Kneecap Fracture: Causes, Treatment & Recovery Canada
Share
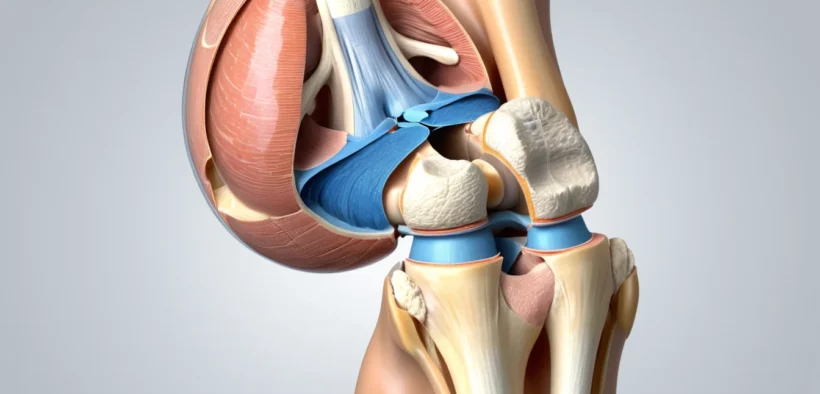
A kneecap fracture is a painful and often debilitating knee injury that can affect anyone in Canada — from athletes and active adults to seniors and children. The kneecap, medically known as the patella, sits at the front of your knee and plays a critical role in helping you walk, climb stairs, and bend your leg. When this small but essential bone breaks, everyday movement becomes extremely difficult.
How Is a Kneecap Fracture Diagnosed and Treated in Canada?
Whether caused by a fall, a sports collision, or a direct blow to the knee, a kneecap dislocation or fracture requires prompt medical attention. This guide explains the key differences between these injuries, how Canadian doctors diagnose and treat them, and what your rehabilitation journey will look like so you can get back on your feet with confidence.
What Is the Kneecap and Why Does It Matter?
| Fracture Type | Characteristics | Common Causes | Typical Management |
|---|---|---|---|
| Transverse Fracture | Horizontal break across the middle of the patella; most common type, accounting for roughly 50–80% of cases | Direct blow to the knee or sudden forceful contraction of the quadriceps muscle | Surgery (tension band wiring or screws) if displaced; cast or brace for 4–6 weeks if non-displaced |
| Comminuted (Stellate) Fracture | Patella shatters into three or more fragments; often results in significant joint surface damage | High-impact trauma such as a motor vehicle collision or a hard fall onto a hard surface | Surgical fixation if possible; partial or total patellectomy may be required for severely fragmented cases |
| Vertical Fracture | Longitudinal split along the length of the patella; extensor mechanism is typically preserved | Direct lateral impact or indirect twisting force on the knee joint | Usually managed non-operatively with a cylinder cast or hinged knee brace for 4–6 weeks |
| Osteochondral Fracture | Fracture involving the cartilage and underlying bone; often associated with patellar dislocation | Acute patellar dislocation, common in adolescents and young active adults | Arthroscopic or open surgery to remove or reattach the fragment; rehabilitation to restore stability |
| Avulsion Fracture | Small fragment of bone pulled away at the attachment site of a tendon or ligament | Sudden forceful muscle contraction, such as a rapid deceleration or jumping movement | Conservative management with immobilization for minor avulsions; surgical reattachment if the fragment is large or displaced |
The kneecap is a small, triangular bone that sits in front of the knee joint. It protects the joint and helps your leg muscles work efficiently when you move. Without it functioning properly, bending and straightening your knee becomes very hard.
The kneecap sits inside a groove at the end of the thigh bone. Strong tendons and ligaments hold it in place. Any strong impact or awkward movement can disrupt this structure and lead to a kneecap fracture or dislocation.
Understanding the difference between a fracture and a dislocation is important. A fracture means the bone has cracked or broken. A dislocation means the kneecap has slipped out of its normal groove — but the bone itself may not be broken.
Kneecap Dislocation: Causes and Symptoms
A kneecap dislocation happens when the patella shifts out of its normal position, usually moving to the outside of the knee. This can happen to people with perfectly healthy knees or to those who have had previous knee problems or certain congenital conditions.
Common causes include a sudden twisting movement, a direct blow to the knee, or landing awkwardly after a jump. Athletes who play contact sports or sports that involve rapid direction changes — like hockey, soccer, or basketball — face a higher risk.
Recognising the Symptoms of a Dislocated Kneecap
The symptoms of a kneecap dislocation are usually hard to miss. You will likely feel sudden, sharp pain in the front of the knee. Bending the leg often makes the pain much worse.
When you look at the knee, you may notice the kneecap sitting in the wrong position. There may also be a visible hollow or depression where the kneecap normally sits. Some people experience swelling inside the joint, known as joint effusion. This swelling can range from mild to quite significant.
Kneecap Fracture: Causes and Symptoms
A kneecap fracture can happen in two main ways. A direct fracture results from a hard blow to the knee — for example, falling on a hard surface or a car dashboard impact during a collision. An indirect fracture happens when the muscles pull so forcefully that the bone cracks, often during a sudden, forceful bending of the leg.
Indirect fractures tend to happen during high-intensity physical activity. For example, a sudden lunge or an explosive jump can generate enough force to break the kneecap from the inside out.
Recognising the Symptoms of a Kneecap Fracture
A kneecap fracture causes significant pain, swelling, and tenderness around the front of the knee. You may notice bruising quite quickly after the injury. The knee joint may fill with blood, a condition called haemarthrosis, which causes warmth and tightness around the joint.
Walking becomes very difficult or impossible. When a doctor gently feels around the knee, they may detect bone fragments that have shifted out of place. This is a clear sign that the fracture has caused displacement, which usually means more intensive treatment is needed. You can learn more about general knee injuries from Mayo Clinic’s knee pain resource.
Treatment Options for Kneecap Injuries
Treatment depends on the type and severity of the injury. A healthcare provider — whether your family doctor, an emergency room physician, or an orthopaedic specialist — will assess the injury with a physical exam and imaging tests like an X-ray or MRI.
Treating a Kneecap Dislocation
For a dislocated kneecap, the first step is to gently move the kneecap back into its groove. A doctor performs this manoeuvre carefully, often with some pain relief or sedation. This procedure is called a reduction.
After the reduction, many cases are managed with a compression bandage or a knee brace to keep the joint stable. In most cases, this conservative approach works well. However, if the dislocation is severe, recurrent, or involves damage to other structures, surgery may be necessary. In rare cases, the kneecap may need to be surgically removed — a procedure called a patellectomy.
Treating a Kneecap Fracture
Treatment for a kneecap fracture also varies based on severity. A minor, non-displaced fracture — where the bone pieces stay in place — may heal with rest, a compression bandage, and a plaster splint or cast. Most people can begin walking again within about three weeks, depending on how well healing progresses.
A displaced fracture — where bone fragments have moved apart — usually requires surgery. Surgeons use wires, screws, or pins to hold the fragments together while the bone heals. In very severe cases where the bone is shattered, a partial or full patellectomy may be performed. According to Health Canada, musculoskeletal injuries are among the most common reasons Canadians visit orthopaedic specialists and walk-in clinics each year.
Rehabilitation After a Kneecap Injury
Rehabilitation is an essential part of recovery from both a kneecap fracture and a dislocation. In Canada, a physiotherapist — sometimes called a physio — will guide your recovery programme. Your family doctor or orthopaedic surgeon will refer you to physiotherapy as part of your treatment plan.
Rehabilitation begins even during the immobilisation period. The early goals are to reduce inflammation, support healthy lymphatic drainage, and maintain muscle tone so the leg does not weaken significantly while healing.
Stages of Knee Rehabilitation
Once the immobilisation phase ends, rehabilitation moves into more active stages. A physiotherapist will begin with passive exercises, often performed in water. Hydrotherapy reduces the load on the joint and allows gentle movement without pain.
As strength and mobility return, the programme shifts to active exercises. These include gradually rebuilding the range of flexion in the knee, strengthening the surrounding muscles, and relearning how to walk properly. Initially, patients use crutches for support. They then transition to a cane before eventually walking without any assistance.
Returning to a normal standing position — called orthostatism — is also practised carefully. The goal is full joint mobility, strong supporting muscles, and a confident, pain-free walking pattern. The entire recovery process can take several weeks to several months, depending on the severity of the original injury and how consistently the patient follows their rehabilitation programme. For general guidance on bone health and recovery, Healthline’s bone health section offers reliable information.
Prevention: Protecting Your Knees
Preventing kneecap injuries is possible with the right habits and awareness. This is especially important for high-performance athletes, older adults, and children — all of whom have a higher sensitivity to knee injuries.
Athletes should always warm up properly before training or competition. Sudden, jerky movements at the knee — especially twisting or pivoting — put the kneecap at risk. Using proper technique in sports and wearing appropriate protective equipment greatly reduces this risk.
Older Canadians should focus on balance training and lower body strengthening exercises to reduce the risk of falls. Children should be encouraged to move safely, especially during sports and play. Wearing proper footwear and using protective knee pads during high-risk activities can also make a real difference.
Maintaining a healthy weight helps reduce the load on the knee joint during everyday activities. Regular low-impact exercise — like swimming, cycling, or walking — keeps the muscles around the knee strong and supportive.
When to See a Doctor
If you experience sudden knee pain, visible swelling, or notice your kneecap sitting in an unusual position, seek medical attention right away. Do not try to push the kneecap back into place yourself — this can cause further damage.
In Canada, you have several options depending on your situation. For a serious injury with severe pain or an obvious deformity, go directly to your nearest emergency room. For less urgent but still concerning symptoms — such as ongoing knee pain, swelling that does not improve, or a history of kneecap problems — visit your family doctor or a walk-in clinic. Your doctor can arrange X-rays, refer you to an orthopaedic specialist, and connect you with physiotherapy services covered under your provincial health plan.
Most provincial health plans in Canada cover orthopaedic consultations and physiotherapy referrals when arranged through your family doctor. Always ask your provider about what is covered in your province so you can access the care you need without unexpected costs.
How long does a kneecap fracture take to heal?
A minor kneecap fracture that does not require surgery can take about six to eight weeks to heal. More serious displaced fractures that need surgical repair may require three to six months of healing and rehabilitation before you return to full activity. Your physiotherapist and orthopaedic surgeon will guide you through each stage of recovery.
Can you walk with a fractured kneecap?
Walking with a kneecap fracture is usually very painful and difficult, especially right after the injury. In minor cases with no displacement, some weight-bearing may be possible with a brace or splint, but most people need crutches initially. Your doctor will advise when it is safe to start putting weight on the leg again.
What is the difference between a kneecap fracture and a kneecap dislocation?
A kneecap fracture means the bone has actually cracked or broken into pieces. A kneecap dislocation means the patella has slipped out of its normal groove at the front of the knee, but the bone may not be broken. Both conditions cause significant pain and require medical treatment, though the treatment approaches differ.
Is surgery always needed for a kneecap fracture?
Not all kneecap fractures require surgery. Non-displaced fractures — where the bone pieces remain in their correct position — are often treated with a cast or splint and rest. However, displaced fractures, where the pieces have shifted apart, usually do require surgery to realign and secure the bone fragments so they heal correctly.
What does kneecap rehabilitation involve in Canada?
Rehabilitation for a kneecap fracture or dislocation in Canada typically involves a physiotherapy programme prescribed by your family doctor or orthopaedic surgeon. Treatment includes reducing swelling, gentle water-based exercises, progressive strengthening, and relearning to walk with and then without assistive devices. Many provincial health plans cover physiotherapy when referred through your family doctor.
Who is most at risk for kneecap injuries?
According to Mayo Clinic’s guide to patella and knee conditions, this information is supported by current medical research.
For more information, read our guide on MRI vs CT scan for diagnosing knee injuries.
Athletes who play high-impact or contact sports — such as hockey, soccer, and basketball — face a higher risk of kneecap dislocation and fracture. Older adults are at greater risk due to reduced bone density and balance, while children can be vulnerable because their bones are still developing. Taking preventive steps like proper warm-ups, balance training, and protective equipment significantly lowers the risk for all age groups.
Key Takeaways
- Kneecap fractures and dislocations are serious knee injuries that require prompt medical attention.
- Symptoms include sudden pain, swelling, and difficulty bending or walking.
- Treatment ranges from compression bandages and rest to surgery, depending on severity.
- Rehabilitation with a physiotherapist is essential for a full recovery and should begin early.
- Recovery involves reducing inflammation, rebuilding strength, and gradually relearning to walk.
- Prevention through proper warm-up, technique, and strength training protects the knee long-term.
- If you are concerned about a knee injury, visit your family doctor, a walk-in clinic, or the emergency room — and always consult a healthcare professional before starting any rehabilitation programme on your own.
Frequently Asked Questions
What is a kneecap fracture?
A kneecap fracture (patella fracture) is a break in the small bone covering the front of the knee joint. It can occur as a hairline crack or a complete break into multiple pieces. Most kneecap fractures result from direct impact, a fall, or sudden muscle contraction, and require prompt medical attention.
What are the symptoms of a kneecap fracture?
Common symptoms include sudden, severe knee pain, visible swelling and bruising, inability to straighten the leg or walk, and tenderness directly over the kneecap. In severe cases, you may feel a gap in the bone. Symptoms of a kneecap dislocation also include the kneecap visibly shifting out of position.
How is a kneecap fracture treated in Canada?
Treatment depends on fracture severity. Non-displaced fractures are typically managed with a cast or knee brace for 4–6 weeks. Displaced or comminuted fractures usually require surgery to realign and stabilize bone fragments using screws or wires. Physiotherapy is an essential part of recovery at Canadian orthopaedic clinics.
When should you see a doctor for a knee injury or dislocation?
Seek immediate medical care if you experience sudden severe knee pain, visible deformity, significant swelling, or inability to bear weight or straighten your leg. These are signs of a potential fracture or dislocation. In Canada, visit your nearest emergency department or urgent care centre without delay.
Can you prevent kneecap injuries during sports or exercise?
You can reduce risk by wearing appropriate protective knee pads during contact sports, strengthening quadriceps and hamstring muscles, practicing proper landing techniques, and wearing supportive footwear. Warming up thoroughly before exercise and avoiding sudden increases in training intensity also significantly lowers the likelihood of kneecap fractures and dislocations.
About the Author
Dr. Linda Chen, RD, PhDDr. Linda Chen is a registered dietitian and PhD in Nutritional Sciences from the University of British Columbia. With expertise in clinical nutrition, sports dietetics, and gut health, she has worked with leading Canadian hospitals and sports organizations. Dr. Chen is a member of Dietitians of Canada and regularly contributes to national nutrition policy discussions.
View all articles →