Gum Disease: Gingivitis & Periodontitis Guide Canada
Share
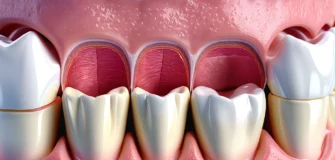
Gum disease is one of the most common oral health problems in Canada, yet millions of Canadians don’t realize they have it. It begins silently, often with little or no pain, and can gradually destroy the tissue and bone that hold your teeth in place. Recognizing the early warning signs can save your smile and protect your long-term health.
What Is Gum Disease and Why Should Canadians Be Concerned?
Also known as periodontal disease, this condition ranges from mild gingivitis and periodontitis in its advanced form. Understanding the difference between these stages is critical because early detection allows for simpler, more effective treatment. In this guide, we break down the causes, symptoms, risk factors, and prevention strategies every Canadian should know to keep their gums healthy.
What Is Gum Disease?
| Stage / Type | Key Characteristics | Common Symptoms | Recommended Management |
|---|---|---|---|
| Gingivitis (Early Gum Disease) | Inflammation limited to the gums; no bone or tissue loss; fully reversible | Red, swollen gums; bleeding when brushing or flossing; mild bad breath | Professional dental cleaning; improved brushing and flossing; antimicrobial mouthrinse |
| Mild Periodontitis | Infection spreads below the gumline; early bone loss begins; pocket depths 3–4 mm | Persistent bad breath; gums beginning to pull away from teeth; slight tooth sensitivity | Scaling and root planing (deep cleaning); more frequent dental visits (every 3–4 months) |
| Moderate Periodontitis | Significant bone and connective tissue destruction; pocket depths 5–6 mm | Noticeable gum recession; increased tooth sensitivity; loose teeth; pus between gums and teeth | Scaling and root planing; possible antibiotic therapy; referral to a periodontist |
| Severe Periodontitis | Advanced bone loss; deep pockets over 6 mm; high risk of tooth loss | Significant tooth mobility; severe pain when chewing; abscesses; major gum recession | Periodontal surgery (flap surgery or bone grafting); tooth extraction if necessary; ongoing specialist care |
| Necrotizing Periodontal Disease | Rapid tissue death affecting gums, ligaments, and bone; most severe form; rare but serious | Severe pain; grey film on gums; punched-out ulcers between teeth; fever; strong bad breath | Immediate dental or medical attention; debridement; antibiotics; treatment of underlying conditions (e.g., HIV, malnutrition) |
Gum disease is a bacterial infection of the tissues that surround and support your teeth. Dentists also call it periodontal disease. It ranges from mild inflammation of the gums to serious damage to the bone and soft tissue.
There are two main stages. The first is gingivitis, which affects only the gum tissue. The second, more serious stage is periodontitis (also called periodontal disease or parodontosis). If gingivitis goes untreated, it can progress into periodontitis and lead to tooth loss.
Gingivitis: The Early Stage
Gingivitis causes gums to become red, swollen, and easy to bleed — especially when you brush or floss. However, gingivitis is usually painless. Because of this, many Canadians ignore the early warning signs and don’t seek treatment.
The good news is that gingivitis is reversible with proper dental care. Catching it early makes a big difference. For more information, visit Health Canada’s oral health resources.
Periodontitis: The Advanced Stage
When gingivitis is left untreated, it advances to periodontitis. The gums pull away from the teeth, creating deep pockets where bacteria thrive. These bacteria destroy the bone and connective tissue that hold teeth in place.
As a result, gums recede and teeth may appear longer than normal. Teeth can become loose, shift position, or eventually fall out. In some cases, a dentist must remove them entirely.
What Causes Gum Disease?
Gum disease starts with bacteria. Your mouth naturally contains bacteria, and they mix with mucus and food particles to form a sticky, colourless film on your teeth called plaque. Regular brushing and flossing remove plaque before it can cause harm.
When plaque stays on the teeth too long, it hardens into a rough deposit called tartar (also known as calculus). Tartar irritates the gums and can only be removed by a dental professional. The bacteria in plaque feed on sugars from food and drinks, producing toxins that inflame and damage gum tissue.
Common Risk Factors
Several factors raise your risk of developing gum disease. Some you can control, and some you cannot. Knowing your risk factors helps you take better care of your oral health.
- Tobacco use: Smoking or chewing tobacco is one of the biggest risk factors. Tobacco weakens your immune system, slows healing, and makes serious gum problems much more likely — even after a tooth extraction.
- Genetics: If gum disease runs in your family, your risk is higher — even with excellent oral hygiene. A family history of periodontitis is a strong predictor.
- Hormonal changes: Women going through puberty, pregnancy, or menopause experience hormonal shifts that make gums more sensitive and vulnerable to infection.
- Certain medications: Some drugs reduce saliva flow or cause gum tissue to grow abnormally. These include phenytoin (an anti-seizure medication), calcium channel blockers (used for high blood pressure), cyclosporine (an immunosuppressant used after organ transplants), oral contraceptives, and some antidepressants.
- Weakened immune system: Conditions such as type 2 diabetes, HIV/AIDS, and leukemia make it harder for your body to fight infection, including gum infections.
- Poor diet: A diet low in vitamins and minerals weakens the immune system. Diets high in sugar and refined carbohydrates — such as white bread, pasta, and cereals — also feed the bacteria that cause plaque to grow.
- Chronic stress: Stress weakens the immune system and raises your risk of infections, including gum disease.
Recognising the Symptoms of Gum Disease
Many Canadians live with gum disease without realising it. The early stages are often painless, which is why regular dental checkups are so important. Knowing the symptoms helps you act before things get worse.
Early Symptoms (Gingivitis)
- Red, swollen, or tender gums
- Gums that bleed easily when you brush or floss
- Gums that look slightly puffy along the gum line
These symptoms may seem minor. However, they are your body’s way of signalling that bacteria are causing damage. Don’t ignore them.
Advanced Symptoms (Periodontitis)
As gum disease progresses to periodontitis, symptoms become harder to ignore. At this stage, damage to the bone and tissue is already underway.
- Gums that pull away from the teeth (receding gums)
- Persistent bad breath that doesn’t go away with brushing
- Pus between the teeth and gums
- Teeth that feel loose or shift when you bite
- A change in how your teeth fit together when you chew
- Teeth that look longer because the gums have receded
According to the Mayo Clinic’s guide to periodontitis, advanced gum disease can also be linked to serious systemic health issues, including heart disease and diabetes.
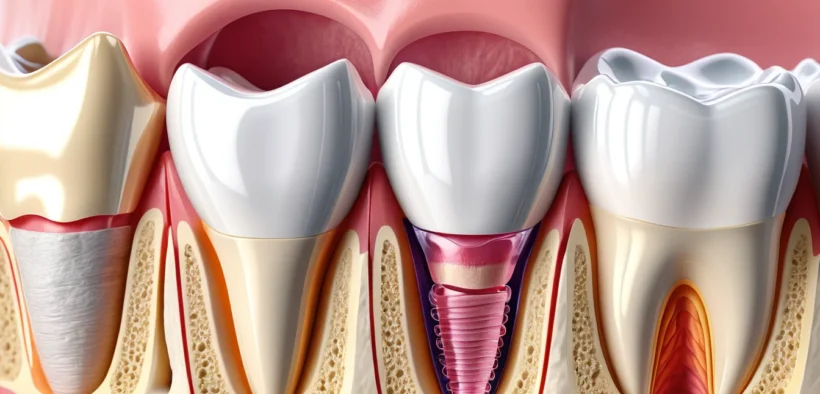
How Gum Disease Develops: The Biological Process
Understanding how gum disease progresses helps explain why early treatment matters so much. The process unfolds gradually over months or even years.
It begins when bacteria collect on the teeth and gums, forming plaque. The bacteria produce acids and toxins that irritate the gum tissue, causing redness and swelling. This is gingivitis — the earliest and most treatable form of gum disease.
If plaque is not removed, it mineralises into tartar. Tartar sits along and below the gum line, causing constant irritation. The gums begin to separate from the teeth, forming pockets. Bacteria move deeper into these pockets, attacking the bone and connective tissue below the gum line.
Furthermore, the immune system responds by releasing substances that, over time, actually contribute to more tissue and bone breakdown. This is why periodontitis can worsen even when it doesn’t feel painful. The World Health Organization’s oral health fact sheet notes that severe periodontal disease is among the most prevalent non-communicable diseases globally.
Prevention and Daily Oral Care
The best way to prevent gum disease is through consistent daily habits. Good oral hygiene removes plaque before it hardens into tartar and causes damage.
Daily Habits That Protect Your Gums
- Brush twice a day: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, making sure to clean along the gum line.
- Floss once a day: Flossing removes plaque and food particles from between the teeth where your toothbrush can’t reach.
- Rinse with an antiseptic mouthwash: This helps reduce bacteria in the mouth and freshens breath.
- Eat a balanced diet: A diet rich in vegetables, fibre, and vitamins supports a healthy immune system and healthy gums.
- Limit sugary foods and drinks: Sugar feeds the bacteria that produce plaque. Cutting back reduces your risk significantly.
- Quit smoking: Giving up tobacco is one of the most powerful steps you can take for your gum health. Talk to your family doctor about cessation programmes covered under your provincial health plan.
Regular Dental Visits
Visiting your dentist or dental hygienist every six months is essential. Professional cleanings remove tartar that brushing and flossing cannot. Your dental team can also spot early signs of gum disease before they become serious problems.
Many provincial health plans in Canada include some dental benefits, particularly for children and lower-income residents. The federal Canadian Dental Care Plan also now helps eligible Canadians access dental care. Check with your province or territory to understand what is covered for you.
When to See a Doctor or Dentist
If you notice any signs of gum disease, don’t wait. Early treatment is far simpler and more effective than treating advanced periodontitis.
See your family doctor or dentist if you experience any of the following:
- Gums that bleed regularly when you brush or floss
- Persistent bad breath that doesn’t improve
- Gums that look swollen, red, or have pulled away from your teeth
- Loose or shifting teeth
- Pain when chewing
If you don’t have a regular dentist, a walk-in dental clinic can assess your gum health and refer you to a periodontist (a gum specialist) if needed. Don’t let cost be a barrier — ask about payment plans or provincial assistance programmes.
Always speak with a qualified dental or medical professional before starting any treatment for gum disease. This article is for informational purposes only and does not replace personalised medical advice.
Frequently Asked Questions About Gum Disease
Can gum disease be reversed?
Gingivitis, the earliest stage of gum disease, can be fully reversed with proper brushing, flossing, and professional dental cleanings. However, once gum disease advances to periodontitis, the damage to bone and tissue cannot be fully reversed — only managed. Early treatment gives you the best outcome.
Is gum disease contagious?
The bacteria that cause gum disease can be passed between people through saliva — for example, through kissing or sharing utensils. However, most people’s immune systems prevent these bacteria from causing gum disease on their own. Good oral hygiene remains your strongest defence.
What does gum disease look like?
In the early stages, gum disease causes gums to appear red, swollen, and slightly puffy along the gum line. As it progresses, gums may recede (pull away from the teeth), making teeth look longer. You may also notice bleeding when brushing, pus near the gums, or persistent bad breath.
How is gum disease treated by a dentist?
A dentist or dental hygienist treats early gum disease with a thorough professional cleaning to remove plaque and tartar. For more advanced gum disease, a procedure called scaling and root planing cleans deep below the gum line. In severe cases, a periodontist may recommend surgical treatment to restore damaged tissue and bone.
Can gum disease affect my overall health?
Yes. Research links gum disease to several systemic health conditions, including heart disease, diabetes, and respiratory problems. The bacteria from infected gums can enter the bloodstream and affect other parts of the body. Managing gum disease is an important part of maintaining your overall health.
Does the Canadian Dental Care Plan cover gum disease treatment?
According to Health Canada’s oral health resources, this information is supported by current medical research.
For more information, read our guide on myths about infections and overall health every Canadian should know.
The federal Canadian Dental Care Plan provides coverage for eligible Canadians who meet certain income criteria and do not have private dental insurance. Coverage may include cleanings, scaling, and other treatments related to gum disease. Visit your provincial health authority’s website or speak with your dentist’s office to find out if you qualify.
Key Takeaways
- Gum disease is a bacterial infection that ranges from mild gingivitis to serious periodontitis.
- Gingivitis is often painless, which is why many Canadians miss the early warning signs.
- Plaque and tartar buildup are the main causes, but tobacco use, genetics, hormonal changes, and certain medications also raise your risk.
- Symptoms include red or swollen gums, bleeding, bad breath, receding gums, and loose teeth.
- Brushing twice daily, flossing, eating a balanced diet high in fibre, and quitting smoking are the best preventive steps.
- See your family doctor, dentist, or a walk-in dental clinic if you notice any symptoms — early treatment works best.
- Some dental treatments for gum disease may be covered under your provincial health plan or the Canadian Dental Care Plan.
Frequently Asked Questions
What is gum disease and what causes it?
Gum disease is a bacterial infection of the tissues supporting your teeth. It begins when plaque — a sticky film of bacteria — builds up along the gumline. If not removed through brushing and flossing, plaque hardens into tartar, triggering inflammation. Risk factors include smoking, diabetes, poor oral hygiene, and certain medications.
What are the early warning signs of gum disease?
Early gum disease symptoms include red, swollen, or tender gums that bleed easily during brushing or flossing. Bad breath that won’t go away, gums pulling away from teeth, and increased tooth sensitivity are also common signs. Many Canadians don’t notice pain in early stages, making regular dental checkups essential.
How is gum disease treated in Canada?
Gum disease treatment depends on severity. Gingivitis is typically reversed with professional dental cleaning and improved oral hygiene at home. Advanced periodontitis may require scaling and root planing (deep cleaning), antibiotics, or surgical procedures. Most provincial dental plans cover basic periodontal treatments, though coverage varies significantly by province.
Can gum disease be prevented with daily brushing and flossing?
Yes, consistent oral hygiene is your best defence against gum disease. Brush twice daily with fluoride toothpaste, floss once daily, and rinse with an antibacterial mouthwash. Combined with professional dental cleanings every six months, these habits remove plaque before it causes gum inflammation and significantly reduce your risk.
When should you see a dentist about gum problems?
See a dentist promptly if your gums bleed regularly, appear swollen or receding, or if you notice persistent bad breath or loose teeth. Don’t wait for pain — gum disease is often painless until advanced. Canadians should schedule dental checkups at least twice yearly for early detection and treatment.
About the Author
Dr. Sarah Mitchell, MDDr. Sarah Mitchell is a board-certified family physician with over 15 years of clinical experience. She completed her MD at the University of Toronto and her residency at Toronto General Hospital. Dr. Mitchell specializes in preventive medicine and chronic disease management. She is a member of the College of Family Physicians of Canada (CFPC) and has published over 30 peer-reviewed articles on preventive health care.
View all articles →