Placenta Previa: Causes, Symptoms & Treatment Canada
Share
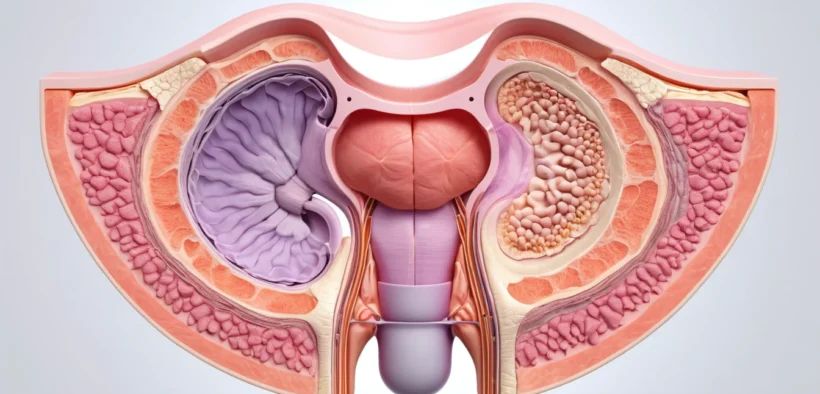
Placenta previa is a pregnancy complication in which the placenta grows too low in the uterus, partially or fully covering the cervix. It affects fewer than 1 in 100 pregnancies in Canada, but it demands careful monitoring and timely medical care to protect both mother and baby.
What Is Placenta Previa and How Does It Affect Pregnancy?
Understanding the causes, placenta previa symptoms, and available treatment options can help Canadian mothers and families feel more prepared for what lies ahead. If you notice any unusual bleeding during pregnancy or have concerns about a low-lying placenta, speak with your family doctor, obstetrician, or midwife right away.
What Is Placenta Previa?
| Type | Characteristics | Symptoms & Risks | Management Approach |
|---|---|---|---|
| Complete (Total) Placenta Previa | Placenta fully covers the internal cervical os | Heavy, painless vaginal bleeding; highest risk of hemorrhage and preterm birth | Planned caesarean section at 36–37 weeks; hospitalization often required after 34 weeks |
| Partial Placenta Previa | Placenta partially covers the internal cervical os | Moderate to heavy bleeding; significant risk of complications during labour | Caesarean section typically required; close monitoring with serial ultrasounds |
| Marginal Placenta Previa | Placental edge reaches but does not cover the cervical os | Mild to moderate bleeding; may resolve as uterus grows | Vaginal delivery may be possible if placenta migrates; regular ultrasound monitoring every 4 weeks |
| Low-Lying Placenta | Placenta implants within 2 cm of the cervical os but does not cover it | Spotting or light bleeding; often asymptomatic in early pregnancy | Follow-up ultrasound at 32–36 weeks; vaginal delivery possible if placenta moves sufficiently |
| Placenta Previa with Accreta | Placenta abnormally adheres to the uterine wall alongside previa | Severe hemorrhage risk; associated with prior uterine surgery or C-section scarring | Delivery at a tertiary care centre; caesarean hysterectomy may be required; multidisciplinary team essential |
The placenta is an organ that forms on the inner wall of the uterus shortly after conception. It carries oxygen and nutrients from the mother to the baby, and removes the baby’s waste products.
In most pregnancies, the placenta attaches to the upper part of the uterus, well above the cervix. However, in fewer than 1% of births, the placenta forms near the bottom of the uterus and covers the cervix either partially or completely. This condition is called placenta previa.
When the placenta blocks the cervix, it can cause serious bleeding during pregnancy and delivery. This is why placenta previa is considered a significant pregnancy complication that requires close medical supervision. For more background on placenta previa, visit Mayo Clinic’s overview of placenta previa.
Causes and Risk Factors of Placenta Previa
The exact cause of placenta previa is not fully understood. However, several risk factors can increase a woman’s chances of developing this condition.
Smoking During Pregnancy
Smoking reduces the amount of oxygen that reaches the baby. As a result, the placenta may grow larger than normal, making it more likely to extend into the lower part of the uterus. Smoking is associated with about 1 in 4 cases of placenta previa.
Previous Uterine Procedures
A history of procedures that affect the lining of the uterus can increase risk. These include dilation and curettage (D&C), which may be performed after a miscarriage or a therapeutic abortion. These procedures can affect how and where the placenta attaches in future pregnancies.
Previous Caesarean Sections
Women who have had a caesarean section before face a higher risk. Among women with one previous caesarean, about 4 in 100 will develop placenta previa in a later pregnancy. Among those with four or more caesarean sections, the risk rises to about 10 in 100.
Multiple Previous Pregnancies
Placenta previa occurs in about 1 in 1,500 first-time mothers. However, for women who have had five or more pregnancies, the risk rises significantly to about 1 in 20.
Maternal Age
Older mothers face a higher risk. Among pregnant women under 19 years of age, only about 1 in 1,500 develops placenta previa. Among women over 35, the rate rises to about 1 in 100.
Other Risk Factors
- Cocaine use during pregnancy
- A previous diagnosis of placenta previa or a low-lying placenta
It is worth noting that placenta previa diagnosed before 20 weeks of pregnancy often resolves on its own. As the uterus grows, the placenta may move away from the cervix. Approximately 90% of cases diagnosed before 20 weeks resolve by the end of pregnancy.
Symptoms of Placenta Previa
The most common symptom of placenta previa is sudden, painless vaginal bleeding. The blood is usually bright red. Bleeding can appear as early as the 20th week of pregnancy, but it is more common in the third trimester.
The amount of bleeding can vary. It may be light at first, then stop, only to return more heavily within days or weeks. In addition, about 1 in 5 women with placenta previa also experiences uterine contractions, which can be a sign of preterm labour.
Some women with placenta previa have no symptoms at all. In these cases, the condition is often discovered during a routine ultrasound. It may also be found when an ultrasound is performed to investigate vaginal bleeding or when labour begins. Learn more about placenta previa symptoms and complications at Healthline.
How Placenta Previa Is Diagnosed
Ultrasound is the main tool used to diagnose placenta previa and low-lying placenta. It allows doctors to see exactly where the placenta is positioned in the uterus.
In some cases, a single ultrasound may not give a clear picture. A follow-up ultrasound may be needed to confirm the diagnosis. Fetal heart rate monitoring is also used to check on the baby’s health and wellbeing.
A vaginal examination is generally not recommended for women with placenta previa. Examining the cervix can disturb the placenta and cause serious bleeding. This is especially important if a caesarean section is not already planned in the near future.
Treatment Options for Placenta Previa
Treatment for placenta previa depends on several factors. These include how much bleeding is occurring, the mother’s overall health, the baby’s stage of development, and how much of the cervix the placenta is covering.
Watchful Waiting
If bleeding slows down or stops, doctors may recommend a period of watchful waiting. This means closely monitoring both the mother and baby while delaying delivery. If the baby is between 24 and 34 weeks of gestational age, corticosteroids may be given to help speed up the baby’s lung development and prepare for a possible early birth.
Additional supportive care may include iron supplements to treat or prevent anaemia, and a diet high in fibre or mild laxatives to prevent constipation.
Precautions for Non-Bleeding Cases
Women with placenta previa who are not actively bleeding are still advised to follow important safety guidelines. These precautions help reduce the risk of triggering a bleeding episode.
- Avoid intense physical activity, such as running or lifting anything heavier than about 9 kilograms
- Avoid sexual intercourse after 28 weeks of pregnancy (discuss risks with your doctor before that point)
- Do not use vaginal tampons or douches
- Avoid any vaginal examination unless your doctor specifically orders one
- Keep a phone nearby at all times in case of emergency
- Stay within a reasonable distance of a hospital that can care for both premature newborns and mothers
- Seek emergency care immediately if any vaginal bleeding begins
Hospital Care and Delivery
Women who are actively bleeding may need to be admitted to hospital for monitoring and treatment. A blood transfusion may be necessary in cases of heavy blood loss. Because vaginal delivery carries a high risk of severe bleeding when the placenta covers the cervix, a caesarean section is almost always the preferred method of delivery for placenta previa.
When possible, delivery is delayed until the baby’s lungs are fully mature. However, if the mother or baby is in danger, an early caesarean may be necessary. For more information on pregnancy complications, visit Health Canada’s guide to your health during pregnancy.
When to See a Doctor
If you experience any sudden vaginal bleeding during pregnancy, seek medical care right away. Do not wait to see if it stops on its own. This is a situation that needs immediate attention.
You can call your family doctor, visit a walk-in clinic, or go directly to your nearest hospital emergency department. If you have already been diagnosed with placenta previa, make sure your healthcare team knows so they can respond appropriately.
Even if you have no symptoms, speak with your family doctor or midwife about your risk factors at your next prenatal visit. Regular prenatal care is one of the best ways to catch complications early. Most provincial health plans in Canada cover prenatal ultrasounds, so make sure you attend all recommended appointments.
As always, consult your doctor or a qualified healthcare professional before making any decisions about your care during pregnancy.
Frequently Asked Questions About Placenta Previa
What are the main symptoms of placenta previa?
The most common symptom of placenta previa is sudden, painless, bright red vaginal bleeding during pregnancy. It can begin as early as 20 weeks but is more common in the third trimester. Some women also experience uterine contractions, while others have no symptoms at all.
Can placenta previa resolve on its own?
Yes, in many cases placenta previa diagnosed before 20 weeks of pregnancy can resolve on its own. As the uterus grows larger, the placenta may shift away from the cervix. Approximately 90% of early cases resolve by the end of pregnancy without intervention.
Is a caesarean section always required with placenta previa?
In most confirmed cases of placenta previa, a caesarean section is the recommended method of delivery. Vaginal delivery poses a serious risk of heavy bleeding when the placenta covers the cervix. Your doctor will assess your specific situation to determine the safest plan for you and your baby.
What increases the risk of developing placenta previa?
Several factors can raise the risk of placenta previa, including smoking during pregnancy, previous caesarean sections, prior uterine procedures like D&C, advanced maternal age, and having had multiple pregnancies. A previous diagnosis of placenta previa also increases the risk in future pregnancies.
How is placenta previa diagnosed in Canada?
Placenta previa is diagnosed using ultrasound, which allows doctors to see the exact position of the placenta in the uterus. Most provincial health plans in Canada cover routine prenatal ultrasounds. Your family doctor or midwife will refer you for imaging if they suspect a concern.
What should I do if I have bleeding during pregnancy?
According to Mayo Clinic’s guide to placenta previa, this information is supported by current medical research.
For more information, read our guide on mastitis treatment and causes for Canadian mothers.
Any vaginal bleeding during pregnancy should be treated as a medical emergency. Go to your nearest hospital emergency department, call your family doctor, or visit a walk-in clinic immediately. Do not wait to see if the bleeding stops, especially if you have been diagnosed with placenta previa.
Key Takeaways
- Placenta previa occurs when the placenta covers the cervix, affecting fewer than 1% of pregnancies
- The main symptom is sudden, painless, bright red vaginal bleeding, most often in the third trimester
- Risk factors include smoking, previous caesarean sections, multiple pregnancies, older maternal age, and prior uterine procedures
- Ultrasound is the standard tool used to diagnose placenta previa in Canada
- Many early cases resolve on their own as the uterus grows during pregnancy
- Treatment depends on the amount of bleeding, the baby’s development, and the mother’s health
- A caesarean section is usually required for delivery when placenta previa is confirmed
- Always speak with your family doctor, midwife, or healthcare provider about any concerns during pregnancy
Frequently Asked Questions
What is placenta previa?
Placenta previa is a pregnancy complication where the placenta partially or completely covers the cervical opening. This blocks the baby’s path during delivery and can cause serious bleeding. It affects approximately 1 in 200 pregnancies and is typically diagnosed through ultrasound during the second or third trimester.
What are the symptoms of placenta previa?
The most common symptom of placenta previa is sudden, painless bright red vaginal bleeding during the second or third trimester. Some women also experience cramping or contractions alongside bleeding. In some cases, there are no symptoms at all, and the condition is only discovered during a routine prenatal ultrasound.
How is placenta previa treated in Canada?
Treatment depends on severity, gestational age, and bleeding amount. Options include pelvic rest, hospitalization for monitoring, corticosteroid injections to mature the baby’s lungs, and planned Caesarean section delivery. Most Canadian hospitals recommend a C-section at 36–37 weeks for complete placenta previa to prevent life-threatening hemorrhage.
Can placenta previa be prevented?
Placenta previa cannot be fully prevented, as many risk factors are uncontrollable. However, avoiding smoking, limiting uterine surgeries, and spacing pregnancies appropriately may reduce risk. Known risk factors include previous C-sections, multiple pregnancies, advanced maternal age, and carrying multiples. Early prenatal care allows for timely detection and management.
When should I see a doctor for vaginal bleeding during pregnancy?
Seek emergency medical care immediately if you experience any vaginal bleeding during pregnancy, especially if it is painless and bright red. Do not wait to see if bleeding stops on its own. In Canada, go to your nearest emergency department or call 911, as bleeding may indicate placenta previa or another serious complication.
About the Author
Dr. Sarah Mitchell, MDDr. Sarah Mitchell is a board-certified family physician with over 15 years of clinical experience. She completed her MD at the University of Toronto and her residency at Toronto General Hospital. Dr. Mitchell specializes in preventive medicine and chronic disease management. She is a member of the College of Family Physicians of Canada (CFPC) and has published over 30 peer-reviewed articles on preventive health care.
View all articles →