Knee Plica Syndrome: Causes, Symptoms & Treatment Canada
Share
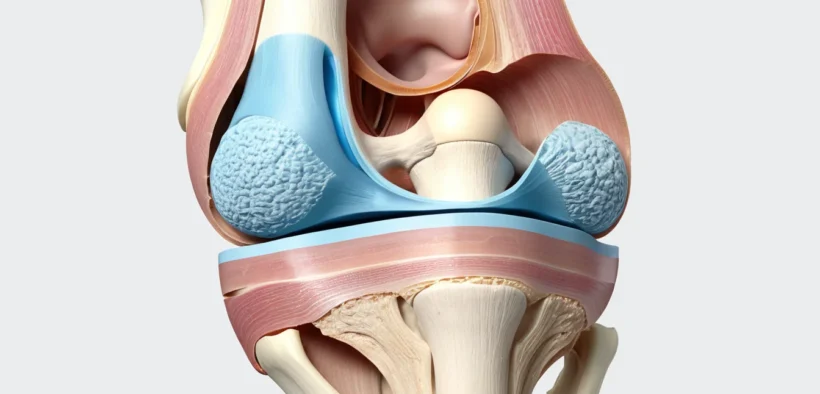
Knee plica syndrome is a common but often overlooked condition that causes persistent pain, swelling, and discomfort in the knee joint. It occurs when a thin fold of tissue inside the knee, called a plica, becomes irritated or inflamed. Many Canadians live with this condition for months without a proper diagnosis because its symptoms closely mimic other knee injuries.
What Causes Knee Plica Syndrome in Canadians?
Understanding plica syndrome symptoms early can make a significant difference in recovery time and quality of life. Whether the irritation stems from overuse, a sports injury, or an underlying inflammatory condition, knowing what to look for helps Canadians seek timely treatment. This guide covers everything you need to know about the causes, diagnosis, and treatment options available across Canada.
What Is Knee Plica Syndrome?
| Treatment Option | How It Works | Benefits | Considerations |
|---|---|---|---|
| Rest & Activity Modification | Reduces repetitive stress on the inflamed plica tissue by limiting aggravating movements | Non-invasive, no cost, effective for mild cases; first-line approach recommended by most Canadian physiotherapists | Requires patient compliance; symptoms may return if activity is resumed too quickly |
| Physiotherapy & Exercise | Strengthens quadriceps and hip muscles to reduce plica irritation and improve knee tracking | Addresses underlying biomechanical issues; long-term symptom prevention; widely available across Canada | Requires consistent commitment over 6–12 weeks; progress may be gradual |
| NSAIDs (e.g., Ibuprofen, Naproxen) | Reduces inflammation and pain in the synovial plica tissue | Provides short-term relief; available over-the-counter at Canadian pharmacies | Not suitable for long-term use; potential gastrointestinal side effects; consult a physician before use |
| Corticosteroid Injection | Anti-inflammatory medication injected directly into the knee joint to reduce plica swelling | Rapid pain relief; useful when conservative measures have failed; performed in clinic settings across Canada | Limited to 2–3 injections; temporary relief only; small risk of infection or cartilage damage |
| Arthroscopic Surgery (Plica Resection) | Minimally invasive removal of the thickened or scarred plica tissue using a small camera and tools | Highly effective for refractory cases; quick recovery of 4–6 weeks; performed in Canadian hospitals and surgical centres | Reserved for cases unresponsive to 3–6 months of conservative treatment; carries standard surgical risks |
Inside your knee, there are thin bands of tissue called plicae (the singular form is plica). These are remnants of tissue from when you were developing in the womb. Normally, they fade as the fetus grows. However, in some people, these tissue folds remain in the knee joint after birth.
Most people never have a problem with their plicae. But when this tissue gets irritated, thickened, or inflamed, it causes knee plica syndrome. The condition can affect people of all ages, though it is more common in active individuals and athletes. For more information on joint health, visit Mayo Clinic’s guide to knee pain.
How Does a Plica Form?
During early fetal development, the knee joint starts as several separate compartments. These compartments are divided by thin walls of synovial tissue. As the fetus develops, these walls normally dissolve and merge into one large joint cavity.
If this process does not complete fully, small folds or bands of synovial tissue remain. There are up to four of these folds in the knee, found in different locations around the joint. The one most likely to cause problems sits along the inner side of the kneecap. When this tissue fold gets thick or tight, it rubs against the bones and cartilage inside the knee.
Common Causes of Knee Plica Syndrome
Knee plica syndrome does not always have one single cause. In most cases, it develops over time due to repeated stress on the knee. Understanding the triggers can help you protect your joints.
Overuse and Repetitive Motion
Repetitive activities like running, cycling, or climbing stairs are common triggers. These motions put repeated stress on the knee joint. Over time, this stress irritates the plica tissue and causes it to swell. Runners and cyclists in Canada are among those most commonly affected.
Injury or Trauma
A direct blow to the knee can also trigger this condition. For example, a fall or a sports collision can injure the synovial tissue. As a result, the plica becomes inflamed and painful. Even a minor knee injury can start this process if the tissue does not heal properly.
Inflammatory Joint Conditions
Certain inflammatory conditions, such as arthritis, can also irritate the plica. When the joint lining becomes inflamed for any reason, the plica can thicken and tighten. This leads to pain and restricted movement. If you have a known joint condition, you may be at higher risk for developing knee plica syndrome.
Symptoms of Knee Plica Syndrome
The symptoms of knee plica syndrome can feel similar to several other knee problems. This is one reason why it is frequently misdiagnosed. Knowing the specific signs can help you have a more informed conversation with your doctor.
Pain and Tenderness
Most people feel a dull, aching pain on the inner side of the kneecap. The pain often gets worse after sitting for a long time or after physical activity. You may also notice tenderness when you press on the inside of your knee. The discomfort tends to worsen when you climb stairs or squat.
Swelling Around the Knee
Swelling is another common symptom. The area around the kneecap may look puffy or feel warm to the touch. This swelling is caused by inflammation of the synovial tissue. In some cases, the swelling comes and goes depending on your activity level.
Clicking or Snapping Sensation
Many people with this condition feel or hear a clicking or snapping sound when they move their knee. This happens when the thickened plica snaps over the end of the thigh bone. The sound can be startling, but it is a key clue for diagnosis. However, many knee conditions can cause similar sounds, so this symptom alone is not enough to confirm the diagnosis.
Feeling of Weakness or Locking
Some people notice that their knee feels weak or unstable. Others describe a sensation of the knee “giving way” or locking up briefly. This can affect your ability to walk, exercise, or perform everyday tasks. These symptoms often lead people to visit a walk-in clinic or their family doctor.
How Is Knee Plica Syndrome Diagnosed?
Diagnosing knee plica syndrome can be challenging. Its symptoms closely resemble those of other knee conditions, such as a meniscus tear or patellofemoral syndrome. As a result, doctors often reach the diagnosis by ruling out other conditions first.
Physical Examination
Your doctor will begin with a physical exam. They will press along the inner edge of your kneecap to check for tenderness. They may also ask you to bend and straighten your knee while they feel for the snapping sensation. This hands-on assessment provides important clues about what is happening inside your joint.
Imaging Tests
X-rays cannot show soft tissue like the plica, but they can rule out bone problems. An MRI scan gives a much clearer picture of the soft tissues inside the knee. However, an MRI does not always show a thickened plica clearly. Your doctor may use imaging results alongside your symptoms to form a diagnosis. You can learn more about how joint imaging works at Healthline’s overview of plica syndrome.
Arthroscopy for Diagnosis
In some cases, your doctor may recommend arthroscopy to confirm the diagnosis. This is a minimally invasive procedure where a small camera is inserted into the knee joint. It allows the surgeon to see the plica directly. Arthroscopy can both diagnose and treat the condition in the same procedure.
Treatment Options for Knee Plica Syndrome
The good news is that most people with knee plica syndrome recover well with the right treatment. Treatment focuses on reducing inflammation and allowing the tissue to heal. Your doctor will usually start with the least invasive options first.
Rest and Activity Modification
The first step is to reduce the activities that are making your knee worse. This does not mean you need to stop moving entirely. Your doctor or physiotherapist will help you modify your activities so your knee can heal. Low-impact activities like swimming can keep you active without stressing the joint.
Ice and Compression
Applying ice to the knee for 15 to 20 minutes several times a day helps reduce swelling. Wrapping the knee with an elastic bandage or wearing a knee sleeve also provides support. These simple steps can make a noticeable difference in your comfort level. In addition, elevating your leg when resting can help reduce swelling further.
Anti-Inflammatory Medication
Your doctor may recommend over-the-counter anti-inflammatory medications such as ibuprofen. These help reduce both pain and swelling in the joint. Always follow the recommended dosage and speak with your pharmacist if you have other health conditions. Provincial drug benefit programmes in Canada may cover prescription anti-inflammatory medications if needed.
Physiotherapy and Strengthening Exercises
Strengthening the muscles around the knee is one of the most effective long-term treatments. A physiotherapist can design a programme tailored to your needs. Stronger quadriceps and hip muscles take pressure off the knee joint. Many Canadians access physiotherapy through their provincial health plan or private insurance.
Corticosteroid Injections
If rest and medication do not bring enough relief, your doctor may suggest a corticosteroid injection directly into the knee joint. Research suggests these injections help about half of patients with this condition. The injection reduces inflammation quickly and can allow you to participate more fully in physiotherapy. Your family doctor or a specialist can perform this procedure.
Surgery
If conservative treatment does not improve symptoms after about three months, surgery may be recommended. The most common procedure is arthroscopic surgery, where the surgeon removes or releases the thickened plica. This is a minimally invasive procedure with a relatively quick recovery time. Most patients return to normal activity within a few weeks after surgery. For further reading on joint procedures, see Health Canada’s information on the Canadian health care system.
When to See a Doctor
You should see your family doctor or visit a walk-in clinic if your knee pain has lasted more than two weeks. You should also seek care if your knee is significantly swollen, locks up, or gives way unexpectedly. Do not wait to get help if your pain is interfering with your daily life or sleep.
Your family doctor can assess your knee, order imaging if needed, and refer you to an orthopaedic specialist or physiotherapist. If you do not have a family doctor, a walk-in clinic is a good first step. Early diagnosis leads to better outcomes and a faster recovery. Always consult a qualified healthcare professional before starting any new treatment or exercise programme for knee pain.
Frequently Asked Questions About Knee Plica Syndrome
What does knee plica syndrome feel like?
Knee plica syndrome typically causes a dull ache on the inner side of the kneecap, along with swelling and tenderness. Many people also notice a clicking or snapping sensation when bending the knee. In some cases, the knee may feel weak or briefly lock up during movement.
Can knee plica syndrome heal on its own?
Mild cases of knee plica syndrome can sometimes improve with rest and reduced activity. However, most people need a structured treatment plan that includes physiotherapy and anti-inflammatory medication. Without treatment, the irritation can become chronic and worsen over time.
How long does recovery from knee plica syndrome take?
Recovery time varies depending on the severity of the condition and the treatment used. With conservative treatment, many patients see improvement within six to twelve weeks. If surgery is needed, most people return to full activity within four to six weeks after the procedure.
Is knee plica syndrome the same as a meniscus tear?
No, knee plica syndrome and a meniscus tear are two different conditions, though their symptoms can be very similar. A meniscus tear involves damage to the cartilage cushions in the knee, while knee plica syndrome involves irritation of a tissue fold in the joint lining. A doctor will use a physical exam and imaging to tell the difference.
Who is most at risk for knee plica syndrome?
Knee plica syndrome is most common in athletes and physically active people who do repetitive knee movements, such as runners and cyclists. However, it can also occur after a direct knee injury or alongside inflammatory joint conditions like arthritis. People of all ages can develop this condition.
Can physiotherapy help knee plica syndrome?
According to Mayo Clinic’s guide to knee pain causes and diagnosis, this information is supported by current medical research.
For more information, read our guide on differences between MRI and CT scans for knee imaging.
Yes, physiotherapy is one of the most effective treatments for knee plica syndrome. A physiotherapist will design a programme to strengthen the muscles around the knee and reduce stress on the irritated tissue. Many Canadians access physiotherapy through their provincial health plan or extended health benefits.
Key Takeaways
- Knee plica syndrome occurs when a fold of tissue inside the knee becomes irritated and inflamed.
- It is caused by overuse, injury, or inflammatory joint conditions.
- Symptoms include inner knee pain, swelling, clicking, and a feeling of weakness or locking.
- Diagnosis involves ruling out other knee conditions through physical exam, imaging, and sometimes arthroscopy.
- Most cases improve with rest, ice, anti-inflammatory medication, and physiotherapy.
- Corticosteroid injections help about half of patients who do not respond to basic treatment.
- Surgery is an effective option if conservative treatment does not work after three months.
- See your family doctor or visit a walk-in clinic if knee pain persists or affects your daily life.
- Always speak with a healthcare professional before starting a new treatment plan.
Frequently Asked Questions
What is knee plica syndrome?
Knee plica syndrome is a condition where the plica — a fold of synovial tissue inside the knee joint — becomes irritated and inflamed. This tissue is a remnant from fetal development. When aggravated by overuse or injury, it thickens and causes pain, swelling, and restricted knee movement.
What are the symptoms of knee plica syndrome?
Common symptoms include aching pain along the inner knee, clicking or snapping sensations, swelling, and stiffness — especially after sitting for long periods or climbing stairs. Symptoms often worsen with repetitive activities like running or cycling and may mimic other knee conditions, making accurate diagnosis important.
How is knee plica syndrome treated in Canada?
Treatment typically begins conservatively with rest, ice, anti-inflammatory medications like ibuprofen, and physiotherapy to strengthen surrounding muscles. Most Canadians recover without surgery. If symptoms persist beyond three to six months, arthroscopic surgery to remove or release the irritated plica tissue is a safe, effective option.
Can knee plica syndrome be prevented?
Prevention involves gradually increasing exercise intensity, maintaining strong quadriceps and hamstring muscles, and using proper technique during physical activity. Wearing supportive footwear, warming up thoroughly before workouts, and avoiding sudden increases in training volume can significantly reduce the risk of plica irritation and inflammation.
When should I see a doctor for knee pain that might be knee plica syndrome?
See a doctor if knee pain persists longer than two weeks, worsens with activity, or is accompanied by noticeable swelling, locking, or a clicking sensation. Early assessment by a Canadian physician or physiotherapist helps rule out other conditions like meniscus tears and ensures appropriate, timely treatment.
About the Author
Dr. James Okafor, MD, PhDDr. James Okafor holds an MD and PhD in Neurological Sciences from McGill University. With 12 years of experience in clinical neurology and mental health research, he has contributed to landmark studies on depression, anxiety, and cognitive health. Dr. Okafor is a Fellow of the Royal College of Physicians and Surgeons of Canada and serves on the editorial board of two peer-reviewed journals.
View all articles →