Cholesteatoma: Causes, Symptoms & Treatment in Canada
Share
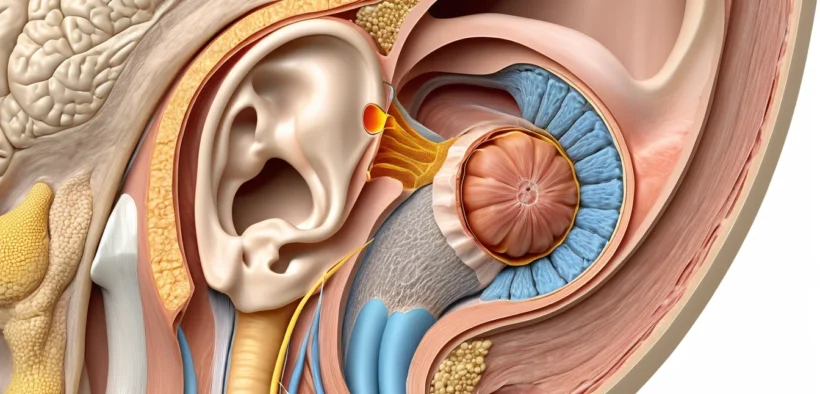
A cholesteatoma is an abnormal skin cyst that develops inside the middle ear and can silently destroy the delicate bone structures surrounding your ear and brain. While the name may not sound alarming, this condition can lead to permanent hearing loss and life-threatening infections without timely intervention. Understanding the warning signs early is critical for Canadians who want to protect their long-term hearing health.
What Is a Cholesteatoma and Why Is It Dangerous?
Recognizing cholesteatoma symptoms — such as persistent foul-smelling ear discharge, gradual hearing loss, and recurring ear infections — can make a real difference in your outcome. In Canada, this condition is treated by ENT (ear, nose, and throat) specialists, and surgical removal is typically covered by provincial health plans. This guide explains the causes, diagnosis, and treatment options available to help you take the right steps toward recovery.
What Is a Cholesteatoma?
| Treatment Option | Description & Benefits | Considerations & Risks | Typical Outcome |
|---|---|---|---|
| Canal Wall Up Mastoidectomy (CWU) | Removes cholesteatoma while preserving the ear canal wall; better cosmetic result and easier hearing aid fitting post-surgery | Higher recurrence rate (up to 30–40%); requires regular follow-up imaging (MRI) and possible second-look surgery | Good hearing preservation in many cases; ongoing monitoring required for at least 5 years |
| Canal Wall Down Mastoidectomy (CWD) | Removes the posterior canal wall creating an open mastoid cavity; lowers recurrence risk significantly | Requires lifelong annual ear cleaning by an ENT specialist; water precautions needed; larger cavity can collect debris | Lower recurrence rate; hearing outcomes vary; widely performed across Canadian ENT centres |
| Tympanoplasty (Eardrum Repair) | Reconstructs the eardrum following cholesteatoma removal; often combined with mastoidectomy to restore hearing | May require a second staged procedure; success depends on extent of middle ear damage and ossicle involvement | Hearing improvement in 60–80% of cases when ossicles are intact or reconstructed |
| Ossicular Chain Reconstruction | Rebuilds damaged hearing bones (ossicles) destroyed by cholesteatoma using prostheses or cartilage grafts | Often performed as a second-stage procedure 6–12 months after initial surgery; outcomes depend on middle ear health | Meaningful hearing improvement in many patients; prosthesis extrusion is a possible long-term complication |
| Watchful Waiting & Antibiotic Ear Drops | Used temporarily to control infection and reduce inflammation before surgery; not a curative option for cholesteatoma | Cholesteatoma will continue to grow without surgical removal; risk of serious complications including meningitis increases over time | Symptom relief only; all confirmed cholesteatoma cases in Canada are ultimately referred for surgical management |
A cholesteatoma is a cyst made up of squamous (skin-like) tissue that forms inside the skull base, usually in the middle ear. Because bone is rigid and cannot simply stretch, the cyst grows by eroding the surrounding bone. This is what makes it so dangerous.
As the cyst expands, it can damage important structures inside the temporal bone — the part of the skull that houses your hearing and balance organs. In severe cases, it can expose the brain’s protective lining, known as the dura mater. According to Mayo Clinic, cholesteatoma is a well-recognized cause of serious ear complications if left untreated.
The bone erosion happens in two main ways. First, the constant pressure from the growing cyst wears bone down over time. Second, the cyst triggers enzyme activity that speeds up bone breakdown, especially when the cyst becomes infected.
Types of Cholesteatoma
Congenital Cholesteatoma
A congenital cholesteatoma is present from birth. It forms when squamous tissue gets trapped inside the temporal bone during fetal development. This type usually shows up in children between six months and five years of age.
Congenital cholesteatoma typically sits near the front of the middle ear, close to the Eustachian tube. As it grows, it can block the tube and cause fluid to build up in the middle ear. This leads to hearing loss caused by poor sound conduction.
However, unlike other types, congenital cholesteatoma does not damage the eardrum. Children with this type also rarely have a history of repeated ear infections or a perforated eardrum.
Acquired Cholesteatoma
Acquired cholesteatoma develops later in life. It is the more common form, and it comes in two subtypes: primary and secondary.
Primary acquired cholesteatoma results from a retracted eardrum. When the Eustachian tube does not work properly, it creates negative pressure in the middle ear. This negative pressure pulls the eardrum inward, which can eventually lead to cyst formation. Over time, the cyst can erode the small hearing bones (ossicles), the mastoid bone, and even the semicircular canals responsible for balance. This can cause dizziness and significant hearing loss.
Secondary acquired cholesteatoma develops after the eardrum is damaged. A perforated eardrum — caused by a middle ear infection, injury, or even a medical procedure — can allow skin cells to enter the middle ear. Interestingly, even a minor procedure like placing a tympanostomy tube (ear tube) carries a small risk of introducing skin tissue into the middle ear. Posterior perforations near the edge of the eardrum carry the highest risk.
What Causes a Cholesteatoma?
Poor Eustachian tube function is the most common underlying cause of acquired cholesteatoma. The Eustachian tube connects your middle ear to the back of your throat, helping equalize pressure. When it does not work well, pressure imbalances develop inside the ear.
This ongoing negative pressure slowly pulls the eardrum inward. Over time, the retracted eardrum forms a pocket that traps dead skin cells. That pocket can fill with skin debris, metabolic waste, and fluid — forming the cyst. If the cyst becomes infected, it grows faster and can cause rapid damage.
In addition, chronic ear infections that are left untreated increase the risk significantly. Healthline notes that repeated middle ear infections are a well-known risk factor for developing this condition.
Symptoms of Cholesteatoma
Recognizing cholesteatoma symptoms early gives you the best chance at a good outcome. The symptoms can be subtle at first, but they tend to worsen as the cyst grows.
The most telling symptom is a painless discharge from the ear that keeps coming back. This discharge is often yellowish-brown in colour and has a strong, unpleasant smell. It does not respond well to standard ear infection treatments.
Common symptoms include:
- Persistent or recurring ear discharge — often foul-smelling and yellowish in colour
- Hearing loss — more noticeable as the cyst grows larger and damages the hearing bones
- Dizziness or vertigo — occurs when the cyst erodes the bone near the balance canals
- Tinnitus — a ringing, buzzing, or humming sound in the ear
- Facial muscle weakness or numbness — this signals damage near the facial nerve, which runs through the temporal bone
- Ear pain or headache — especially in more advanced cases
Therefore, if you notice any of these symptoms — especially ongoing ear discharge — you should seek medical attention promptly. Do not assume it is just a simple ear infection.
How Is Cholesteatoma Diagnosed?
Diagnosis begins with a thorough medical history and physical examination. Your doctor will examine your ear canal and eardrum carefully using an otoscope, a lighted instrument designed for ear exams. A perforated eardrum or visible debris in the middle ear is found in more than 90% of cases.
Further tests may include:
- CT scan (computed tomography) — provides detailed images of the temporal bone to assess the extent of bone erosion
- Hearing tests (audiometry) — measure how much hearing has been affected and what type of hearing loss is present
- Balance testing (electronystagmography) — evaluates the balance system when dizziness is a symptom
In Canada, your family doctor can refer you for these tests through your provincial health plan. If your family doctor is not immediately available, a walk-in clinic can assess your ear symptoms and provide a referral to an ear, nose, and throat (ENT) specialist. For more information on navigating specialist referrals in Canada, visit Health Canada’s official health resources.
Treatment Options for Cholesteatoma
Surgery is the only effective treatment for cholesteatoma. The goal is to completely remove the cyst and prevent it from coming back. Leaving any cyst tissue behind can lead to regrowth.
The type of surgery depends on the size and location of the cholesteatoma. Common surgical approaches include:
- Mastoidectomy — removal of infected bone cells in the mastoid area behind the ear
- Tympanoplasty — reconstruction of the eardrum after surgery
- Ossiculoplasty — repair or replacement of the small hearing bones that may have been damaged
Recovery time varies. Your ENT specialist will monitor you closely after surgery to check for any signs of regrowth. Follow-up appointments are essential, as cholesteatoma can return even after a successful operation.
In cases where surgery is delayed or the cyst becomes infected, doctors may first prescribe antibiotics and ear drops to control the infection. However, these medications do not eliminate the cyst itself. Surgery is still required.
Possible Complications If Left Untreated
A cholesteatoma that is not treated can cause serious and permanent damage. The longer it grows, the more structures it can destroy. Complications can include:
- Permanent hearing loss
- Damage to the facial nerve, causing weakness or paralysis on one side of the face
- Chronic dizziness or balance problems
- Meningitis — a dangerous infection of the brain’s protective lining
- Brain abscess — a collection of infection inside the brain
- Spread of infection to the neck or nervous system
Furthermore, in neglected cases, the growing cyst can press directly on brain tissue. This makes early diagnosis and prompt treatment absolutely critical.
When to See a Doctor
You should see your family doctor if you notice ear discharge that keeps returning, especially if it smells unpleasant. Do not wait to see if it clears up on its own. Cholesteatoma does not go away without medical intervention.
If your family doctor is unavailable, visit a walk-in clinic as soon as possible. Bring a list of your symptoms, including when they started and whether you have had previous ear infections or ear surgery. Your doctor will likely refer you to an ENT specialist for further evaluation.
Seek emergency care immediately if you experience sudden severe headache, facial drooping, high fever with ear pain, or significant changes in vision or balance. These could signal a serious complication that requires urgent attention.
Always speak with a qualified healthcare provider before making any decisions about your ear health. This article is for informational purposes only and is not a substitute for professional medical advice.
Frequently Asked Questions About Cholesteatoma
Is a cholesteatoma a type of cancer?
No, a cholesteatoma is not cancerous. It is a non-cancerous cyst made of skin cells that grows in the wrong location — inside the middle ear. However, it can still cause serious damage to surrounding structures if left untreated, so prompt medical care is important.
Can a cholesteatoma go away on its own?
No, a cholesteatoma cannot go away on its own. It will continue to grow and erode surrounding bone without surgical treatment. Antibiotics can help manage infections associated with the cyst, but they cannot remove the cholesteatoma itself.
What does cholesteatoma discharge look, smell, and feel like?
The discharge from a cholesteatoma is typically yellowish-brown in colour and has a strong, foul odour. It is usually painless and tends to keep coming back even after treatment with ear drops. This persistent, smelly ear discharge is often the first sign that prompts people to see a doctor.
How common is cholesteatoma in Canada?
The exact incidence of cholesteatoma in Canada is not precisely tracked, but it is a recognized condition that leads to a significant number of ear, nose, and throat surgeries each year. Both children and adults can develop cholesteatoma, though congenital cases appear in early childhood and acquired cases are more common in adults.
Can cholesteatoma come back after surgery?
Yes, cholesteatoma can recur after surgery if any cyst tissue is left behind. This is why regular follow-up appointments with your ENT specialist are so important after treatment. In some cases, a second surgery may be needed to fully remove any remaining or regrown tissue.
Is cholesteatoma surgery covered by provincial health plans in Canada?
According to Mayo Clinic’s overview of cholesteatoma, this information is supported by current medical research.
For more information, read our guide on signs and symptoms you should never ignore.
In most cases, yes. Cholesteatoma surgery is considered medically necessary, and it is generally covered under provincial and territorial health insurance plans across Canada. Your family doctor or ENT specialist can provide a referral and guide you through the process in your province.
Key Takeaways
- A cholesteatoma is a non-cancerous but destructive skin cyst that grows inside the middle ear.
- It can be congenital (present from birth) or acquired (developing later due to ear infections, injury, or Eustachian tube problems).
- Key symptoms include persistent foul-smelling ear discharge, hearing loss, dizziness, tinnitus, and facial weakness.
- Diagnosis involves a physical ear exam, CT scan, and hearing tests — all accessible through your provincial health plan with a referral.
- Surgery is the only effective treatment. Early intervention leads to much better outcomes.
- Left untreated, cholesteatoma can cause permanent hearing loss, facial nerve damage, meningitis, or brain abscess.
- If you notice recurring ear discharge or unexplained hearing changes, see your family doctor or visit a walk-in clinic promptly.
Frequently Asked Questions
What is a cholesteatoma?
A cholesteatoma is an abnormal, noncancerous skin growth that develops in the middle ear, behind the eardrum. It typically forms due to repeated ear infections or Eustachian tube dysfunction. If left untreated, it can expand and erode surrounding bone, potentially causing hearing loss, infection, or serious complications.
What are the symptoms of cholesteatoma?
Common symptoms include a persistent, foul-smelling ear discharge, progressive hearing loss, and a feeling of fullness or pressure in the ear. Some people experience earache, dizziness, or tinnitus. Symptoms often develop gradually and may worsen over time as the growth enlarges and damages middle ear structures.
How is cholesteatoma treated in Canada?
Cholesteatoma is primarily treated through surgery, typically a procedure called a mastoidectomy or tympanoplasty, performed by an ENT (ear, nose, and throat) specialist. Surgery removes the growth and repairs damaged structures. In Canada, this is covered under provincial health plans. Early treatment prevents serious complications like hearing loss or meningitis.
Can cholesteatoma be prevented?
There is no guaranteed way to prevent cholesteatoma, but reducing risk factors helps. Promptly treating ear infections, managing Eustachian tube dysfunction, and addressing chronic negative ear pressure can lower your risk. Children with recurring ear infections or who require ear tubes should be monitored regularly by a healthcare provider.
When should I see a doctor about ear symptoms?
See a doctor if you experience persistent ear discharge, unexplained hearing loss, chronic ear pain, or dizziness lasting more than a few days. These symptoms may indicate cholesteatoma or another serious ear condition. Early diagnosis is critical, as untreated cholesteatoma can lead to permanent hearing damage or life-threatening complications.
About the Author
Dr. Linda Chen, RD, PhDDr. Linda Chen is a registered dietitian and PhD in Nutritional Sciences from the University of British Columbia. With expertise in clinical nutrition, sports dietetics, and gut health, she has worked with leading Canadian hospitals and sports organizations. Dr. Chen is a member of Dietitians of Canada and regularly contributes to national nutrition policy discussions.
View all articles →