking for tenderness, swelling, and range of motion. They may also watch you walk or squat to assess how your kneecap moves.
Imaging Tests
In some cases, your doctor may order an X-ray to rule out other bone problems. A magnetic resonance imaging (MRI) scan may also be recommended. An MRI gives a detailed view of the soft tissues, cartilage, and structures inside the knee joint.
Treatment Options for Patellofemoral Pain Syndrome
The good news is that most cases of patellofemoral pain syndrome improve with non-surgical treatment. Your doctor will create a plan based on the severity of your condition. Treatment usually involves a combination of rest, exercise, and pain management.
Rest and Activity Modification
The first step is often to reduce or avoid activities that make your pain worse. This does not mean you have to stop moving entirely. However, high-impact activities like running and jumping should be limited until your knee heals.
Avoid prolonged kneeling or sitting with deeply bent knees. If you use a stationary bike, set the seat at the right height so your legs are not fully extended at the lowest pedal position. Your feet should push down with a smooth, even motion without rocking your hips from side to side.
Pain Relief Medications
Over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and swelling. Common options include ibuprofen (such as Advil) and naproxen (such as Aleve). Always follow the dosage instructions on the package and speak with your pharmacist before starting any new medication.
Ice and Rest
Applying ice to the knee for 15 to 20 minutes at a time can reduce swelling and ease pain. Wrap the ice pack in a cloth to protect your skin. Rest the joint as much as possible during flare-ups.
Physiotherapy and Strengthening Exercises
A physiotherapist can design a programme of exercises to strengthen the muscles around your knee. Strong quadriceps muscles at the front of the thigh help support the kneecap and keep it tracking properly. Stretching exercises are also important to improve flexibility and reduce strain on the joint.
Exercises that deeply bend the knee, such as deep squats or lunges past 90 degrees, should be avoided during recovery. Your physiotherapy programme will focus on controlled, low-impact movements. As your strength improves, you can gradually return to more demanding activities.
Knee Support and Bracing
An elastic knee brace or patellar taping can help stabilize the kneecap during activity. These supports are widely available at pharmacies across Canada. Ask your pharmacist or physiotherapist which type is most appropriate for your needs.
Surgical Treatment
Surgery is rarely needed for patellofemoral pain syndrome. It is only considered when all other treatments have failed and symptoms remain severe. If surgery is ever discussed, your orthopedic specialist will explain the options and risks clearly.
When to See a Doctor
You should visit your family doctor or a walk-in clinic if your knee pain has lasted more than a few days and does not improve with rest. You should also seek care if the pain is severe, your knee swells up, or your knee gives out suddenly. Do not wait too long, as early treatment leads to better outcomes.
Your family doctor can assess your knee and refer you to a physiotherapist or orthopedic specialist if needed. Most provincial health plans in Canada cover physiotherapy referrals and specialist visits when ordered by a physician. Visit Health Canada for information on healthcare coverage and services available in your province.
If you are unsure whether your symptoms require urgent care, a walk-in clinic is a convenient option. Walk-in clinics across Canada can assess knee pain and order imaging tests if necessary. Always consult a qualified healthcare professional before starting any new treatment plan.
What is patellofemoral pain syndrome and who does it affect?
Patellofemoral pain syndrome is a condition that causes pain at the front of the knee, around the kneecap. It commonly affects teenagers, runners, cyclists, and active adults. However, it can develop in anyone who puts repeated stress on the knee joint.
How long does patellofemoral pain syndrome take to heal?
Recovery time varies depending on the severity of the condition and how consistently you follow your treatment plan. Mild cases of patellofemoral pain syndrome may improve within a few weeks with rest and physiotherapy. More severe cases can take several months to fully resolve.
Can I still exercise with patellofemoral pain syndrome?
Yes, but you need to modify your activities to avoid movements that worsen the pain. Low-impact exercises like swimming or stationary cycling are generally well tolerated with patellofemoral pain syndrome. Always check with your physiotherapist or family doctor before continuing or starting a new exercise routine.
Is patellofemoral pain syndrome the same as runner’s knee?
Yes, patellofemoral pain syndrome is often called runner’s knee because it is very common in runners. However, the condition can affect anyone, not just athletes. The term refers to the same type of kneecap irritation and cartilage stress regardless of what caused it.
Does patellofemoral pain syndrome require surgery?
Surgery is rarely needed for patellofemoral pain syndrome. Most people recover well with rest, physiotherapy, and pain management. Surgery is only considered when symptoms are severe and all other treatments have not provided relief after an extended period.
Can patellofemoral pain syndrome come back after treatment?
According to Mayo Clinic’s guide to patellofemoral pain syndrome, this information is supported by current medical research.
For more information, read our guide on MRI vs CT scan for diagnosing knee pain.
Yes, patellofemoral pain syndrome can recur, especially if you return too quickly to high-impact activities. Continuing your strengthening exercises and maintaining a healthy weight can help prevent it from coming back. Your physiotherapist can guide you on a safe return-to-activity plan.
Key Takeaways
- Patellofemoral pain syndrome causes pain at the front of the knee, around the kneecap.
- It is common in teenagers, runners, and active adults, but can affect anyone.
- Main causes include overuse, kneecap misalignment, excess body weight, and past knee injuries.
- Symptoms include front knee pain, a clicking or grinding sensation, and the knee giving way.
- Most cases improve with rest, physiotherapy, ice, NSAIDs, and activity changes.
- Surgery is rarely needed and is only considered as a last resort.
- See your family doctor or visit a walk-in clinic if your knee pain does not improve within a few days.
- Always consult a healthcare professional before beginning any new treatment plan.
Frequently Asked Questions
What is patellofemoral pain syndrome?
Patellofemoral pain syndrome is a condition causing pain around or behind the kneecap (patella) where it meets the thighbone (femur). It commonly affects runners, cyclists, and active individuals. The pain typically results from cartilage irritation, muscle imbalances, or poor kneecap alignment and often worsens with prolonged sitting, squatting, or stair climbing.
What are the symptoms of patellofemoral pain syndrome?
The most common symptoms of patellofemoral pain syndrome include a dull, aching pain at the front of the knee, increased discomfort when climbing stairs, squatting, kneeling, or sitting for long periods. Some people experience a grinding or clicking sensation in the knee. Swelling is less common but can occasionally occur.
How is patellofemoral pain syndrome treated in Canada?
Treatment typically includes rest, activity modification, physiotherapy, and targeted exercises to strengthen the quadriceps and hip muscles. A physiotherapist may recommend orthotics, taping techniques, or bracing. Over-the-counter pain relievers like ibuprofen can manage discomfort. Most Canadians recover fully with conservative treatment over several weeks to months.
Can patellofemoral pain syndrome be prevented?
Yes, patellofemoral pain syndrome can often be prevented by maintaining strong quadriceps and hip muscles, wearing proper footwear, and gradually increasing exercise intensity. Avoiding sudden changes in training volume, using correct running form, and stretching regularly can significantly reduce your risk of developing this common knee condition.
When should I see a doctor for knee pain?
See a doctor if your knee pain is severe, persists beyond a few weeks, or significantly limits daily activities. Seek immediate medical attention if your knee is swollen, locked, gives way suddenly, or was injured in a fall or collision. A Canadian family doctor or sports medicine physician can provide an accurate diagnosis and referral.
About the Author
Dr. Linda Chen, RD, PhDDr. Linda Chen is a registered dietitian and PhD in Nutritional Sciences from the University of British Columbia. With expertise in clinical nutrition, sports dietetics, and gut health, she has worked with leading Canadian hospitals and sports organizations. Dr. Chen is a member of Dietitians of Canada and regularly contributes to national nutrition policy discussions.
View all articles →